## Clinical Diagnosis: Diphtheria **Key Point:** The hallmark of diphtheria is a thick, adherent, greyish-white pseudomembrane that does not blanch and bleeds on removal—pathognomonic findings in this case. ### Pathophysiology Diphtheria is caused by *Corynebacterium diphtheriae*, which produces a potent exotoxin (diphtheria toxin) that inhibits protein synthesis via inactivation of elongation factor-2. The membrane consists of fibrin, dead epithelial cells, and bacteria, and is firmly adherent to the underlying mucosa. ### Clinical Features Present in This Case - **Pseudomembrane:** Greyish-white, thick, adherent, does not blanch, bleeds on removal - **Systemic signs:** Low-grade fever, sore throat, dysphagia - **Cervical lymphadenopathy with neck edema:** "Bull neck" appearance (early sign) - **Tachycardia and tachypnea:** Suggest systemic toxemia - **Unvaccinated status:** Major risk factor in endemic regions ### Most Important Immediate Intervention **High-Yield:** Diphtheria antitoxin (DAT) must be administered **immediately, without waiting for culture or PCR confirmation**. Delaying antitoxin administration increases the risk of myocarditis, neuritis, and death. The antitoxin is effective only against circulating toxin, not toxin already bound to tissues—hence early administration is critical. **Clinical Pearl:** Culture confirmation typically takes 24–48 hours. The clinical diagnosis alone (pseudomembrane + systemic features) is sufficient to initiate antitoxin therapy in endemic areas. ### Management Algorithm ```mermaid flowchart TD A[Suspected Diphtheria<br/>Pseudomembrane + Systemic Signs]:::outcome --> B[Administer DAT immediately<br/>without waiting for culture]:::action B --> C[Send throat/nasopharyngeal swab<br/>for culture & PCR]:::action C --> D[Start antibiotics<br/>Penicillin G or Erythromycin]:::action D --> E[Monitor for complications<br/>Myocarditis, Neuritis]:::decision E -->|Cardiac involvement| F[ECG, Troponin, Supportive care]:::action E -->|Neurological involvement| G[Cranial nerve palsies<br/>Respiratory muscle paralysis]:::urgent ``` ### Dosing of Diphtheria Antitoxin - **Dose:** 20,000–100,000 units IV or IM (depending on severity and duration of illness) - **Route:** IV preferred for rapid systemic distribution - **Timing:** Within 24–48 hours of symptom onset for maximum efficacy ### Antibiotic Therapy (After Antitoxin) 1. **Penicillin G:** 50,000 units/kg/day IV in divided doses (preferred) 2. **Erythromycin:** 40–50 mg/kg/day orally in divided doses (alternative) 3. **Duration:** 7–10 days ### Complications to Monitor | Complication | Timing | Mechanism | Management | |---|---|---|---| | **Myocarditis** | 1–3 weeks | Toxin-mediated cardiac damage | ECG, troponin, supportive care, arrhythmia management | | **Cranial nerve palsies** | 2–6 weeks | Demyelination of motor nerves | Supportive care, respiratory support if needed | | **Respiratory paralysis** | 3–4 weeks | Involvement of phrenic & intercostal nerves | Mechanical ventilation | | **Airway obstruction** | Early | Membrane extension, edema | Airway management, possible tracheostomy | **Mnemonic — Complications of Diphtheria: CARD** - **C**ranial nerve palsies (palatal, pharyngeal, laryngeal) - **A**irway obstruction - **R**espiratory paralysis (phrenic nerve) - **D**ilatation of heart (myocarditis, cardiomegaly) ### Why Antitoxin Without Culture Confirmation? **High-Yield:** The clinical diagnosis of diphtheria in an endemic setting is sufficiently specific to justify immediate antitoxin administration. Waiting for culture results delays therapy and increases mortality. Antitoxin is safe and specific; the risk of withholding it far outweighs the risk of administering it for a misdiagnosis. [cite:Park 26e Ch 8] 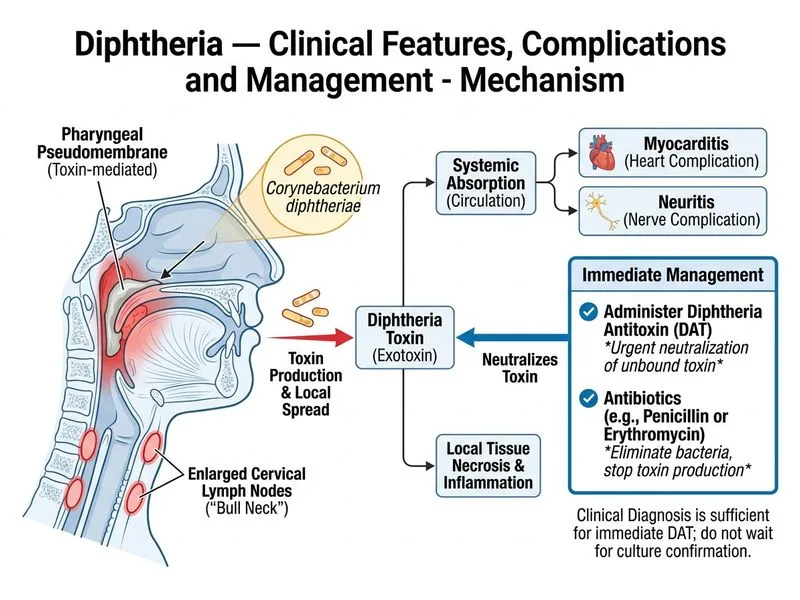
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.