## Difficult Airway Algorithm — Predicted Difficult Airway with Adequate Ventilation ### Clinical Context This is a **predicted difficult airway** (laryngeal papillomatosis with 60% obstruction) encountered after inhalational induction. The patient has **failed direct laryngoscopy** but **bag-mask ventilation remains adequate**. This is the classic "cannot intubate, CAN ventilate" scenario in the ASA Difficult Airway Algorithm. ### Key Distinction: Adequate Ventilation Changes Strategy **Key Point:** When bag-mask ventilation is adequate despite failed direct laryngoscopy, the priority is **NOT emergency surgical airway**, but rather **maintaining oxygenation and planning a controlled, visualized intubation technique** (ASA Difficult Airway Algorithm, 2022 update). ### Correct Approach: Call for Help, Maintain Oxygenation, Plan Advanced Airway 1. **Call for help** — senior anesthesiologist, ENT surgeon (essential in RRP cases) 2. **Maintain oxygenation** — continue bag-mask ventilation with 100% O₂; do not allow desaturation 3. **Plan rescue intubation** — **fiberoptic intubation** (allows direct visualization around papillomas, universally available) OR **rigid bronchoscopy** (allows simultaneous visualization and debulking by ENT when available) 4. **Consider LMA as a bridge** — if fiberoptic is unavailable, an LMA can maintain the airway temporarily while awaiting ENT or fiberoptic equipment ### Fiberoptic Intubation vs. Rigid Bronchoscopy in RRP Both are valid and equally important approaches: | Technique | Advantages | Considerations | |---|---|---| | **Fiberoptic intubation** | Universally available; direct visualization; avoids blind passage | Papillomas may obscure view; friable tissue may bleed | | **Rigid bronchoscopy (ENT)** | Simultaneous debulking/laser ablation; passage of larger ETT after debulking | Requires ENT availability; more invasive | **High-Yield:** In RRP with laryngeal obstruction, fiberoptic intubation is the most universally applicable first-line advanced technique. Rigid bronchoscopy with ENT is an equally important alternative, often preferred when ENT expertise is immediately available as it allows simultaneous debulking of papillomas. The choice depends on institutional resources and ENT availability — neither technique is universally superior (Difficult Airway Society Guidelines 2015; ASA Difficult Airway Algorithm 2022; Miller's Anesthesia, 9th ed.). **Clinical Pearl:** RRP is a contraindication to aggressive blind intubation attempts. Papillomas are friable and bleed easily; repeated blind attempts can cause hemorrhage, further airway compromise, and seeding of papillomatous tissue into the lower airways. Visualized techniques are mandatory. ### Why Not Emergency Cricothyrotomy (Option D)? - Bag-mask ventilation is adequate — cricothyrotomy is reserved for "cannot intubate, cannot oxygenate" (CICO) scenarios - Cricothyrotomy risks seeding papillomas into the trachea and subglottis in RRP - Premature surgical airway violates the ASA algorithm when oxygenation is maintained ### Why Not LMA Alone and Proceed with Surgery (Option A)? - An LMA does NOT secure the trachea against aspiration during abdominal surgery (hysterectomy) - LMA may be used as a **temporary bridge** to fiberoptic intubation, but not as the definitive airway for this procedure - Proceeding with surgery without a secured airway in a patient with 60% laryngeal obstruction is unsafe ### Why Not Smaller Endotracheal Tube (Option B)? - Blind passage of any tube through papillomas risks trauma, hemorrhage, and aspiration of papillomatous tissue - A 6.0 mm tube may not pass even with force; forcing risks airway rupture and worsening obstruction - This violates the principle of avoiding repeated blind attempts in a known difficult airway [cite: ASA Difficult Airway Algorithm 2022; Difficult Airway Society Guidelines 2015; Miller's Anesthesia, 9th ed., Chapter on Airway Management] 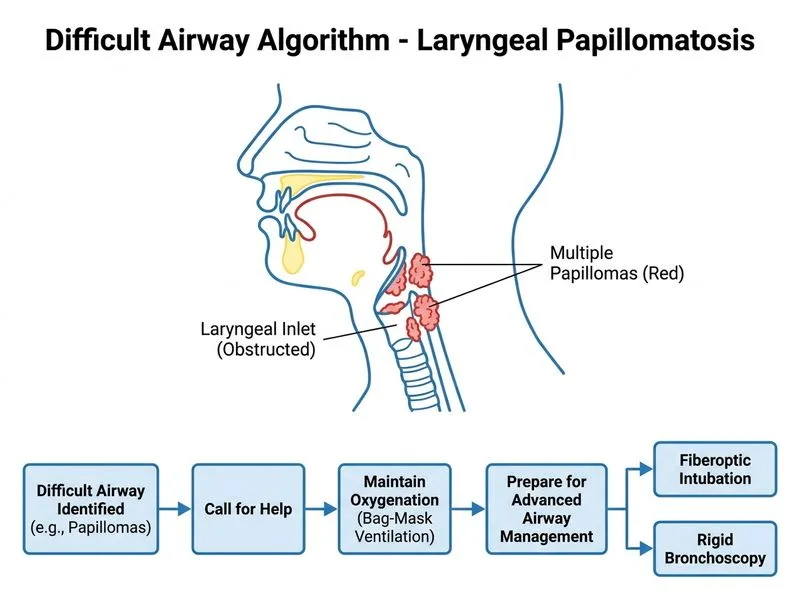
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.