## Clinical Diagnosis: Infected Femoral Lymph Node / Lymph Node Abscess in Femoral Triangle ### Anatomical Substrate of the Femoral Triangle **Key Point:** The femoral triangle contains not only the femoral artery and vein, but also lymph nodes and lymphatic vessels. These are often overlooked but clinically significant. ### Contents of the Femoral Triangle (NAVEL mnemonic) | Structure | Position | Vulnerability to Catheterization | |-----------|----------|----------------------------------| | **N**erve (femoral) | Lateral (outside triangle proper) | Protected by lateral position; less likely to be punctured | | **A**rtery (femoral) | Central | Protected by firm muscular wall; direct puncture causes pseudoaneurysm, not abscess | | **V**ein (femoral) | Medial to artery | Medial position; less commonly punctured than artery | | **E**ly's fascia | Investing layer | — | | **L**ymphatics & nodes | Throughout triangle | Superficial, easily punctured; prone to infection if contaminated | **High-Yield:** Femoral lymph nodes lie within the femoral triangle, anterior and medial to the femoral vessels. They are frequently in the trajectory of femoral artery puncture, especially if the needle is angled medially or if multiple passes are made. ### Why Lymph Node Abscess Develops 1. **Mechanical trauma:** Needle puncture during catheterization breaches the lymph node capsule 2. **Bacterial seeding:** Skin flora (Staph aureus) introduced along the needle tract 3. **Lymphoid tissue vulnerability:** Lymph nodes are highly vascularized and immunologically active — ideal substrate for bacterial proliferation 4. **Abscess formation:** Localized suppuration within the node, creating a fluctuant collection 5. **Clinical presentation:** Fever, tender swelling 2–5 days post-procedure (timeline matches) ### Pathophysiology of Post-Catheterization Infection ```mermaid flowchart TD A[Femoral artery catheterization]:::action --> B[Needle traverses skin & subcutaneous tissue]:::action B --> C{Needle trajectory}:::decision C -->|Medial/multiple passes| D[Femoral lymph node puncture]:::outcome C -->|Central| E[Femoral artery/vein injury]:::outcome D --> F[Bacterial seeding into node]:::action F --> G[Suppurative lymphadenitis]:::outcome G --> H[Abscess formation]:::outcome H --> I[Fever, tender fluctuant mass]:::outcome E --> J[Pseudoaneurysm/AVF]:::outcome ``` ### Clinical Features Supporting Lymph Node Abscess | Feature | Explanation | |---------|-------------| | **Timing (3 days)** | Consistent with acute bacterial infection; pseudoaneurysm would present within 24 hrs | | **Fever 38.5°C** | Systemic inflammatory response to localized infection | | **Fluctuant swelling** | Pus collection within lymph node; not seen with nerve or muscle injury | | **Positive blood cultures** | Indicates bacteremia from infected lymphoid tissue | | **Ultrasound: 4 cm fluid collection** | Hypoechoic/anechoic collection typical of abscess; separate from artery rules out pseudoaneurysm | | **Staph aureus** | Common skin flora; consistent with iatrogenic inoculation | **Clinical Pearl:** Femoral lymph node abscess is an underrecognized complication of femoral artery procedures. The nodes lie in the superficial tissues of the triangle and are easily accessible to needle trauma. ### Why NOT the Other Structures **Femoral nerve:** Located laterally, outside the triangle proper; not in the direct path of femoral artery puncture. Nerve injury would cause motor/sensory deficits, not abscess. **Saphenous vein:** Superficial vein; puncture would cause hematoma or thrombophlebitis, not a deep abscess. Venous injury is less likely to seed bacteria. **Pectineus muscle:** Deep structure; not typically in the needle trajectory. Muscle injury would cause hematoma, not abscess with fever and positive blood cultures. ### Management 1. **Imaging:** Ultrasound or CT to confirm abscess 2. **Microbiology:** Blood cultures, aspiration culture if accessible 3. **Antibiotics:** Empiric anti-staphylococcal coverage (e.g., cloxacillin or vancomycin) 4. **Drainage:** Percutaneous needle aspiration or ultrasound-guided catheter drainage if >3 cm 5. **Monitoring:** Serial imaging to assess response **Mnemonic: LYMPH = Lymph nodes in femoral triangle, Yieldable to needle, Microbes seeded, Pus forms, Host inflammatory response** 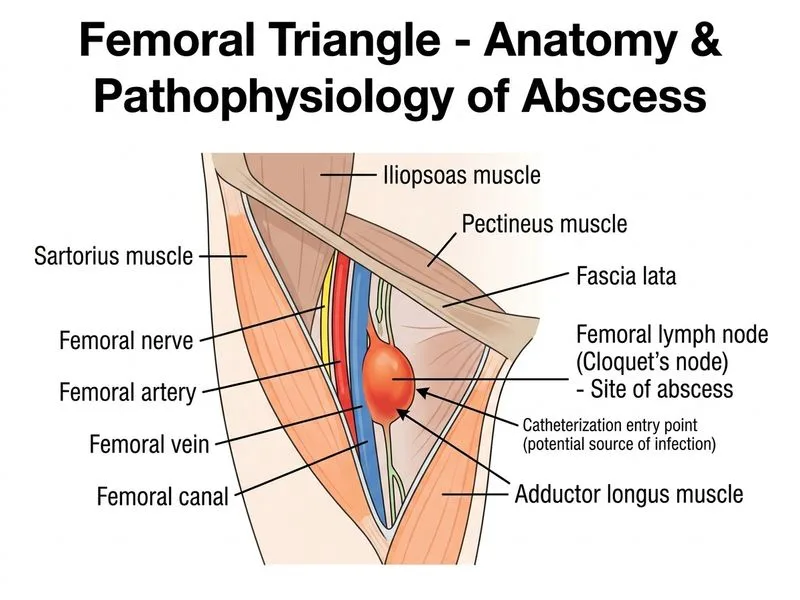
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.