## Clinical Presentation & Imaging Interpretation **Key Point:** This patient has an **acute epidural hematoma (EDH)** with favorable prognostic features: lens-shaped (biconvex), does NOT cross midline, stable vital signs, and relatively small thickness (8 mm). However, the mechanism (high-impact trauma) and brief loss of consciousness indicate risk of rapid deterioration. ### Epidural vs Subdural Hematoma: Quick Differential | Feature | Epidural Hematoma | Subdural Hematoma | | --- | --- | --- | | **Shape on CT** | Lens-shaped, biconvex | Crescent-shaped, concave | | **Crosses midline** | NO (stops at dural attachments/sutures) | YES (crosses falx/tentorium) | | **Location** | Between skull and dura | Between dura and arachnoid | | **Arterial source** | Middle meningeal artery | Bridging cortical veins | | **Typical onset** | Rapid (minutes to hours) | Slower (hours to days/weeks) | | **"Talk and die" syndrome** | Classic (lucid interval common) | Less common | | **Age at risk** | Younger (dura adherent to skull in elderly) | Elderly, alcoholics, anticoagulated | **Clinical Pearl:** The "talk and die" syndrome is pathognomonic for EDH — patient loses consciousness, regains consciousness (lucid interval), then deteriorates rapidly as hematoma expands and causes herniation. ### Management Algorithm for Acute Epidural Hematoma ```mermaid flowchart TD A[Acute EDH diagnosed]:::outcome --> B{Thickness & midline shift?}:::decision B -->|>30 mm or >5 mm shift| C[Emergency burr hole/craniotomy]:::urgent B -->|<30 mm, <5 mm shift, stable neuro| D{Neurologically stable?}:::decision D -->|Yes| E[Serial CT + ICU monitoring]:::action D -->|No| C E --> F[Repeat CT at 6-24 hrs]:::action F --> G{Progression?}:::decision G -->|Yes| C G -->|No| H[Continue monitoring, consider discharge if stable]:::action C --> I[Evacuation via burr hole/craniotomy]:::action ``` ### Why Serial CT & ICU Monitoring Is Correct **High-Yield:** This EDH is **small** (8 mm) with **minimal midline shift** (implied by stable vitals and mild confusion only). Current guidelines support **conservative management** for small, hemodynamically stable EDH. 1. **Thickness 8 mm** is below the 30 mm threshold for mandatory surgery 2. **No mention of midline shift** and stable vitals suggest low immediate herniation risk 3. **Serial CT** is essential because EDH can expand rapidly (arterial bleeding) 4. **ICU monitoring** allows detection of deterioration requiring urgent evacuation 5. **Close neuro checks** enable early intervention if patient declines **Mnemonic: SAFE-EDH** — **S**mall (<30 mm), **A**lert/stable, **F**ew neuro deficits, **E**arly imaging = Safe for observation with serial imaging. ### Why Each Wrong Option Fails **Emergency burr hole (Option 1):** Reserved for large EDH (>30 mm), significant midline shift, or neurological deterioration. This patient is hemodynamically stable with a small collection. **Intubation & hyperventilation (Option 2):** Hyperventilation is a temporizing measure for raised ICP in emergencies (target PaCO~2~ 30–35 mmHg), but it is NOT the next step here. The patient is alert and breathing spontaneously. Intubation without clear indication increases aspiration risk and ICU complications. **Ward observation (Option 4):** Inadequate. EDH can expand rapidly due to ongoing arterial bleeding. This patient requires **ICU-level monitoring** with capability for emergency imaging and intervention, not ward-level care. [cite:Harrison 21e Ch 445; Robbins 10e Ch 28] 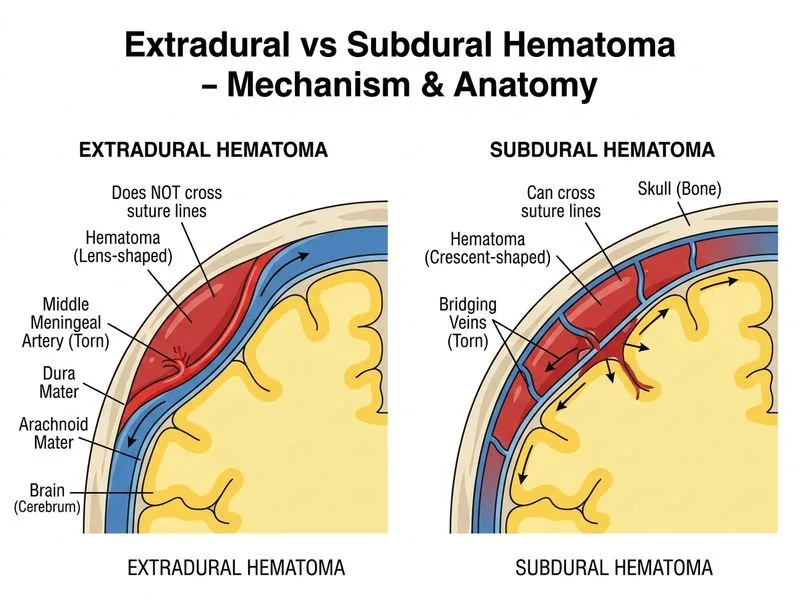
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.