## Acute Epidural Hematoma: Classic Presentation **Key Point:** The **lens-shaped (biconvex) hyperdense collection that does not cross the midline**, combined with the classic **"lucid interval"** (brief consciousness followed by rapid deterioration), is pathognomonic for **acute epidural hematoma (EDH)**. ### Why Epidural Hematoma? 1. **Lucid interval**: Patient was unconscious, then alert (classic for EDH). This occurs because the high-pressure arterial bleed accumulates slowly enough to allow brief consciousness before mass effect causes herniation. 2. **Imaging findings**: - **Lens-shaped (biconvex)** — bounded by dural attachments at suture lines - **Hyperdense** — acute blood (high protein content) - **Does not cross midline** — epidural space is limited by dural attachments - **Does not cross sutures** — dura is adherent to sutures 3. **Location**: Temporal region → suggests **middle meningeal artery (MMA) injury** (most common source of EDH). 4. **Age**: Younger patients (dura is less adherent to skull in youth, allowing blood to accumulate). 5. **Rapid deterioration**: Arterial bleeding (high pressure) causes rapid accumulation → acute mass effect → herniation. ### Epidural vs Subdural: Comparative Table | Feature | Epidural Hematoma | Subdural Hematoma | |---------|-------------------|-------------------| | **Vessel injured** | Middle meningeal artery (arterial) | Bridging veins (venous) | | **Pressure** | High → rapid accumulation | Low → slower accumulation | | **Shape** | Lens-shaped (biconvex) | Crescent-shaped | | **Crosses midline?** | No | Yes | | **Crosses sutures?** | No (stops at suture lines) | Yes | | **Density (acute)** | Hyperdense | Hyperdense | | **Density (chronic)** | Remains hyperdense longer | Becomes hypodense | | **Lucid interval** | Common (40–50%) | Rare | | **Age group** | Younger (dura less adherent) | Elderly, alcoholics | | **Prognosis** | Better if treated promptly | Worse (often brain injury) | | **Treatment** | Burr holes or craniotomy | Burr holes or craniotomy | **High-Yield:** The **lucid interval** is a red flag for EDH. Any patient with head trauma who becomes unconscious, then alert, then deteriorates again must be assumed to have EDH until proven otherwise. This is a neurosurgical emergency. ### Pathophysiology of Acute EDH 1. **Trauma** → fracture of temporal bone 2. **Laceration of MMA** (runs in grooves in skull) 3. **Arterial bleeding** into epidural space (between dura and skull) 4. **Mass effect** → compression of brain → increased ICP 5. **Herniation** → brainstem compression → coma, death **Clinical Pearl:** The classic presentation is a young patient with a **brief loss of consciousness, then a lucid interval of minutes to hours, followed by rapid deterioration with headache, vomiting, and coma**. This is a **neurosurgical emergency** requiring immediate burr hole drainage or craniotomy. Mortality is ~5–10% if treated promptly, but >80% if untreated. **Warning:** Do not discharge patients with head trauma and loss of consciousness without imaging, even if they appear well. The lucid interval can be deceptively reassuring. **Mnemonic: EDH = Epidural, Lens-shaped, Does not cross midline, High-pressure artery, Lucid interval** ```mermaid flowchart TD A[Head trauma with LOC]:::outcome --> B{Lucid interval?}:::decision B -->|Yes| C[Suspect EDH]:::action B -->|No| D[Consider SDH or DAI]:::action C --> E[CT head]:::action E --> F{Lens-shaped,<br/>does not cross midline?}:::decision F -->|Yes| G[Epidural hematoma]:::outcome F -->|No| H[Subdural hematoma]:::outcome G --> I[Neurosurgery:<br/>burr holes/craniotomy]:::action I --> J[Urgent decompression]:::urgent ``` [cite:Robbins 10e Ch 28] 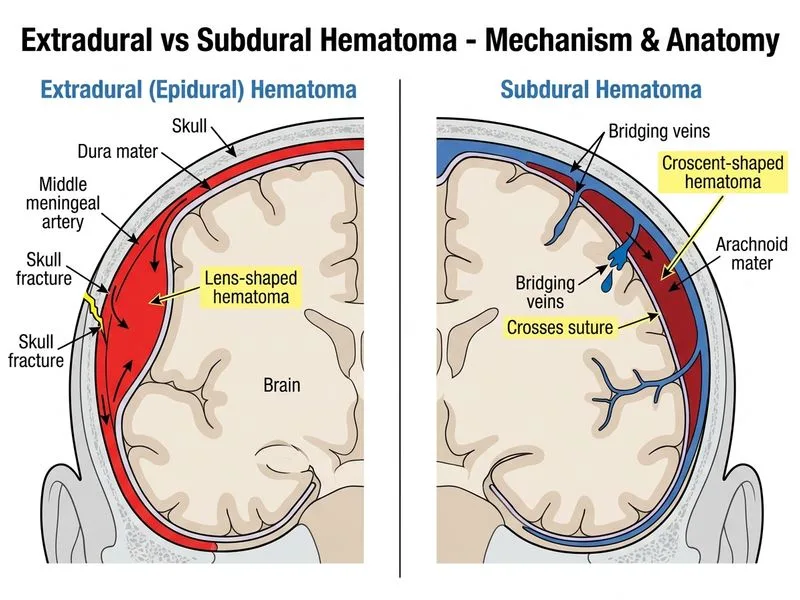
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.