## Diphtheritic Neuropathy: Cranial Nerve Involvement ### Clinical Presentation Analysis The patient presents with: - **Blurred vision + difficulty in accommodation** → ciliary muscle paralysis - **Intact extraocular movements** → rules out oculomotor nerve (CN III) palsy - **Normal pupillary light reflex** → rules out CN III involvement This constellation is pathognomonic for **ciliary nerve paralysis** (parasympathetic fibers of CN V). ### Pathophysiology of Diphtheritic Neuropathy **Key Point:** Diphtheria toxin causes demyelination of motor and parasympathetic nerves via inhibition of protein synthesis (ADP-ribosylation of elongation factor 2). Cranial nerves are affected in a characteristic sequence. ### Temporal Sequence of Cranial Nerve Involvement ```mermaid flowchart TD A[Diphtheria toxin absorption]:::outcome --> B[Days 3-5: Soft palate palsy]:::action B --> C[Days 5-7: Ciliary nerve paralysis]:::action C --> D[Accommodation paralysis + blurred vision]:::outcome D --> E[Days 7-10: Extraocular nerve palsies]:::action E --> F[Days 10-14: Bulbar palsies]:::action F --> G[Aspiration risk]:::urgent A --> H[Myocarditis: Days 4-6]:::urgent H --> I[Conduction block, arrhythmia]:::urgent ``` ### Cranial Nerve Involvement Pattern | Nerve | Timing | Clinical Feature | Mechanism | |-------|--------|------------------|----------| | **Soft palate (CN IX, X)** | Days 3–5 | Nasal regurgitation, nasal twang | Motor paralysis | | **Ciliary nerve (CN V parasympathetic)** | Days 5–7 | Accommodation paralysis, blurred vision | Parasympathetic demyelination | | **Extraocular nerves (CN III, IV, VI)** | Days 7–10 | Ophthalmoplegia, diplopia | Motor demyelination | | **Bulbar nerves (CN IX, X, XII)** | Days 10–14 | Dysphagia, dysphonia, tongue weakness | Motor paralysis | | **Peripheral motor nerves** | Weeks 2–3 | Ascending paralysis (Guillain-Barré–like) | Demyelination | **High-Yield:** The **ciliary nerve paralysis is the earliest cranial nerve complication** (days 5–7), presenting as accommodation paralysis before extraocular nerve involvement. ### Why This Is Ciliary Nerve Paralysis 1. **Accommodation paralysis** = ciliary muscle dysfunction 2. **Blurred vision** = inability to focus on near objects 3. **Intact extraocular movements** = CN III, IV, VI are still functional 4. **Normal pupillary reflex** = pupillary sphincter (CN III parasympathetic) is spared at this stage **Clinical Pearl:** Accommodation paralysis precedes pupillary involvement because the ciliary muscle is more sensitive to toxin-induced demyelination than the pupillary sphincter. ### Management of Diphtheritic Neuropathy - **Supportive care:** No specific treatment reverses demyelination - **Prognosis:** Most cranial nerve palsies resolve within 2–3 months - **Prevention of complications:** - Aspiration precautions if bulbar involvement develops - Cardiac monitoring for myocarditis - Respiratory support if respiratory muscle paralysis occurs ### Why Not the Other Options? **Myocarditis** would present with: - Chest pain, dyspnea, palpitations - Cardiogenic shock (hypotension, poor perfusion) - ECG changes (ST depression, T-wave inversion, prolonged PR interval) - Occurs days 4–6, but this patient has ocular symptoms on day 5 **Oculomotor nerve (CN III) palsy** would present with: - Ptosis, mydriasis, "down and out" eye position - Impaired extraocular movements (this patient's are intact) - Occurs later (days 7–10) **Bulbar palsy** would present with: - Dysphagia, dysphonia, nasal regurgitation - Occurs days 10–14 (later than this patient's presentation) [cite:Park 26e Ch 8; Harrison 21e Ch 139] 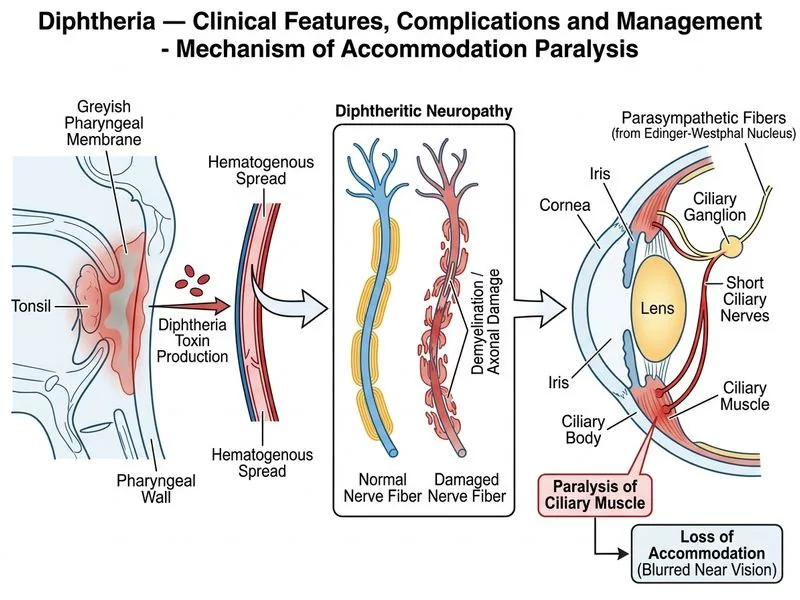
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.