## Management of Posterior Epistaxis with Coagulopathy **Key Point:** Posterior epistaxis in an anticoagulated patient requires simultaneous management of three components: (1) correct the coagulopathy, (2) achieve hemostasis via mechanical tamponade, (3) monitor for complications (airway, aspiration, sinusitis). ### Why This Is Posterior Epistaxis - Bleeding originates from branches of the **sphenopalatine artery** (terminal branch of maxillary artery) in the posterior nasal cavity - Presents as blood running down the pharynx (not anterior nosebleed) - Cannot be controlled by anterior packing alone - Requires hospital admission and closer monitoring ### Stepwise Management of Posterior Epistaxis ```mermaid flowchart TD A[Posterior epistaxis confirmed]:::outcome --> B[Establish IV access<br/>Type & cross-match]:::action B --> C[Correct coagulopathy if present]:::action C --> D[Topical vasoconstrictor<br/>4% lidocaine + epinephrine]:::action D --> E{Can visualize bleeding site?}:::decision E -->|Yes, accessible| F[Endoscopic cautery<br/>or clip placement]:::action E -->|No, or posterior| G[Posterior packing<br/>or Foley balloon]:::action G --> H[Admit ICU/HDU<br/>Monitor airway & O2]:::action H --> I{Rebleeding after 48-72 hrs?}:::decision I -->|Yes| J[Angiography &<br/>embolization]:::action I -->|No| K[Remove pack, discharge<br/>with precautions]:::outcome ``` ### Coagulopathy Reversal in This Case **High-Yield:** INR 8.5 is supratherapeutic and increases bleeding risk. Immediate reversal is essential: | Agent | Dose | Onset | Notes | |-------|------|-------|-------| | **Vitamin K (phytonadione)** | 10 mg IV slow infusion | 12–24 hours | Slow onset; always give | | **Fresh Frozen Plasma (FFP)** | 10–15 mL/kg (usually 2–4 units) | Immediate | Rapid reversal; volume overload risk | | **Prothrombin Complex Concentrate (PCC)** | 25–50 units/kg | Immediate | Preferred over FFP (less volume); not always available in India | **Clinical Pearl:** In this case, give **vitamin K + FFP immediately** (PCC if available). This achieves rapid INR reduction while vitamin K takes effect over hours. ### Why Posterior Packing or Foley Balloon? Unlike anterior epistaxis, posterior bleeding cannot be reached by simple anterior packing. Options include: 1. **Posterior nasal packing** — traditional but uncomfortable; requires sedation 2. **Foley catheter balloon** — less invasive; easier to manage; allows oral intake - Insert 14–16 Fr Foley catheter posteriorly - Inflate balloon with 10–15 mL saline - Pull anteriorly to tamponade posterior nasopharynx - Secure with tape 3. **Endoscopic cautery** — if bleeding vessel is visible and accessible; avoids packing **Warning:** Posterior packing carries risk of: - Airway obstruction - Aspiration - Sinusitis (requires prophylactic antibiotics) - Eustachian tube obstruction (otalgia, otitis media) - Hypoventilation if sedation is excessive → **Always admit to ICU/HDU for continuous monitoring.** ### Why NOT the Other Options? | Option | Why Incorrect | |--------|---------------| | **Observe for spontaneous hemostasis** | Posterior epistaxis rarely stops spontaneously, especially with INR 8.5; patient is already anemic (Hb 9.2); observation risks exsanguination and shock | | **Rigid endoscopy under local anesthesia** | Posterior bleeding is difficult to visualize and cauterize under local anesthesia alone; patient needs sedation/GA; packing is more reliable first-line for posterior bleeds | | **Immediate angiography without stabilization** | Premature escalation; should attempt mechanical tamponade first; angiography reserved for rebleeding after packing or when bleeding vessel is not accessible | **Mnemonic: POSTER** — **P**osterior epistaxis needs **O**pen IV, **S**tabilize coagulopathy, **T**amponade (packing/balloon), **E**nsure airway, **R**efer if rebleeds. ### Post-Packing Protocol 1. **Antibiotics:** Broad-spectrum (e.g., amoxicillin-clavulanate 625 mg TDS or cefixime 400 mg BD) to prevent sinusitis 2. **Monitoring:** Pulse oximetry, continuous observation for airway compromise 3. **Analgesia & sedation:** Paracetamol, NSAIDs (if not contraindicated), mild sedation if needed 4. **Anticoagulation:** Restart warfarin only after pack removal and hemostasis confirmed; bridge with LMWH if high thromboembolic risk 5. **Pack removal:** After 48–72 hours if no rebleeding 6. **Follow-up:** Repeat INR; adjust warfarin dose; consider alternative anticoagulation (DOAC) if recurrent epistaxis [cite:Robbins & Cotran 10e Ch 16; Harrison 21e Ch 47] 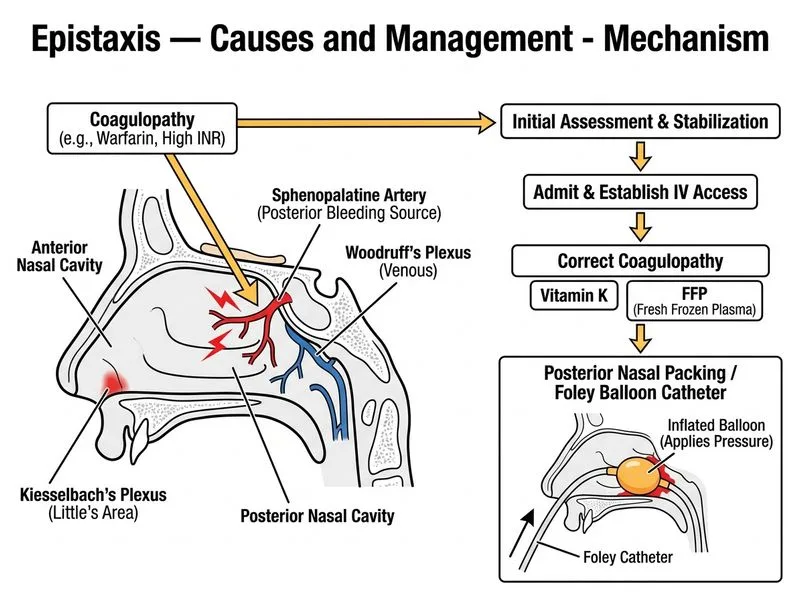
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.