## Transposition of the Great Arteries (TGA) — Neonatal Emergency ### Clinical Recognition **High-Yield:** The classic triad of D-TGA: - **Severe cyanosis unresponsive to oxygen** (SpO₂ 60% on 100% FiO₂) — pathognomonic for parallel circulations with no effective mixing - **'Egg-on-string' (egg-on-a-side) appearance** on CXR — narrow superior mediastinum due to AP arrangement of aorta and pulmonary artery, with an oval cardiac silhouette - **Maternal diabetes** — a well-established risk factor for D-TGA (KD Tripathi; Nelson's Textbook of Pediatrics) **Key Point:** D-TGA is a **duct-dependent lesion for systemic oxygenation**. The ductus arteriosus (and foramen ovale) are the only mixing points between the two parallel circuits. As the ductus closes in the first hours of life, cyanosis and shock worsen precipitously. ### Why PGE₁ is the MOST APPROPRIATE IMMEDIATE Next Step | Priority | Action | Rationale | |----------|--------|-----------| | **1 (Immediate)** | **Initiate PGE₁ infusion (0.05–0.1 μg/kg/min)** | Reopens/maintains ductus arteriosus; restores mixing; is life-saving and must NOT be delayed | | **2** | Prepare for urgent cardiac catheterization / Rashkind procedure | Once stabilized with PGE₁, echo confirms anatomy and Rashkind septostomy improves mixing further | | **3** | Echocardiography + cardiology consult | Confirms diagnosis and guides definitive planning | | **4** | Arterial switch operation (Jatene) | Definitive repair within 2 weeks of life | **Clinical Pearl (Harrison's / Nelson's):** In any cyanotic neonate with suspected duct-dependent congenital heart disease, **PGE₁ infusion must be started immediately — before echocardiographic confirmation** — because the risk of ductal closure causing cardiovascular collapse far outweighs the risk of PGE₁ in a non-duct-dependent lesion. Delaying PGE₁ to obtain echo first is a dangerous error. ### Why Option A (Echo + Cardiology Consult) is Incorrect as the IMMEDIATE Next Step While echocardiography and cardiology consultation are essential, they are **not the most immediate priority** in a hemodynamically crashing neonate. PGE₁ must be started first to stabilize the infant; echo follows to confirm anatomy and guide the Rashkind procedure. Option C correctly captures this sequence: start PGE₁ NOW, then proceed to cardiac catheterization/Rashkind. ### Why Option D (Indomethacin) is Dangerous Indomethacin closes the ductus arteriosus — the exact opposite of what is needed in TGA. This would be immediately fatal. ### Why Option B (Immediate Bedside Rashkind) is Incorrect Balloon atrial septostomy requires fluoroscopy or echocardiographic guidance and is performed in a catheterization lab or NICU with echo guidance — not as a blind bedside procedure. PGE₁ stabilizes the infant first. **Mnemonic:** **PGE₁ FIRST** — Prostaglandin keeps the duct open; Give it before echo; Echo confirms; then Rashkind; Surgical switch follows. **Key Point:** Per Nelson's Textbook of Pediatrics (21st ed.) and standard neonatal cardiology protocols, **PGE₁ infusion is the single most important immediate intervention** in suspected duct-dependent cyanotic CHD, including TGA with shock. 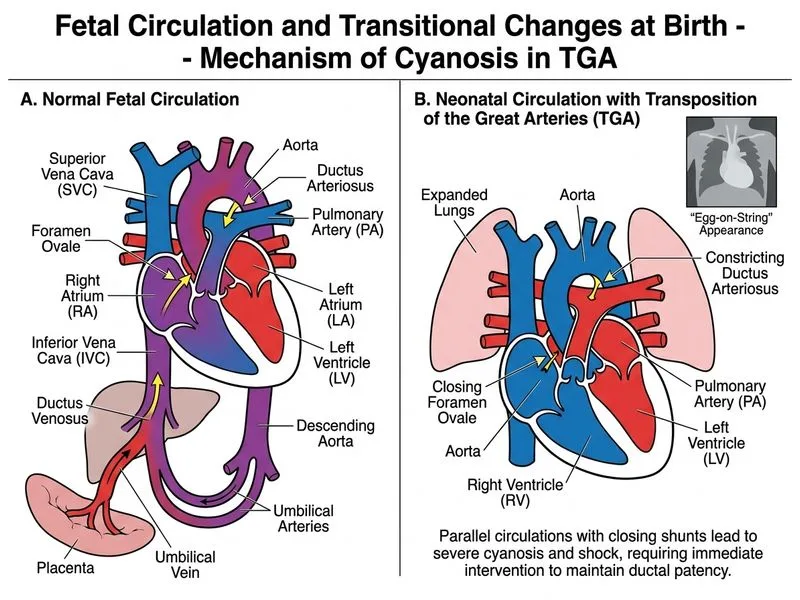
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.