## Clinical Diagnosis: DIC with ARDS in Malignancy ### Pathophysiologic Context **Key Point:** Solid tumors, particularly pancreatic and lung cancers, are potent triggers of DIC through release of tissue factor (TF) and cancer procoagulant from tumor cells and tumor-associated macrophages. Pancreatic adenocarcinoma has one of the highest DIC incidences among solid malignancies (up to 50–70% in advanced disease). Metastatic burden amplifies procoagulant activity, leading to systemic activation of coagulation and consumption of platelets, fibrinogen, and clotting factors. ### ISTH DIC Scoring: Overt DIC Confirmed | Component | Value | Points | |-----------|-------|--------| | Platelet count | 32,000/μL | +1 | | D-dimer/FDP elevation | 8.5 μg/mL (markedly elevated) | +3 | | PT prolongation | 22 sec (+10 sec above control) | +1 | | Fibrinogen | 78 mg/dL (<100 mg/dL) | +1 | | **Total Score** | — | **≥6 (overt DIC)** | ### Multi-Organ Involvement: DIC Manifestations 1. **Pulmonary:** Bilateral infiltrates + hemoptysis + hypoxemia → **DIC-induced ARDS** - Microthrombi in pulmonary capillaries → capillary leak, pulmonary edema - Platelet and fibrin deposition → acute lung injury 2. **Hematologic:** Thrombocytopenia (32,000) + anemia (Hb 8.9) → consumption coagulopathy 3. **Bleeding:** Gum oozing, dark urine (hematuria) → factor depletion + microthrombi 4. **Hemodynamic:** Hypotension (88/54), tachycardia (126), tachypnea (28) → sepsis-like state, tissue hypoperfusion **High-Yield:** The triad of **advanced malignancy + coagulopathy + bilateral pulmonary infiltrates** is classic for DIC-ARDS. ### Pathophysiology of DIC-ARDS ```mermaid flowchart TD A[Pancreatic adenocarcinoma]:::outcome --> B[Release of tissue factor & cancer procoagulant]:::outcome B --> C[Systemic coagulation activation]:::action C --> D[Platelet & fibrinogen consumption]:::outcome C --> E[Fibrin microthrombi formation]:::outcome E --> F[Pulmonary capillary occlusion]:::outcome F --> G[Capillary leak & endothelial injury]:::outcome G --> H[ARDS]:::urgent D --> I[Thrombocytopenia & hypofibrinogenemia]:::outcome I --> J[Bleeding manifestations]:::urgent C --> K[Factor consumption]:::outcome K --> L[Prolonged PT/aPTT]:::outcome ``` ### Management Strategy 1. **Supportive care (first-line):** - Platelet transfusion (target >20,000/μL for bleeding; >50,000/μL for ARDS) - FFP + cryoprecipitate for fibrinogen replacement - Mechanical ventilation for ARDS (lung-protective strategy) 2. **Anticoagulation (controversial but considered):** - Low-dose unfractionated heparin (5–10 units/kg/hr) to block ongoing thrombin generation - Rationale: Prevent further microthrombi formation while supporting bleeding with transfusions 3. **Treat underlying malignancy:** - Palliative chemotherapy or clinical trial enrollment - DIC often signals end-stage disease; prognosis poor **Clinical Pearl:** DIC in solid tumors carries a mortality rate of 40–60% despite aggressive supportive care. The presence of ARDS worsens prognosis further. Definitive treatment of the cancer (if feasible) is the only way to halt DIC progression. 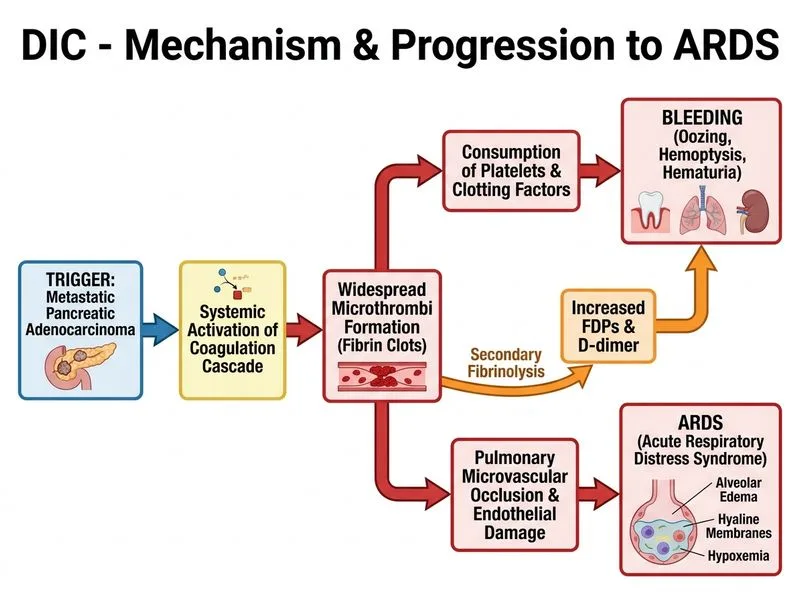
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.