## Hypothyroidism in Down Syndrome **Key Point:** Children with Down syndrome have a 10–15% prevalence of hypothyroidism, predominantly autoimmune (Hashimoto thyroiditis). When TSH and free T4 are both abnormal with clinical symptoms, treatment should be initiated without delay. ## Pathophysiology of Thyroid Disease in Down Syndrome ### Mechanism - Increased susceptibility to autoimmune thyroid disease (Hashimoto thyroiditis) - Possible link to chromosome 21 genes involved in immune regulation - Higher prevalence of anti-thyroid peroxidase (anti-TPO) and anti-thyroglobulin antibodies ### Types of Thyroid Dysfunction | Type | Frequency | TSH | Free T4 | Clinical Presentation | |------|-----------|-----|---------|----------------------| | **Primary hypothyroidism** | 60–70% of cases | ↑↑ | ↓ | Fatigue, poor feeding, constipation, weight gain, developmental regression | | **Subclinical hypothyroidism** | 20–30% of cases | ↑ | Normal | Often asymptomatic; requires monitoring | | **Hyperthyroidism** | <5% of cases | ↓ | ↑ | Tachycardia, irritability, poor weight gain | **High-Yield:** Screening recommendations for Down syndrome: - **Baseline:** TSH and free T4 at diagnosis (or within first 6 months of life) - **Frequency:** Every 6–12 months in childhood; annually in adolescence and adulthood ## Clinical Features of Hypothyroidism in This Case The patient presents with: - **Irritability** — can be mistaken for behavioral issues - **Poor feeding** — reduced appetite and swallowing difficulty - **Constipation** — slowed GI motility - **Goiter** — firm, enlarged thyroid gland These symptoms, combined with elevated TSH (8.2) and low free T4 (2.1), confirm **overt primary hypothyroidism** requiring immediate treatment. ## Management of Hypothyroidism ### Indications for Treatment 1. **Overt hypothyroidism** (TSH ↑ + free T4 ↓) — **treat immediately** 2. **Subclinical hypothyroidism** (TSH ↑ + free T4 normal): - Treat if TSH >10 mIU/L - Recheck in 6 weeks if TSH 5–10 mIU/L (may be transient) - Monitor every 6 months if TSH 5–10 and asymptomatic ### Levothyroxine Dosing **Starting dose:** - Children: 1.5–2.0 mcg/kg/day (typical: 25–50 mcg/day for toddlers) - Adjust based on TSH response **Monitoring:** - Recheck TSH and free T4 at 4–6 weeks after initiation - Target TSH: 0.5–2.5 mIU/L in children with Down syndrome (slightly lower than general population) - Adjust dose by 12.5–25 mcg increments - Once stable, recheck annually **Clinical Pearl:** Levothyroxine should be given on an empty stomach, 30–60 minutes before food or other medications (especially calcium, iron, multivitamins), as these reduce absorption. ## Why Immediate Treatment Is Warranted ```mermaid flowchart TD A["Down syndrome child with symptoms<br/>(irritability, poor feeding, constipation)"]:::outcome A --> B["TSH elevated + free T4 low"]:::outcome B --> C{"Overt hypothyroidism?"}:::decision C -->|Yes| D["Start levothyroxine immediately"]:::action C -->|No| E["Subclinical: check TSH level"]:::decision E -->|TSH > 10| F["Treat"]:::action E -->|TSH 5-10| G["Recheck in 6 weeks"]:::action D --> H["Recheck TSH/free T4 at 4-6 weeks"]:::action H --> I["Adjust dose to target TSH 0.5-2.5"]:::action I --> J["Annual monitoring"]:::action ``` **Mnemonic: "THAW" = Thyroid screening, Hypothyroidism common in Down, Autoimmune etiology, Warrant early treatment** ## Why Other Options Are Incorrect - **Repeating labs in 6 weeks:** Inappropriate when overt hypothyroidism with symptoms is already confirmed. Delaying treatment risks developmental regression and worsening symptoms. - **Thyroid ultrasound and antibodies:** Useful for diagnosis confirmation but should not delay treatment initiation. Antibodies confirm autoimmune etiology but don't change management. - **Reassurance:** Thyroid dysfunction in Down syndrome is NOT self-limiting and requires lifelong management. 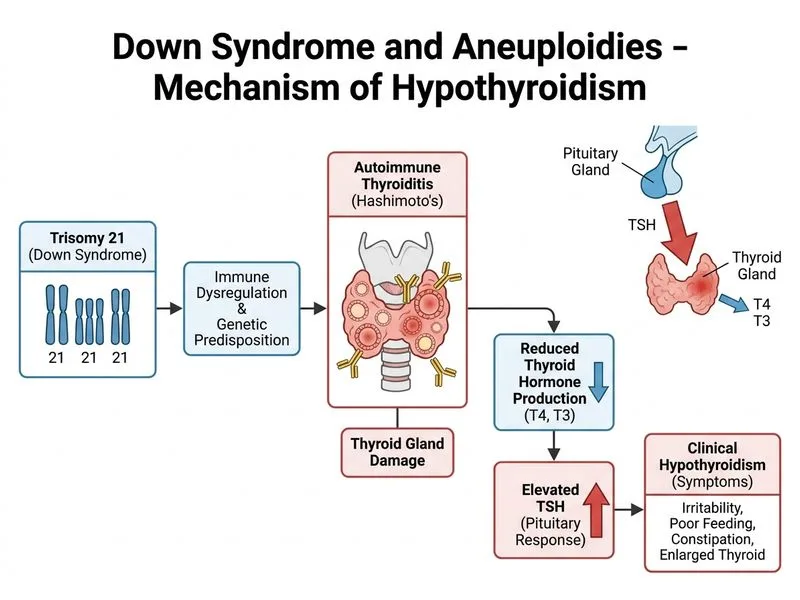
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.