## Clinical Scenario Analysis This child has developed **post-diphtheric neuropathy**, a well-recognized complication occurring in the 2nd–3rd week of illness. The symmetrical lower limb weakness with diminished reflexes is pathognomonic for this complication. ## Pathophysiology of Diphtheric Neuropathy **Key Point:** Diphtheric neuropathy is caused by **diphtheria toxin-mediated demyelination**, not by ongoing bacterial infection or inflammation. It occurs despite appropriate antibiotic and antitoxin therapy because the toxin has already caused irreversible damage to myelin. **Mnemonic:** **DIPHTHERIA NEURO** — Demyelinating, Irreversible, Post-toxin, Happens despite therapy, Toxin-mediated, Hyporeflexia, Electrolyte monitoring, Recovery is slow, Respiratory involvement is the danger, Intensive supportive care. ## Why This Is NOT Meningitis | Feature | Diphtheric Neuropathy | Meningitis | |---------|----------------------|------------|| | **Onset** | Days 5–21 of illness | Acute, within 48 hrs | | **Pattern** | Symmetrical, ascending | Variable, often meningeal signs | | **CSF** | Normal or mildly elevated protein | High protein, pleocytosis | | **Fever** | Absent (child is afebrile) | Present | | **Reflexes** | Diminished/absent | Normal or hyperactive | This child is **afebrile** — meningitis is unlikely. Lumbar puncture is not indicated and may delay supportive care. ## Management of Diphtheric Neuropathy ```mermaid flowchart TD A[Diphtheric neuropathy diagnosed]:::outcome --> B[Continue antibiotics & antitoxin]:::action B --> C[Assess respiratory muscles]:::decision C -->|Intact| D[Monitor for progression]:::action C -->|Weak| E[Prepare for respiratory support]:::action D --> F[Supportive care: nutrition, PT/OT]:::action E --> F F --> G[Recovery over weeks to months]:::outcome ``` **High-Yield:** Management is **supportive**, not curative. Antitoxin and antibiotics have already been given; they cannot reverse toxin-induced demyelination. ## Monitoring Priorities 1. **Respiratory function**: Bulbar and respiratory muscle involvement is the life-threatening complication. Monitor vital capacity, ability to swallow, and cough reflex. 2. **Nutritional support**: Nasogastric feeding if bulbar weakness develops. 3. **Physical therapy**: Passive range of motion and positioning to prevent contractures. 4. **Electrolyte monitoring**: Ensure adequate sodium, potassium, and magnesium for neuromuscular function. **Clinical Pearl:** Most children recover completely over 2–3 months, but respiratory involvement can be fatal. The focus is on preventing complications, not treating the neuropathy itself. [cite:Park 26e Ch 8; Harrison 21e Ch 139] 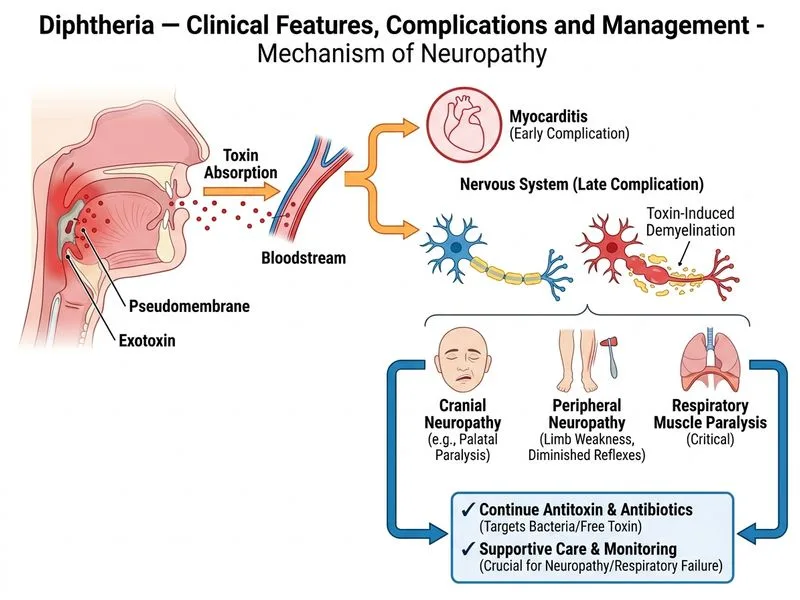
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.