## Clinical Diagnosis **Key Point:** Drug-induced epistaxis (warfarin over-anticoagulation) with diffuse oozing from both nasal cavities and **supratherapeutic INR (4.2 vs. target 2–3)** requires **reversal of anticoagulation** as the primary intervention, NOT local hemostasis alone. ## Pathophysiology Warfarin inhibits vitamin K-dependent factors (II, VII, IX, X). An INR >4 significantly increases bleeding risk, particularly in mucous membranes (nose, GI tract). Diffuse bilateral oozing indicates systemic coagulopathy, not a localized vessel rupture. ## Management Algorithm ```mermaid flowchart TD A[Epistaxis on Warfarin]:::outcome --> B{INR level?}:::decision B -->|INR 2-3 therapeutic| C[Topical hemostasis + cauterization]:::action B -->|INR 3-4| D[Reduce warfarin dose]:::action B -->|INR > 4| E[Reverse anticoagulation]:::urgent E --> F[Vitamin K 5-10 mg IV/PO]:::action E --> G[Fresh Frozen Plasma or PCC]:::action F --> H[Topical hemostatic agents]:::action G --> H H --> I[Monitor INR, recheck in 24 hrs]:::action I --> J{Bleeding controlled?}:::decision J -->|Yes| K[Resume warfarin at lower dose]:::action J -->|No| L[Cauterization or packing]:::action ``` ## Anticoagulation Reversal Strategy **High-Yield:** For **INR >4 with bleeding**: 1. **Vitamin K (phytonadione):** 5–10 mg IV or PO - Onset: 12–24 hours (slow) - Must be combined with faster agents for immediate reversal 2. **Fresh Frozen Plasma (FFP):** 10–15 mL/kg (contains factors II, VII, IX, X) - Onset: immediate - Preferred over FFP: **Prothrombin Complex Concentrate (PCC)** 25–50 units/kg (more concentrated, less volume) 3. **Recheck INR in 24 hours** after reversal ## Role of Topical Hemostasis **Clinical Pearl:** In drug-induced epistaxis, topical hemostatic agents (thrombin, gelfoam, tranexamic acid-soaked gauze) are **adjunctive** and work best when the underlying coagulopathy is corrected. Packing or cauterization without anticoagulation reversal will fail. ## Why Not Cauterization Alone? Cauterization addresses a localized bleeding vessel. In diffuse bilateral oozing from supratherapeutic anticoagulation, there is no single "bleeding point" — the entire nasal mucosa is at risk. Reversal of INR is the definitive treatment. ## Monitoring and Follow-up - Recheck INR 24 hours after reversal - Resume warfarin at a **lower maintenance dose** once INR is therapeutic - Investigate cause of over-anticoagulation (drug interaction, dietary change, compliance issue) - Consider alternative anticoagulation (DOAC) if recurrent epistaxis on warfarin 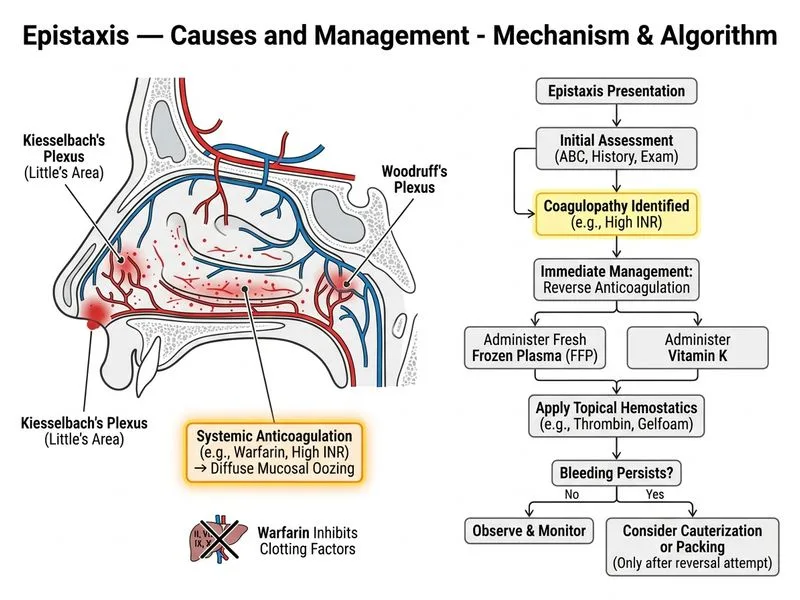
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.