## Clinical Scenario Analysis This is a **predicted difficult airway with an intra-operative complication** during the planned rescue technique. Key facts: - Patient is awake, spontaneously ventilating, and oxygenating well - Epistaxis is a known complication of nasal fiberoptic intubation (incidence 5–30%) - The left nostril remains available - Trismus precludes oral fiberoptic as a practical alternative ## Difficult Airway Algorithm — Awake Intubation Complication Management ```mermaid flowchart TD A[Awake fiberoptic intubation planned]:::outcome --> B[Epistaxis during nasal approach]:::urgent B --> C{Patient stable & oxygenating?}:::decision C -->|Yes| D[Manage epistaxis: topical epinephrine, gentle suction]:::action D --> E[Attempt contralateral nostril]:::action E --> F{Success?}:::decision F -->|Yes| G[Proceed with intubation]:::action F -->|No| H[Wake patient, plan alternative]:::action C -->|No| I[Emergency surgical airway]:::urgent ``` ## High-Yield Management of Nasal Epistaxis During Fiberoptic Intubation | Intervention | Rationale | Evidence | |--------------|-----------|----------| | **Topical epinephrine (1:10,000)** | Vasoconstriction; reduces bleeding | Standard of care; reduces epistaxis by ~60% | | **Gentle suctioning** | Clears blood, improves visualization | Avoid aggressive suctioning (worsens bleeding) | | **Contralateral nostril** | Avoids re-traumatizing bleeding site | First-line salvage in unilateral epistaxis | | **Posterior packing** | Reserved for severe, uncontrolled bleeding | Not needed if contralateral nostril patent | ## Key Point: **In a stable, oxygenating patient with unilateral epistaxis, attempt the contralateral nostril after topical hemostasis.** This is a minor complication with a simple solution — do not abandon awake intubation prematurely. ## Clinical Pearl: **Epistaxis during nasal fiberoptic intubation is common and usually self-limited.** The key is gentle technique, adequate topicalization with epinephrine, and willingness to switch nostrils. Most cases resolve without aborting the procedure. ## Why Each Distractor Fails: **Oral fiberoptic despite trismus (Option 1):** Trismus of 1.5 cm makes oral fiberoptic technically impossible — the scope cannot be advanced. This is not a viable alternative. **Abort and reschedule for awake tracheostomy (Option 2):** Premature abandonment of a salvageable situation. The patient is stable and oxygenating; a minor epistaxis does not warrant aborting elective surgery and committing to tracheostomy (which has its own morbidity). Tracheostomy is a last resort, not a first response to epistaxis. **Rapid sequence induction with video laryngoscope (Option 3):** Dangerous. The patient has OSMF and trismus — predicted difficult airway. RSI removes spontaneous ventilation and commits you to intubation in a patient you have already identified as difficult. This violates the fundamental principle: **awake intubation is mandatory in predicted difficult airways.** RSI is contraindicated. ## Warning: **Do NOT abandon awake intubation in a predicted difficult airway because of a minor, manageable complication.** Epistaxis is expected in 5–30% of nasal fiberoptic intubations; it is not a reason to switch to RSI. 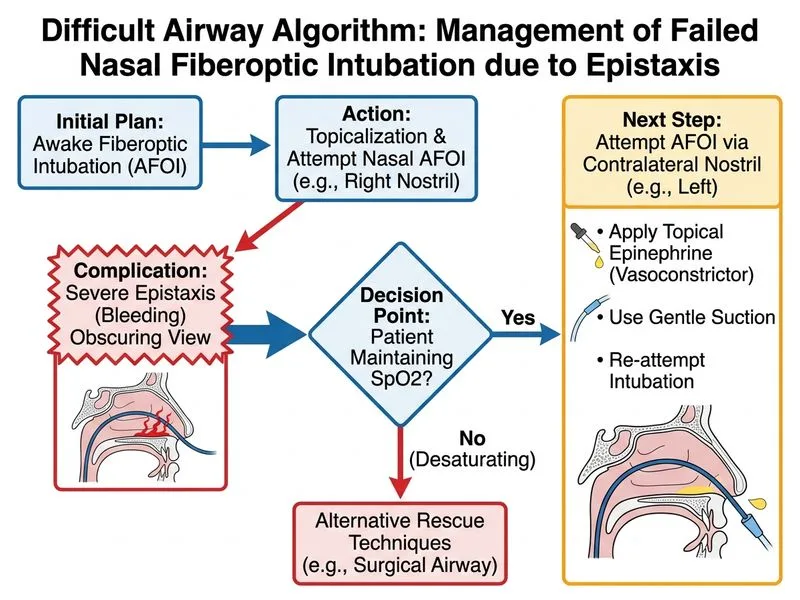
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.