## Epistaxis in Chronic Kidney Disease: Uremic Coagulopathy **Key Point:** Diffuse mucosal oozing (not a discrete bleeding point) in a patient with advanced CKD, anemia, and prolonged INR indicates uremic coagulopathy — a multifactorial bleeding disorder in renal failure. ### Pathophysiology of Uremic Bleeding **High-Yield:** Uremia causes a complex coagulation defect: | Mechanism | Effect | Laboratory Finding | |-----------|--------|--------------------| | **Platelet dysfunction** | Impaired adhesion, aggregation, secretion | Normal/low platelets but prolonged bleeding time | | **Uremic toxins** | Inhibit platelet function | Elevated urea, creatinine | | **Anemia** | Reduced RBC-mediated platelet margination | Low hemoglobin (9.2 g/dL here) | | **Defective Factor VIII/vWF** | Reduced procoagulant activity | Prolonged aPTT, normal PT/INR (or mildly ↑) | | **Fibrinolytic imbalance** | Excess plasmin activity | Elevated D-dimer | ### Clinical Features in This Case **Clinical Pearl:** The patient presents with: 1. **Diffuse mucosal oozing** (not focal bleeding) — hallmark of coagulopathy, not structural lesion 2. **Bilateral epistaxis** — suggests systemic bleeding tendency, not unilateral vascular anomaly 3. **eGFR 28 mL/min/1.73m²** — Stage 4 CKD; uremic toxins accumulate 4. **Hemoglobin 9.2 g/dL** — anemia exacerbates bleeding by reducing platelet margination 5. **Platelet count 85,000/μL** — mild thrombocytopenia (uremia + CKD-related) 6. **INR 1.8** — mildly prolonged (uremic factor deficiency) 7. **No discrete bleeding point** — excludes local structural cause ### Management Algorithm ```mermaid flowchart TD A[Epistaxis + CKD Stage 4]:::outcome --> B{Discrete bleeding point?}:::decision B -->|Yes| C[Local cause: cautery, packing]:::action B -->|No| D[Diffuse oozing: systemic coagulopathy]:::outcome D --> E[Uremic coagulopathy likely]:::outcome E --> F[Optimize renal function]:::action F --> G[Dialysis/ultrafiltration]:::action E --> H[Transfuse RBCs if Hb < 7]:::action E --> I[Avoid NSAIDs, anticoagulants]:::action E --> J[Consider desmopressin if severe]:::action ``` ### Why Uremic Coagulopathy Fits Best **Mnemonic:** **UREMIC** = Uremia, Reduced platelet function, Elevated creatinine, Multifactorial bleeding, Intrinsic coagulation defect, Coagulopathy (not thrombocytopenia alone) 1. **Diffuse oozing** (not focal) = coagulopathy pattern 2. **Advanced CKD** (eGFR 28) = uremic toxin accumulation 3. **Mild thrombocytopenia + prolonged INR** = multifactorial defect 4. **Anemia** = worsens bleeding tendency 5. **Bilateral involvement** = systemic process ### Treatment 1. **Optimize renal function:** Dialysis/ultrafiltration to reduce uremic toxins 2. **Correct anemia:** Transfuse RBCs if Hb < 7 g/dL (improves platelet function) 3. **Desmopressin (DDAVP):** 0.3 μg/kg IV/SC if bleeding severe (enhances vWF release) 4. **Estrogens:** May improve platelet function in chronic uremia 5. **Avoid NSAIDs, anticoagulants:** Worsen bleeding 6. **Nasal measures:** Topical hemostasis (thrombin, hydrogen peroxide), gentle packing if needed [cite:Dhingra 8e Ch 6; Harrison 21e Ch 295] 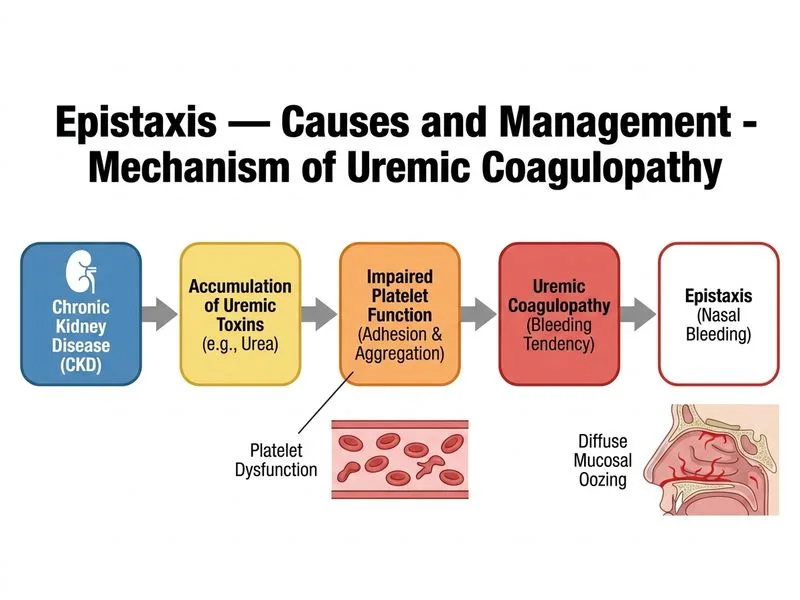
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.