## Gold Standard Status and Complication Profile of Digital Subtraction Angiography ### Role of DSA in Peripheral Arterial Disease **Key Point:** Digital subtraction angiography remains the gold standard for diagnosis and hemodynamic assessment of peripheral arterial disease, with the unique advantage of allowing **real-time intervention** (percutaneous transluminal angioplasty, stenting) in the same session. ### Sensitivity and Specificity DSA has a sensitivity and specificity both >95% for detecting significant stenosis (>50%) in peripheral arteries [cite:Robbins 10e Ch 11]. This is superior to duplex ultrasonography (which has ~85% sensitivity) and comparable to CT angiography, though CT is increasingly used as a first-line non-invasive modality. ### Complication Rate and Types **High-Yield:** The overall complication rate of DSA is **0.5–2%**, with the following breakdown: | Complication | Incidence | Mechanism | | --- | --- | --- | | Contrast-induced nephropathy (CIN) | 0.3–1% | Osmotic diuresis + tubular toxicity | | Arterial dissection | 0.1–0.5% | Catheter trauma during manipulation | | Atheroemboli | 0.1–0.3% | Dislodgement of plaque during instrumentation | | Hematoma at access site | 0.5–1% | Puncture site bleeding | | Allergic reaction to contrast | <0.1% | Type I hypersensitivity | **Clinical Pearl:** The risk of CIN is higher in patients with **pre-existing renal impairment, diabetes, and dehydration**—not an absolute contraindication, but requires hydration protocols and careful monitoring. ### Management in Renal Impairment **Warning:** While DSA carries a real risk of CIN in patients with eGFR <30 mL/min/1.73 m², it is **NOT absolutely contraindicated**. The actual incidence of CIN in this population is 10–20%, not >40%. The key is: 1. Pre-procedure hydration (normal saline 1 mL/kg/hr for 12 hrs pre- and post-procedure) 2. Use of iso-osmolar or low-osmolar contrast media (LOCM) 3. Consideration of non-invasive alternatives (CT angiography, MR angiography) if intervention is not planned 4. Monitoring of creatinine at 48–72 hours post-procedure ### Diabetes and Hypertension Diabetic patients with hypertension are at **higher risk** for atherosclerotic disease and complications, but DSA is **not contraindicated**. The risk of atheroemboli is not >60% higher—it is modestly elevated (relative risk ~1.5–2) due to greater atherosclerotic burden, not the combination of diabetes and hypertension per se. ### Why Option 1 Is Incorrect DSA sensitivity for >50% stenosis is >95%, not 85%. Additionally, DSA is **inferior** to CT angiography in detecting **calcified lesions** because heavy calcification causes beam hardening artifacts on DSA; CT is actually superior in this regard. ### Why Option 2 Is Correct This statement accurately reflects the current evidence: DSA is the gold standard for both diagnosis and intervention, with a well-established complication rate of 0.5–2%, and the major complications (CIN, dissection) are correctly identified. ### Why Option 3 Is Incorrect While CIN risk is real in eGFR <30, the incidence is 10–20%, not >40%. DSA is not contraindicated; it is performed with appropriate precautions (hydration, LOCM, monitoring). ### Why Option 4 Is Incorrect Diabetes and hypertension are risk factors for atherosclerotic disease, but they do not contraindicate DSA. The risk of atheroemboli is not elevated by >60% in this combination; it is modestly elevated due to atherosclerotic burden alone. ```mermaid flowchart TD A[Suspected PAD]:::outcome --> B{Non-invasive imaging first}:::decision B -->|Duplex US or CTA| C[Diagnosis confirmed?]:::decision C -->|Yes, intervention planned| D[DSA + intervention]:::action C -->|Yes, no intervention| E[Medical management]:::action D --> F{Renal function?}:::decision F -->|eGFR >30| G[Standard protocol]:::action F -->|eGFR 15-30| H[Hydration + LOCM + monitoring]:::action F -->|eGFR <15| I[Consider non-invasive alternative]:::decision G --> J[Proceed with DSA]:::action H --> J I --> K{Intervention essential?}:::decision K -->|Yes| J K -->|No| E J --> L[Complication rate 0.5-2%]:::outcome ``` ## Summary **Key Point:** DSA is the gold standard for PAD diagnosis and intervention. While it carries real risks (CIN 0.3–1%, dissection 0.1–0.5%, atheroemboli 0.1–0.3%), these are manageable with appropriate patient selection and periprocedural protocols. Diabetes and renal impairment increase risk but do not contraindicate the procedure. 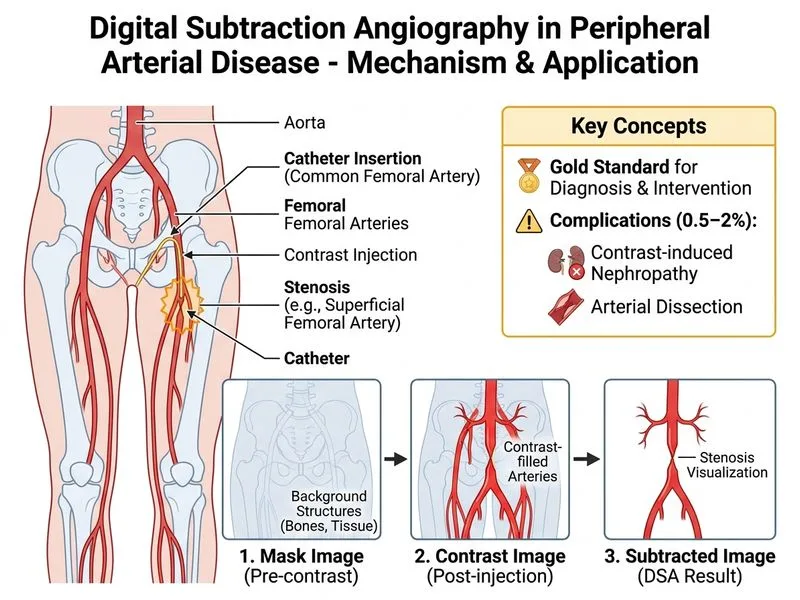
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.