## Clinical Presentation & Imaging Correlation **Key Point:** The 3-week history with insidious onset, crescent-shaped hypodense morphology, and crossing of the midline are classic features of **chronic subdural hematoma (cSDH)**. ### Why Chronic Subdural Hematoma? 1. **Timeline**: Symptoms develop over weeks (not hours/days as in acute SDH). The patient fell 2 weeks ago; cSDH typically presents 2–3 weeks post-injury. 2. **Imaging hallmark**: - Crescent-shaped collection (follows brain contour) - Hypodense on CT (chronic blood has lower density than acute) - Crosses the midline (subdural space is continuous across midline) 3. **Risk factors**: Advanced age + chronic alcoholism = brain atrophy + coagulopathy → increased risk of cSDH from minor head trauma. 4. **Neurological signs**: Drowsiness, confusion, and focal weakness are typical of mass effect from cSDH. ### Subdural vs Epidural: Key Distinguishing Features | Feature | Subdural Hematoma | Epidural Hematoma | |---------|-------------------|-------------------| | **Location** | Between dura and arachnoid | Between skull and dura | | **Shape on CT** | Crescent (follows brain contour) | Lens-shaped (biconvex) | | **Crosses midline?** | Yes (subdural space continuous) | No (limited by dural attachments) | | **Crosses sutures?** | Yes | No (stops at suture lines) | | **Typical onset** | Acute: hours; Chronic: weeks | Acute: hours (lucid interval common) | | **Common vessel** | Bridging veins (low pressure) | Middle meningeal artery (high pressure) | | **Age group** | Elderly, alcoholics, anticoagulated | Younger patients | | **Prognosis** | Worse (brain injury + hematoma) | Better if treated promptly | **High-Yield:** Chronic SDH is a "great imitator" — presents with dementia-like symptoms (confusion, gait disturbance) in elderly patients. Always obtain imaging in elderly with acute cognitive decline + minor head trauma. ### Pathophysiology of Chronic SDH 1. Initial bleeding from bridging veins (low-pressure system) 2. Organization phase: fibrin deposition, neomembrane formation (weeks 1–3) 3. Liquefaction: breakdown of clot, fluid accumulation 4. Hypodensity on CT reflects CSF-like density of chronic collection 5. Recurrent microhemorrhages → mixed density ("layered" appearance) **Clinical Pearl:** Chronic SDH can be treated conservatively (observation + head elevation) if small and asymptomatic, but symptomatic cases require burr hole drainage or craniotomy. This patient's drowsiness and focal weakness indicate surgical intervention. **Mnemonic: CHRONIC SDH = C-Crescent, H-Hypodense, R-Recurrent bleeds, O-Older patients, N-Neomembrane, I-Insidious onset, C-Crosses midline** [cite:Robbins 10e Ch 28] 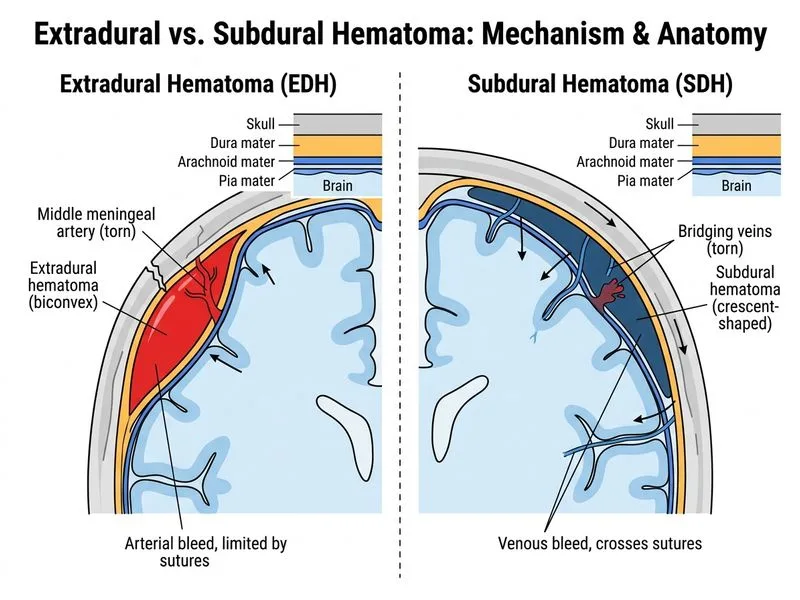
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.