## Investigation of Choice in Acute STEMI **Key Point:** In a patient with clinical symptoms and ECG evidence of STEMI (ST elevation in anatomically contiguous leads with reciprocal changes), coronary angiography is the definitive investigation and therapeutic intervention of choice. ### Why Coronary Angiography? 1. **Diagnostic confirmation**: Directly visualizes the culprit coronary artery and the site of thrombotic occlusion 2. **Therapeutic intervention**: Allows immediate percutaneous coronary intervention (PCI) — primary PCI is the gold standard for STEMI management when performed within 120 minutes of first medical contact 3. **Risk stratification**: Identifies collateral circulation, extent of disease, and left ventricular function 4. **Time-sensitive**: Delays in coronary angiography increase mortality; guideline-recommended door-to-balloon time is <90 minutes ### Role of Other Investigations | Investigation | Role | Timing | |---|---|---| | **Cardiac biomarkers (troponin, CK-MB)** | Confirms myocardial necrosis; NOT diagnostic of acute MI alone; rises 3–4 hours post-infarction | Supportive, not first-line | | **Echocardiography** | Assesses wall motion abnormalities, ejection fraction, mechanical complications | After acute phase; not for diagnosis | | **Chest X-ray** | Rules out pulmonary causes; identifies cardiomegaly or pulmonary edema | Supportive; not diagnostic | **High-Yield:** STEMI + clinical symptoms = **proceed directly to coronary angiography/PCI**. Do NOT wait for biomarker results. **Clinical Pearl:** In this patient, the inferior wall STEMI (II, III, aVF) with reciprocal changes indicates right coronary artery (RCA) occlusion in ~80% of cases. Right ventricular involvement should be suspected, and aggressive fluid resuscitation should be avoided if RV infarction is present — coronary angiography will clarify this. [cite:Harrison 21e Ch 297] 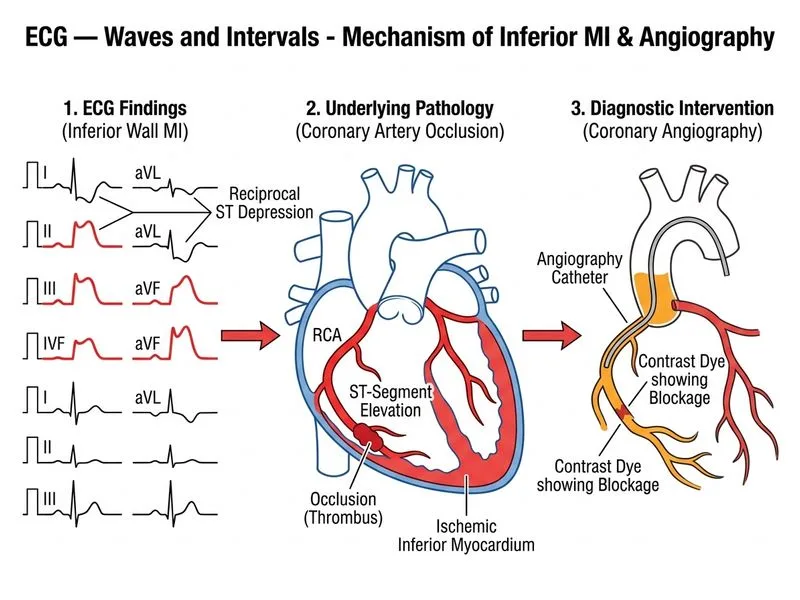
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.