## Management of Anticoagulant-Related Epistaxis This patient has **recurrent epistaxis in the setting of therapeutic anticoagulation** — a common and manageable scenario that requires careful balancing of bleeding risk against thromboembolism risk. ### Clinical Context **High-Yield:** - INR 3.2 is **within target range** (2–3) for mechanical mitral valve; no over-anticoagulation. - **Bilateral epistaxis** suggests mucosal fragility from anticoagulation, not a structural lesion or local trauma. - Stable vital signs and no active bleeding on examination indicate **non-emergent, chronic epistaxis**. - Goal: Maintain anticoagulation for cardiac protection while preventing recurrent bleeds. ### Pathophysiology Anticoagulation (warfarin, DOACs, antiplatelet agents) impairs hemostasis and increases bleeding from minor mucosal trauma or drying. The nasal mucosa is particularly vulnerable due to: - Rich vascularization - Exposure to dry air and crusting - Frequent minor trauma from nose-blowing or rubbing ### Management Hierarchy for Anticoagulant-Related Epistaxis ```mermaid flowchart TD A[Anticoagulant-related epistaxis]:::outcome A --> B{Hemodynamically<br/>stable?}:::decision B -->|No| C[Reverse anticoagulation<br/>+ aggressive hemostasis]:::urgent B -->|Yes| D{Active bleeding<br/>on exam?}:::decision D -->|Yes| E[Topical hemostatics<br/>+ consider packing]:::action D -->|No| F[Optimize INR<br/>+ topical agents<br/>+ nasal hygiene]:::action E --> G[Monitor, maintain<br/>anticoagulation]:::action F --> G G --> H[Recurrent?]:::decision H -->|Yes| I[Endoscopy ±<br/>cautery/ligation]:::action H -->|No| J[Continue prophylaxis]:::action ``` ### Why Option 2 (Optimize INR + Topical Hemostatics + Nasal Hygiene) Is Correct **Key Point:** - This is a **stable, non-emergent epistaxis** in a patient with therapeutic anticoagulation. The goal is to **maintain cardiac protection** while reducing bleeding recurrence. **Rationale:** 1. **INR Optimization**: Reducing INR to 2–2.5 (lower end of therapeutic range) decreases bleeding risk without compromising thromboembolism protection for mechanical mitral valve. This is guideline-recommended for patients with recurrent bleeding on anticoagulation. 2. **Topical Hemostatic Agents**: - **Thrombin (topical)**: Directly activates fibrinogen to fibrin; effective for mucosal bleeding. - **Tranexamic acid (topical or systemic)**: Inhibits fibrinolysis; reduces epistaxis recurrence by ~50% in anticoagulated patients. - **Topical epinephrine or oxymetazoline**: Causes vasoconstriction; reduces bleeding without systemic absorption. 3. **Nasal Hygiene Counseling**: - Avoid nose-blowing, picking, or rubbing. - Use saline nasal irrigation to prevent crusting. - Apply petroleum jelly or antibiotic ointment to nasal vestibule to reduce drying. - Humidify bedroom air. **Clinical Pearl:** - Prophylactic topical hemostatics (thrombin, tranexamic acid) applied 2–3 times weekly can prevent recurrent epistaxis in anticoagulated patients without requiring anticoagulation reversal. ### Why Other Options Are Incorrect **Option 0: Immediate Reversal + Packing** - **Over-treatment** for a stable, non-emergent bleed. - Reversal of warfarin (FFP + vitamin K) carries significant **thromboembolism risk** in a patient with mechanical mitral valve; reversal should be reserved for life-threatening hemorrhage or INR >4. - Packing is not indicated without active bleeding on examination. - Risks sinusitis, aspiration, and patient morbidity. **Option 1: Reduce Warfarin + Decongestant + Follow-up** - **Inadequate management**: Reducing warfarin without topical hemostatics leaves the patient at risk for recurrent bleeding. - Topical decongestants (oxymetazoline) are short-acting and do not address underlying mucosal fragility. - Passive follow-up without active intervention is suboptimal. **Option 3: Discontinue Warfarin + Switch to Aspirin** - **Dangerous**: Discontinuing warfarin in a patient with mechanical mitral valve risks **acute thrombosis** and stroke (annual thromboembolism risk ~4–6% without anticoagulation). - Aspirin 75 mg is **inadequate anticoagulation** for mechanical valve and does not replace warfarin. - Requires urgent cardiology consultation and bridging anticoagulation (LMWH or UFH) if warfarin must be held. ### Summary Table: Epistaxis Management by Anticoagulation Status | Scenario | INR Status | Management | |----------|-----------|-------------| | **Stable, no active bleed** | Therapeutic | Optimize INR (lower end), topical hemostatics, nasal hygiene | | **Active bleeding, stable** | Therapeutic | Topical hemostatics, consider packing; maintain anticoagulation | | **Active bleeding, unstable** | Therapeutic | Reverse anticoagulation (FFP + vitamin K), aggressive hemostasis, ICU monitoring | | **Recurrent despite optimization** | Therapeutic | Endoscopy ± cautery/vessel ligation; maintain anticoagulation | | **Over-anticoagulation (INR >4)** | Supra-therapeutic | Reduce warfarin; vitamin K if INR >4; manage bleed as above | 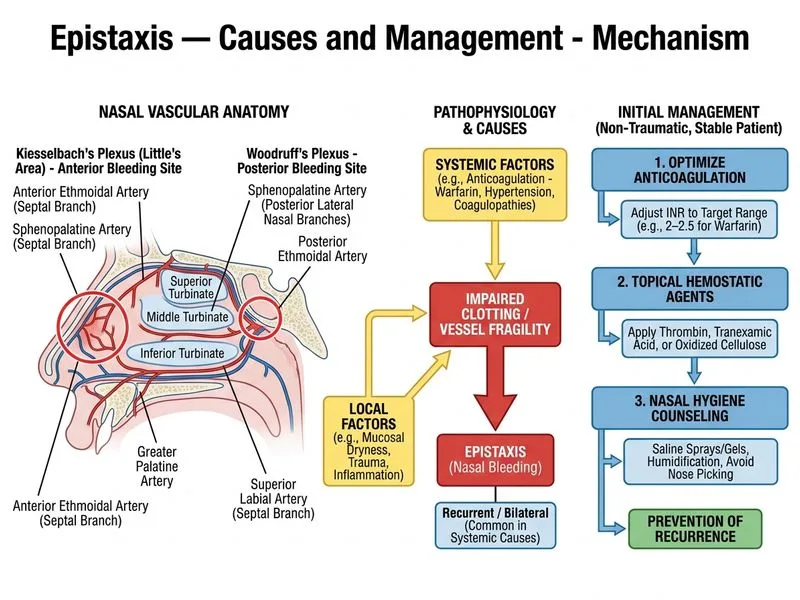
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.