## Atrial Fibrillation: ECG Recognition and Clinical Correlation ### Key ECG Findings in This Case **Key Point:** The combination of an **irregularly irregular heart rhythm**, **absence of P waves**, and **fine baseline undulation** (fibrillatory waves or "f waves") is diagnostic of atrial fibrillation (AF). ### Differential Diagnosis of Rapid Arrhythmias | Feature | Atrial Fibrillation | Atrial Flutter | Ventricular Tachycardia | SVT | |---------|---|---|---|---| | **Rhythm** | Irregularly irregular | Regular (or regular with variable block) | Regular | Regular | | **P waves** | Absent; replaced by f waves | Sawtooth pattern (flutter waves) | Absent or buried | Buried in QRS/T | | **Baseline** | Fine or coarse fibrillatory waves | Sawtooth baseline | Smooth | Smooth | | **QRS duration** | Narrow (< 120 ms) unless aberrancy | Narrow | Wide (≥ 120 ms) | Narrow | | **Ventricular rate** | 100–180 bpm (uncontrolled) | 150–350 bpm | 120–250 bpm | 140–250 bpm | | **Heart sounds** | Irregularly irregular | Regular or regular with pauses | Regular | Regular | **Clinical Pearl:** The **irregularly irregular rhythm** is the hallmark of AF. When you hear the heart sounds are "irregularly irregular," AF should be your first thought. This distinguishes AF from atrial flutter, which typically presents with a regular ventricular response (unless variable AV block is present). ### Pathophysiology of Atrial Fibrillation 1. **Loss of organized atrial contraction** → multiple ectopic foci fire chaotically in the atria 2. **Fibrillatory waves** replace normal P waves (fine waves at ~350–600 bpm) 3. **Variable AV nodal conduction** → irregular ventricular rate (typically 100–180 bpm if uncontrolled) 4. **Loss of atrial kick** → reduced cardiac output and increased stroke volume variability ### Clinical Features in This Patient - **Palpitations and dizziness** → due to rapid, irregular ventricular rate and loss of atrial contribution to ventricular filling - **Irregularly irregular pulse** → pathognomonic for AF - **Normal troponin** → rules out acute MI; AF can be primary (lone AF) or secondary to other cardiac/systemic conditions - **No chest pain** → suggests AF is not secondary to acute coronary syndrome **High-Yield:** AF is the most common sustained arrhythmia in clinical practice. Risk factors include: - Age > 65 years - Hypertension - Heart failure - Valvular disease - Hyperthyroidism - Chronic lung disease - Diabetes ### Management Approach ```mermaid flowchart TD A[Atrial Fibrillation with RVR]:::outcome --> B{Hemodynamically stable?}:::decision B -->|No - hypotensive/shock| C[Synchronized DC cardioversion]:::urgent B -->|Yes| D{Duration < 48 hrs?}:::decision D -->|Yes| E[Can anticoagulate safely?]:::decision D -->|No| F[Anticoagulate for 3 weeks before cardioversion]:::action E -->|Yes| G[Cardioversion or rate control]:::action E -->|No| H[TEE-guided cardioversion]:::action G --> I[Rate control: Beta-blocker, CCB, or digoxin]:::action I --> J[Anticoagulation: DOAC or warfarin]:::action ``` **Mnemonic: AF = CHADS~2~VASc Score for Stroke Risk** - **C**ongestive heart failure - **H**ypertension - **A**ge ≥ 75 years (2 points) - **D**iabetes - **S**troke/TIA/thromboembolism (2 points) - **V**ascular disease - **A**ge 65–74 years - **S**ex category (female) - **c**linical category Score ≥ 2 in men or ≥ 3 in women → anticoagulation indicated. 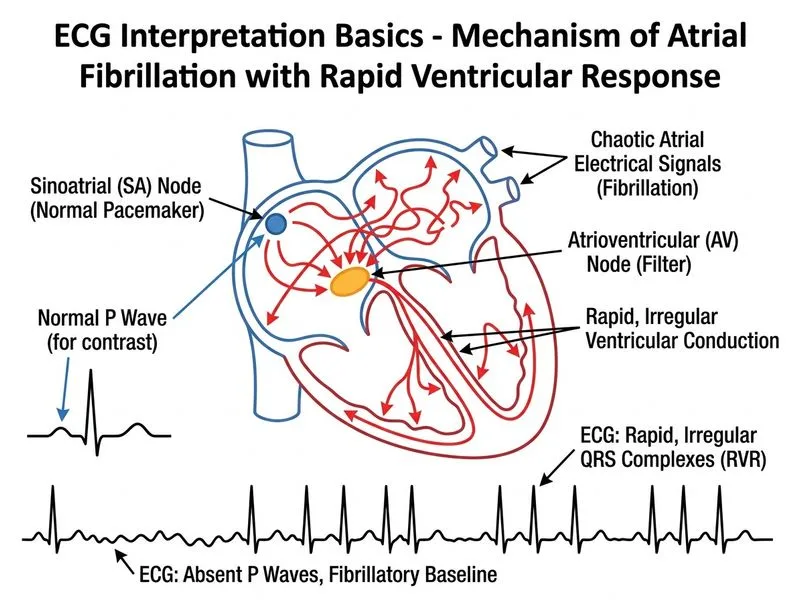
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.