## Distinguishing HHT from ITP in Epistaxis ### Key Pathophysiologic Difference **Key Point:** HHT (Osler-Weber-Rendu syndrome) is a vascular dysplasia disorder characterized by abnormal arteriovenous communications and mucocutaneous telangiectasia, whereas ITP is a primary platelet disorder with normal vessel structure but quantitative platelet deficiency. ### Comparison Table | Feature | HHT | ITP | |---------|-----|-----| | **Primary pathology** | Vascular dysplasia (AVM, telangiectasia) | Platelet destruction (autoimmune) | | **Mucocutaneous findings** | Telangiectasia on lips, tongue, fingers, GI tract | Petechiae, purpura (no telangiectasia) | | **Platelet count** | Normal (50,000–400,000/μL) | Severely reduced (<20,000/μL typical) | | **Bleeding pattern** | Recurrent, chronic, often severe | Acute onset, mucosal bleeding | | **Inheritance** | Autosomal dominant (80% penetrance) | Acquired (not hereditary) | | **Response to steroids** | Poor | Excellent (70–80% remission) | | **Endoscopy findings** | Visible AVMs in GI tract | Normal mucosa | ### Clinical Pearl **Clinical Pearl:** The presence of **visible telangiectasia on the lips, oral mucosa, and fingertips** is pathognomonic for HHT and is part of the Curaçao diagnostic criteria. ITP patients have a normal-appearing mucosa with only petechial hemorrhages; they do not develop telangiectasia. ### High-Yield Diagnostic Approach **High-Yield:** In a patient with epistaxis and telangiectasia: 1. Check platelet count → normal in HHT, low in ITP 2. Look for mucocutaneous telangiectasia → HHT-specific 3. Screen for GI bleeding and pulmonary AVMs → HHT complications 4. Family history → HHT is autosomal dominant; ITP is acquired ### Why the Correct Answer Stands Option 0 directly identifies the **structural vascular abnormality** (AVM and telangiectasia) that is the hallmark of HHT and is absent in ITP. This is the single best discriminating feature. [cite:Harrison 21e Ch 178] 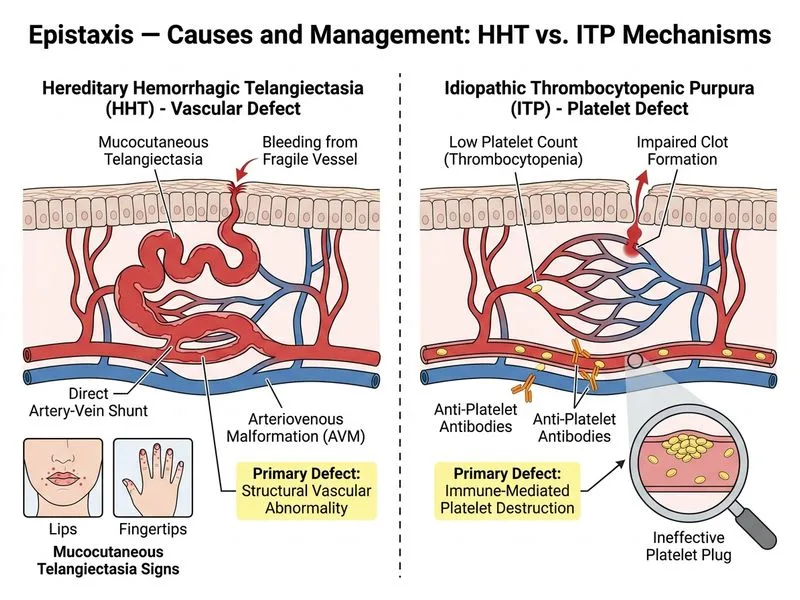
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.