## Management of Failed Anterior Packing (Posterior Epistaxis) **Key Point:** Blood dripping into the nasopharynx and oropharynx indicates posterior epistaxis (from sphenopalatine or posterior ethmoidal arteries). Failed anterior packing signals the bleeding source is posterior, requiring posterior packing or endoscopic intervention. **High-Yield:** Posterior epistaxis accounts for 15–20% of cases and is more common in elderly patients with hypertension or coagulopathy. It requires: 1. Removal of failed anterior pack 2. Posterior nasal packing (Foley catheter, ribbon gauze, or specialized posterior pack) 3. Concurrent anterior packing (to prevent anterior leakage) 4. Admission and monitoring (risk of airway obstruction, aspiration, sinusitis) **Clinical Pearl:** The presence of blood in the nasopharynx/oropharynx after anterior packing failure is pathognomonic for posterior bleed. This patient is stable (no shock), so posterior packing is appropriate before considering embolization. ### Posterior Packing Technique - **Foley catheter method:** 14–16 Fr catheter inserted through nose, inflated in nasopharynx, secured with gauze rolls - **Ribbon gauze method:** Layered gauze packing from posterior to anterior - **Duration:** 48–72 hours (risk of sinusitis and ischemia increases beyond 5 days) - **Adjuncts:** Broad-spectrum antibiotics, topical vasoconstrictor, oxygen if needed **Mnemonic: POST-P** — Posterior bleed (nasopharyngeal blood), Observe (confirm posterior source), Stop anterior pack (remove failed pack), Treat (posterior pack), Prevent (antibiotics, monitoring). 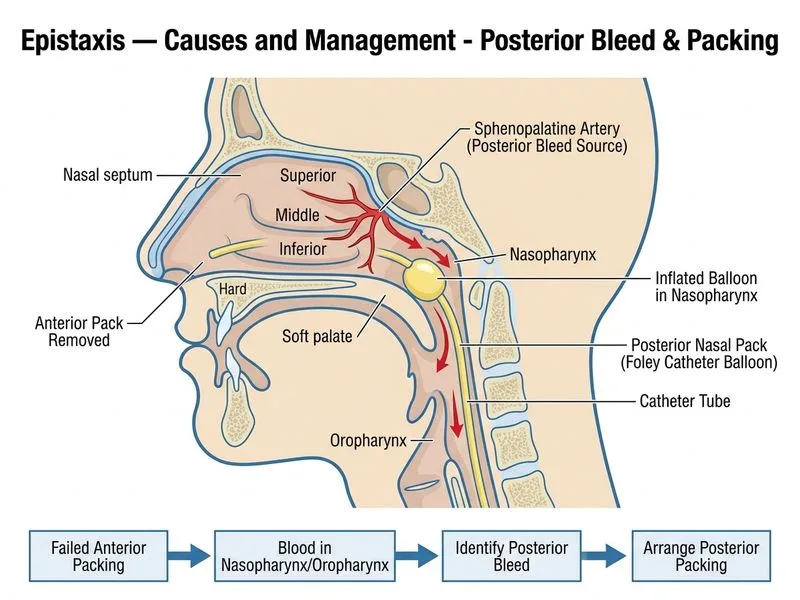
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.