## Diagnostic Approach to Suspected Ewing Sarcoma ### Clinical Presentation The patient presents with classic features of Ewing sarcoma: - Age: 10–20 years (peak incidence) - Location: diaphysis of long bones (femur most common) - Systemic signs: elevated ESR, local inflammation - Radiographic findings: mixed lytic-sclerotic lesion with periosteal reaction ("onion-skin" pattern) ### Next Step: Imaging and Biopsy **Key Point:** Before any treatment (chemotherapy or surgery), histopathological diagnosis MUST be established. Ewing sarcoma is a small round cell tumor requiring immunohistochemistry (CD99+, EWSR1-FLI1 translocation) for confirmation. **High-Yield:** The diagnostic sequence is: 1. **MRI** — gold standard for local staging, assesses soft tissue involvement, marrow edema, and surgical planning 2. **Biopsy** (core needle or open) — confirms diagnosis and identifies EWSR1-FLI1 translocation (present in ~95% of cases) 3. **Staging** (CT chest, bone scan, PET-CT) — performed AFTER diagnosis is confirmed ### Why MRI + Biopsy First? | Step | Purpose | Timing | |------|---------|--------| | MRI | Local staging, soft tissue assessment, surgical margins | Before biopsy | | Biopsy | Histology + molecular confirmation (EWSR1-FLI1) | Diagnostic | | Chemotherapy | Neoadjuvant (reduces tumor burden, improves survival) | After diagnosis | | Metastatic workup | CT chest, bone scan | After diagnosis | **Clinical Pearl:** Ewing sarcoma is chemosensitive. Neoadjuvant chemotherapy is standard of care, but it CANNOT be started without tissue diagnosis. Misdiagnosis as infection (due to elevated ESR and warmth) is a common trap. **Warning:** Do NOT skip biopsy or assume diagnosis from imaging alone. Osteomyelitis, osteosarcoma, and lymphoma can mimic Ewing sarcoma radiographically. 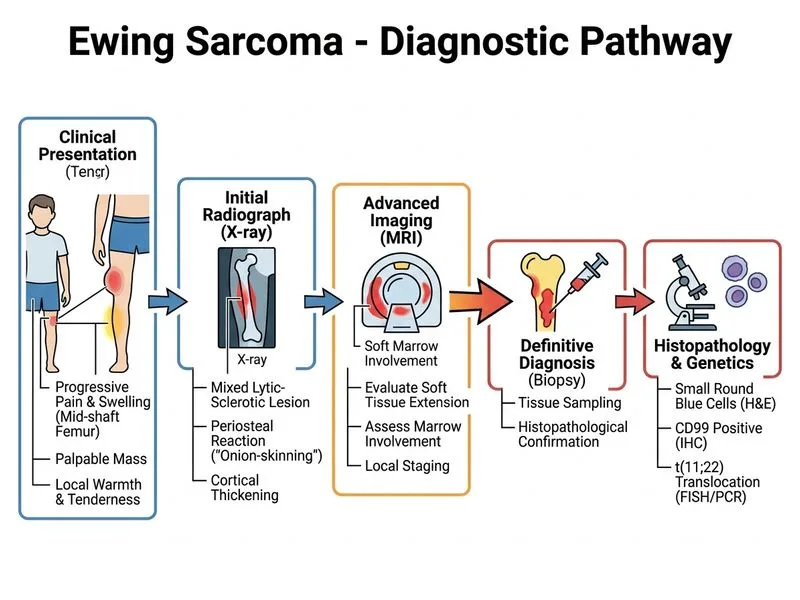
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.