## Clinical Context The patient presents with an incidental finding of prolonged QTc interval (normal: < 450 ms in women). The differential diagnosis of prolonged QT includes: 1. **Acquired causes** (drug-induced, electrolyte abnormalities) 2. **Congenital Long QT Syndrome (LQTS)** (genetic channelopathies) The asymptomatic status and absence of family history do not exclude either category, but the investigation strategy must first exclude reversible, life-threatening acquired causes before pursuing genetic testing. ## Why Electrolyte Panel Is Correct **Key Point:** Electrolyte abnormalities — particularly **hypocalcemia, hypomagnesemia, and hypokalemia** — are common, reversible causes of QT prolongation that carry significant arrhythmia risk (Torsades de Pointes). These must be ruled out first because: - They are immediately correctable - They are more common than congenital LQTS in the general population - Correction may normalize the QTc without further intervention - They are life-threatening if missed **High-Yield:** Serum electrolytes (K^+^, Ca^2+^, Mg^2+^) are the **first-line investigation** for any patient with prolonged QT interval, regardless of clinical presentation. **Mnemonic: ABCDE of QT Prolongation —** - **A**ntiarrhythmics (Class IA, III) - **B**eta-blockers (some) - **C**alcium channel blockers - **D**rugs (macrolides, fluoroquinolones, antipsychotics) - **E**lectrolyte abnormalities (↓K^+^, ↓Mg^2+^, ↓Ca^2+^) ## Investigation Algorithm for Prolonged QT ```mermaid flowchart TD A[Prolonged QTc on ECG]:::outcome --> B[Repeat ECG to confirm]:::action B --> C{QTc still prolonged?}:::decision C -->|No| D[Measurement error / benign variant]:::outcome C -->|Yes| E[Electrolyte panel]:::action E --> F{Electrolytes abnormal?}:::decision F -->|Yes: ↓K⁺, ↓Mg²⁺, ↓Ca²⁺| G[Correct deficiency]:::action G --> H[Repeat ECG after correction]:::action F -->|No: Normal electrolytes| I[Review medications]:::action I --> J{Offending drug identified?}:::decision J -->|Yes| K[Discontinue / substitute]:::action J -->|No| L[Consider genetic testing for LQTS]:::action K --> M[Repeat ECG]:::action L --> N[Genetic counseling + testing]:::action ``` ## Comparison: When to Pursue Each Investigation | Investigation | Indication | Timing | | --- | --- | --- | | **Electrolyte panel** | All patients with prolonged QT | **First** — immediate | | **Medication review** | All patients with prolonged QT | **First** — concurrent | | **Genetic testing** | Persistent QT prolongation after electrolyte/drug correction; family history of sudden death; recurrent syncope | **Third** — after acquired causes excluded | | **Exercise stress test** | Suspected LQTS (especially Romano-Ward type); syncope with exercise | **Selective** — if LQTS suspected | | **Coronary angiography** | Chest pain or ischemic ECG changes | **Not indicated** for QT prolongation alone | ## Clinical Pearl In this asymptomatic woman with incidental QT prolongation, the absence of syncope or family history does not exclude congenital LQTS, but it does lower pretest probability. Electrolyte correction is the critical first step: if QTc normalizes after electrolyte repletion, no further workup may be needed. If QTc remains prolonged despite normal electrolytes and no offending drugs, genetic testing becomes appropriate. 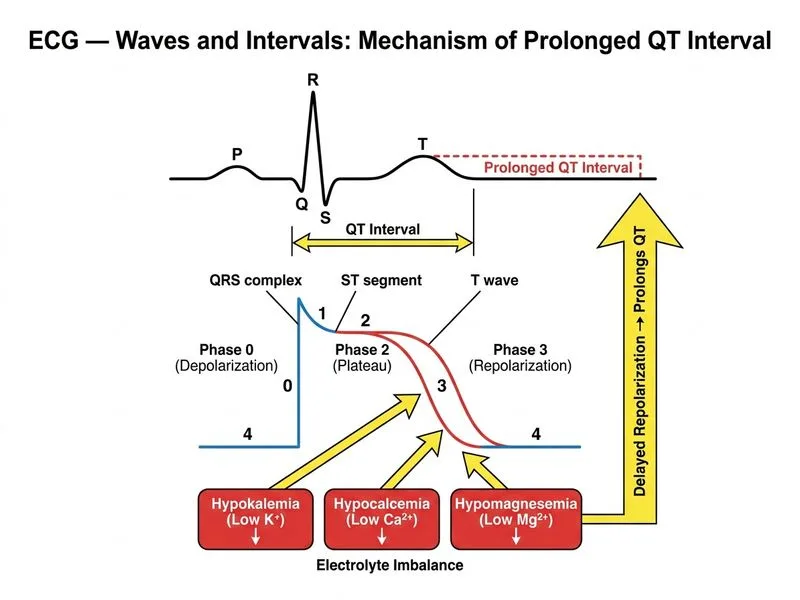
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.