## Clinical Context **Key Point:** A rapidly enlarging breast mass (3.5 cm over 4 months) in a 35-year-old woman, even with benign imaging features, raises concern for a phyllodes tumour. When the patient requests removal, **excision biopsy** is the preferred next step — it simultaneously achieves definitive diagnosis and treatment in a single procedure. **High-Yield:** Phyllodes tumours (0.3–0.9% of breast tumours) are notoriously difficult to distinguish from fibroadenoma on clinical examination and ultrasound. Histology — specifically the stromal architecture — is required for definitive differentiation (Bailey & Love's Short Practice of Surgery; Bland & Copeland, The Breast). ## Why Excision Biopsy (Option C) Is Correct | Indication | Rationale | |-----------|----------| | **Rapid growth** | 4 months of noticeable enlargement is a red flag for phyllodes or malignancy | | **Patient request for removal** | Symptomatic concern + patient autonomy = valid surgical indication | | **Diagnostic uncertainty** | Imaging cannot exclude phyllodes; tissue diagnosis is mandatory | | **Size (3.5 cm)** | Approaching giant fibroadenoma threshold (>4 cm); excision is appropriate | | **Single-step management** | Excision provides both diagnosis (histology) and treatment, avoiding a second procedure | ## Why Core Needle Biopsy (Option B) Is Not the Best Next Step Here Core needle biopsy (CNB) is a valid diagnostic tool and is preferred in some centres as a first step before excision. However, in this specific scenario, excision biopsy is superior because: 1. **The patient has already requested removal** — proceeding directly to excision avoids an additional invasive procedure (CNB) before the inevitable surgery. 2. **CNB has sampling limitations for phyllodes** — CNB may miss the heterogeneous stromal component of phyllodes tumours, leading to false-negative results; excision provides the entire lesion for histological assessment. 3. **Size and growth rate** — at 3.5 cm with rapid growth, the lesion meets standard surgical criteria regardless of CNB result. 4. **Guidelines (NICE CG164; NCCN Breast)** — for symptomatic fibroadenomas >3 cm or with rapid growth where the patient desires removal, excision is recommended as definitive management. > **Note:** CNB before excision is an acceptable alternative in centres where surgical planning requires pre-operative tissue diagnosis (e.g., to counsel about margins for phyllodes). However, when the patient has already consented to removal, excision biopsy is the most efficient and definitive next step. ## Why Other Options Are Incorrect - **Option A (Repeat ultrasound in 3 months):** Watchful waiting is inappropriate when there is rapid growth and the patient requests removal. Delay risks missing a phyllodes tumour or malignancy. - **Option D (Tamoxifen):** Hormonal therapy has no established role in the management of fibroadenoma or phyllodes tumour. Tamoxifen is used for ER-positive breast cancer, not benign breast disease. **Clinical Pearl:** Phyllodes tumours are characterised by rapid growth, large size, and a leaf-like stromal architecture on histology (phyllodes = Greek for "leaf"). They range from benign to malignant. Any rapidly enlarging breast mass warrants excision and histological examination — imaging alone is insufficient. **Mnemonic:** **RAPID** growth in a breast lump = **R**equires **A**nalysis **P**athologically — **I**mmediately **D**iagnose with excision biopsy when removal is requested. **Reference:** Bailey & Love's Short Practice of Surgery, 27th ed., Chapter on Breast Disease; NICE Clinical Guideline CG164 (Early and Locally Advanced Breast Cancer). 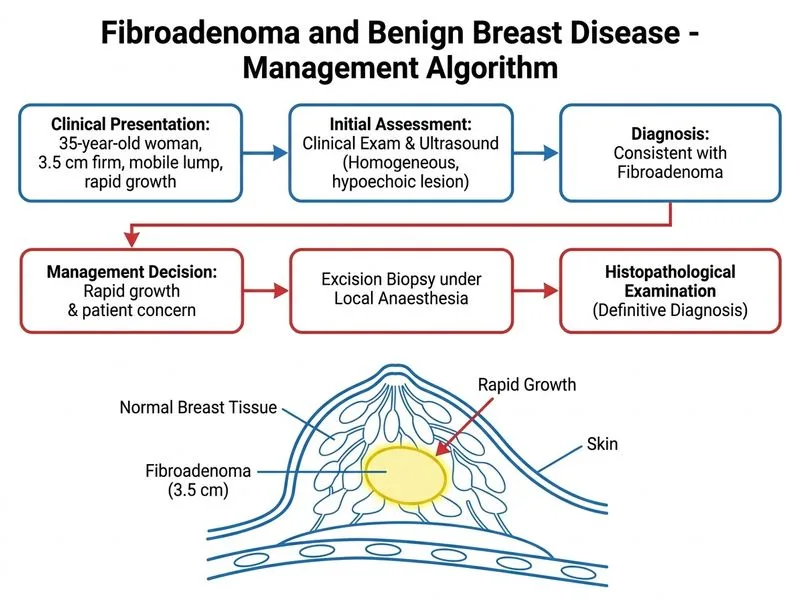
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.