## Management of Diphtheria with Early Myocardial Involvement ### Clinical Assessment of This Case **Key Point:** The combination of tachycardia (120/min), hypotension (95/60 mmHg), tachypnea (32/min), and marked cervical edema in a child on day 5 of illness suggests **early myocarditis**—a life-threatening complication of diphtheria. ### Pathophysiology of Diphtheria Myocarditis The diphtheria toxin causes: 1. **Direct myocardial damage:** Inhibition of protein synthesis → myocyte necrosis 2. **Conduction abnormalities:** Demyelination of cardiac conduction pathways 3. **Arrhythmias:** Ranging from bradycardia to complete heart block 4. **Cardiogenic shock:** From reduced cardiac output and peripheral vasodilation ### Clinical Features of Myocarditis in This Case | Finding | Significance | |---|---| | **Tachycardia (120/min)** | Compensatory response to reduced cardiac output; early sign | | **Hypotension (95/60)** | Indicates hemodynamic compromise; suggests cardiogenic shock | | **Tachypnea (32/min)** | Pulmonary edema or metabolic acidosis from shock | | **Marked neck edema** | Venous congestion from right heart failure | | **Day 5 of illness** | Myocarditis typically develops 2–6 weeks after symptom onset, but early severe cases can present by day 5 | ### Why Continuous Cardiac Monitoring and Inotropic Support? **High-Yield:** Diphtheria myocarditis is the leading cause of death in diphtheria (accounts for 50–90% of mortality). Early recognition and aggressive hemodynamic support can prevent progression to cardiogenic shock and death. **Clinical Pearl:** The presence of hypotension in a child with diphtheria is a medical emergency requiring: 1. **Continuous ECG monitoring** to detect arrhythmias, conduction blocks, and ischemic changes 2. **Inotropic support** (dopamine, dobutamine, or epinephrine) to maintain perfusion pressure 3. **Fluid management:** Cautious IV fluids (avoid overload in heart failure) 4. **Serial troponin and BNP** to assess myocardial injury ### Management Algorithm for Diphtheria with Myocarditis ```mermaid flowchart TD A[Diphtheria with Hemodynamic Compromise<br/>HR >120, BP <95/60, RR >30]:::urgent --> B[Establish IV access<br/>Continuous cardiac monitoring]:::action B --> C[12-lead ECG<br/>Troponin, BNP, Lactate]:::action C --> D{Shock present?}:::decision D -->|Yes| E[Start inotropic support<br/>Dopamine or Dobutamine]:::action D -->|No| F[Supportive care<br/>Monitor closely]:::action E --> G[Fluid resuscitation<br/>Cautious, avoid pulmonary edema]:::action G --> H[Monitor for arrhythmias<br/>Conduction blocks]:::decision H -->|Bradycardia/Block| I[Prepare for pacing<br/>Consider temporary pacemaker]:::urgent H -->|Stable| J[Continue monitoring<br/>Serial troponin]:::action ``` ### Cardiac Monitoring Parameters in Diphtheria **Mnemonic — ECG Changes in Diphtheria Myocarditis: ABCD** - **A**V block (first, second, or third degree) - **B**radycardia (paradoxical, despite shock) - **C**ardiomegaly (on chest X-ray) - **D**iffuse ST-T wave changes (ischemia pattern) ### Why NOT the Other Options? #### Option 1: Second Dose of Antitoxin - A single dose of 50,000 units IV is adequate for this case - Antitoxin is effective only against **circulating toxin**, not toxin already bound to myocardial cells - By day 5, most toxin has already bound to tissues; additional antitoxin will not reverse myocardial damage - Repeat dosing is not indicated unless there is clinical evidence of ongoing toxin production (rare) #### Option 3: Emergency Tracheostomy - This patient's respiratory distress is secondary to **pulmonary edema from myocarditis**, not airway obstruction - The pseudomembrane is confined to the pharynx and does not extend to the larynx or trachea - Tracheostomy is indicated only if there is evidence of **laryngeal involvement** (stridor, hoarseness) or **impending airway obstruction** - Performing tracheostomy in a hemodynamically unstable child increases anesthetic risk #### Option 4: Increased Antibiotic Dose and Vancomycin - Antibiotics eliminate the organism and prevent further toxin production, but do not reverse existing myocardial damage - Standard penicillin G or erythromycin is adequate; vancomycin is not indicated (diphtheria is penicillin-sensitive) - Antibiotic therapy is important but **secondary** to hemodynamic stabilization in a child with shock ### Antibiotic Regimen (Already Initiated) - **Penicillin G:** 50,000 units/kg/day IV in divided doses (preferred) - **OR Erythromycin:** 40–50 mg/kg/day orally in divided doses - **Duration:** 7–10 days ### Prognostic Factors in Diphtheria Myocarditis | Factor | Prognosis | |---|---| | **Hypotension at presentation** | Poor; indicates advanced myocarditis | | **Complete heart block** | Very poor; mortality >50% | | **Elevated troponin** | Indicates myocardial necrosis; worse prognosis | | **Early onset (day 1–5)** | May indicate severe toxemia; variable prognosis | | **Late onset (week 2–3)** | Often follows recovery from acute phase; better prognosis | ### Long-term Sequelae - **Dilated cardiomyopathy** (in survivors with severe myocarditis) - **Chronic conduction abnormalities** - **Heart failure** (may develop weeks to months later) [cite:Park 26e Ch 8; Harrison 21e Ch 139] 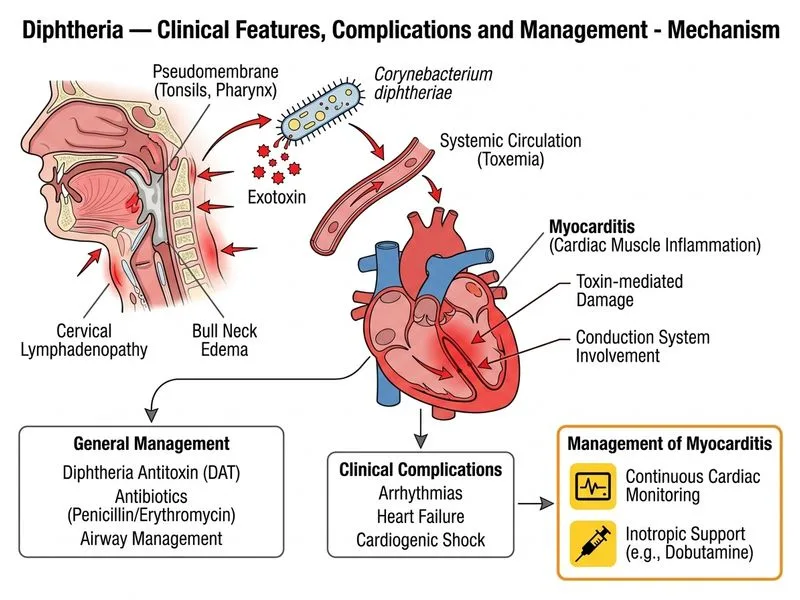
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.