## Cardiac vs. Neurological Complications of Diphtheria ### Temporal and Clinical Distinction | Complication | Onset | Mechanism | Clinical Features | Prognosis | |--------------|-------|-----------|------------------|----------| | **Myocarditis** | Days 3–5 | Diphtheria toxin → ADP-ribosylation of EF-2 → impaired protein synthesis in myocardium | Conduction abnormalities, arrhythmias, cardiogenic shock, heart failure | High mortality if untreated | | **Diphtheritic polyneuritis** | Days 7–21 (peak 10–14) | Toxin-mediated demyelination of peripheral nerves | Ascending motor paralysis, sensory loss (stocking-glove), cranial nerve palsies | Generally reversible with supportive care | **Key Point:** Diphtheritic polyneuritis is a **delayed neurological complication** occurring 7–21 days after symptom onset, whereas myocarditis is an **early complication** (days 3–5). The stocking-glove sensory loss and foot drop in Child B are classic for peripheral neuropathy, not cardiac disease. **High-Yield:** The timing of complications is crucial for diagnosis: - **Early (days 3–5):** Myocarditis, arrhythmias, shock - **Late (days 7–21):** Diphtheritic polyneuritis (motor > sensory, ascending pattern) **Mnemonic:** **DIPHTHERIA COMPLICATIONS = "EARLY HEART, LATE NERVES"** - Early: Myocarditis (toxin damages cardiac myocytes) - Late: Polyneuritis (toxin demyelinates peripheral nerves) **Clinical Pearl:** Diphtheritic polyneuritis typically begins with cranial nerve involvement (soft palate paralysis, loss of accommodation) and progresses to ascending motor paralysis. Sensory involvement is less prominent than motor. Recovery is usually complete if the patient survives the acute phase. **Warning:** Do not confuse diphtheritic polyneuritis with Guillain-Barré syndrome (GBS). GBS occurs within days 1–4 post-infection, has rapid ascending paralysis with prominent sensory loss, and elevated CSF protein. Diphtheritic neuropathy is slower in onset and primarily motor. [cite:Park 26e Ch 7; Harrison 21e Ch 139] 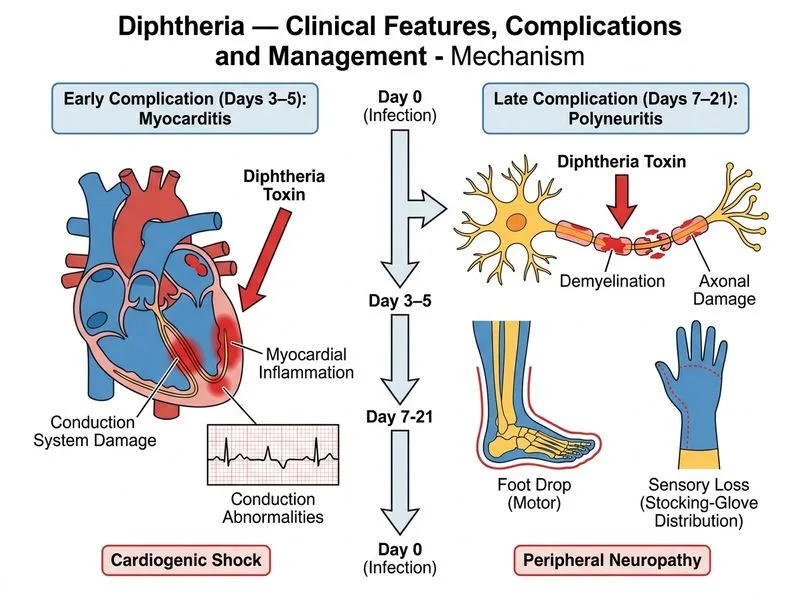
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.