## ECG Diagnosis: Wolff-Parkinson-White (WPW) Syndrome with Atrioventricular Reentrant Tachycardia (AVNRT) **Key Point:** The **short PR interval (<0.12 s)** and **delta wave** (slurred QRS upstroke) are pathognomonic for **pre-excitation** via an **accessory pathway (AP)**. In the setting of a regular narrow-complex tachycardia, this is **AVNRT in WPW syndrome**. **High-Yield:** WPW-associated AVNRT is the most common tachyarrhythmia in patients with pre-excitation. The reentry circuit uses the AV node (orthodromic) and the AP (antidromic) in a reciprocal loop. ## Acute Management of Hemodynamically Stable AVNRT in WPW ### First-Line Agent: Adenosine **Mechanism:** Adenosine blocks AV nodal conduction, breaking the reentry circuit by interrupting the orthodromic limb of the circuit. **Dosing:** - Initial: **6 mg IV rapid push** followed by 10–20 mL saline flush - If no response in 1–2 minutes: **12 mg IV rapid push** - Success rate: >90% for AVNRT termination **Clinical Pearl:** Adenosine works **rapidly** (within seconds) and is **safe** even in the elderly because its half-life is <10 seconds. Transient asystole or brief hypotension is expected and self-limited. **Warning:** ~~Verapamil~~ is **contraindicated in pre-excited atrial fibrillation** (AF with WPW) because it blocks the AV node preferentially, forcing conduction down the AP, which may have a shorter refractory period and cause rapid ventricular rates or degeneration to VF. However, in **orthodromic AVNRT** (narrow-complex), verapamil is theoretically safe but is **second-line** because adenosine is faster and more reliable. ```mermaid flowchart TD A["Regular narrow-complex tachycardia<br/>+ short PR + delta wave"]:::outcome --> B{"Hemodynamically stable?"}:::decision B -->|Yes| C["Adenosine 6 mg IV push"]:::action C --> D{"Tachycardia terminated?"}:::decision D -->|Yes| E["Diagnosis: AVNRT in WPW<br/>Arrange EP study for ablation"]:::outcome D -->|No| F["Adenosine 12 mg IV push"]:::action F --> G{"Terminated?"}:::decision G -->|Yes| E G -->|No| H["Consider verapamil or diltiazem"]:::action B -->|No| I["Synchronized DC cardioversion"]:::urgent ``` ## Why Other Options Are Suboptimal | Option | Reason | |--------|--------| | **DC Cardioversion** | Reserved for hemodynamic instability or adenosine failure. This patient is stable and adenosine is first-line. | | **Verapamil** | Second-line agent; slower onset than adenosine. Also carries risk in pre-excited AF (though not relevant here). | | **EP Study** | Diagnostic and therapeutic (ablation) but NOT an acute management step. EP study is arranged **after** acute termination and stabilization. | **High-Yield:** The **short PR interval persists** even when the tachycardia is terminated (it is a baseline feature of WPW). Do not mistake resolution of tachycardia for resolution of pre-excitation; the AP remains and requires definitive ablation. ## Definitive Management After acute termination: 1. **Electrophysiology study** to localize the AP 2. **Radiofrequency catheter ablation** of the AP (curative; >95% success) 3. Avoid long-term rate-limiting drugs (beta-blockers, verapamil) in pre-excited AF because they increase AP conduction risk 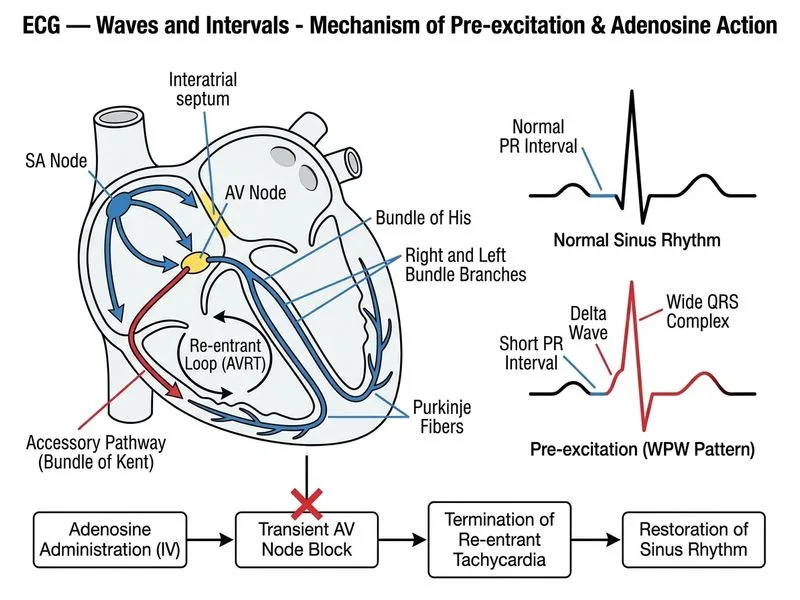
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.