## Clinical Presentation & Diagnostic Challenge This patient presents with features that blur the boundary between **fibroadenoma** and **phyllodes tumor**: - **Fibroadenoma features**: young age, mobile, well-defined, non-tender - **Concerning features**: rapid growth (4 months), heterogeneous echotexture, indistinct margins, increased vascularity **Key Point:** Phyllodes tumors are rare (0.3–0.9% of breast tumors) but can mimic fibroadenoma clinically and radiologically. They are biphasic tumors (epithelial + stromal) with potential for malignant transformation (5–10% of phyllodes are malignant). ## Why Core Needle Biopsy Is Indicated ### Diagnostic Uncertainty Requires Tissue Confirmation 1. **Imaging is equivocal**: The combination of heterogeneous echotexture, indistinct margins, and increased vascularity raises suspicion for phyllodes tumor. 2. **Clinical concern**: Rapid growth over 4 months is atypical for simple fibroadenoma and suggests stromal proliferation. 3. **Tissue diagnosis needed**: Histology (epithelial-stromal ratio, stromal cellularity, mitotic activity) is the only way to differentiate fibroadenoma from benign/borderline/malignant phyllodes. 4. **Guides surgical approach**: If benign fibroadenoma, local excision suffices. If phyllodes (especially borderline/malignant), wide local excision with adequate margins (1–2 cm) is required. **High-Yield:** **CNB is the gold standard for diagnostic uncertainty in breast masses.** It avoids unnecessary imaging delays and provides tissue for definitive classification. ### Core Needle Biopsy Advantages | Advantage | Benefit | |-----------|----------| | **Tissue diagnosis** | Differentiates fibroadenoma from phyllodes; grades phyllodes if present | | **Outpatient procedure** | Performed under ultrasound guidance; no general anesthesia needed | | **Cost-effective** | Cheaper than MRI; avoids unnecessary imaging | | **Prognostic information** | Stromal grade guides surgical margins and follow-up | | **Definitive** | Histology is the gold standard; imaging alone cannot exclude malignancy | ## Why Other Options Are Incorrect ### MRI (Option A) **Clinical Pearl:** While MRI has high sensitivity for breast lesions, it does NOT differentiate fibroadenoma from phyllodes reliably. Both appear as well-circumscribed masses on MRI. MRI is useful for staging known malignancy or assessing contralateral breast, NOT for diagnosis of uncertain benign vs. borderline lesions. ### Excision with Frozen Section (Option C) - **Unnecessary escalation**: Frozen section is used intraoperatively to assess margins in known malignancy, not for primary diagnosis of uncertain lesions. - **Delays diagnosis**: Excision commits the patient to surgery before tissue diagnosis is confirmed. - **Inadequate margins if malignant**: If phyllodes is discovered intraoperatively, the initial excision may have inadequate margins, necessitating re-excision. - **Better to biopsy first**: CNB provides diagnosis preoperatively, allowing planned wide excision if phyllodes is confirmed. ### Observation (Option D) - **Rapid growth is concerning**: A 4-month doubling time is atypical for fibroadenoma and suggests stromal proliferation (phyllodes). - **Risk of delay**: Observation postpones diagnosis and may allow a malignant phyllodes to progress. - **Not safe without diagnosis**: In the face of diagnostic uncertainty and rapid growth, observation is inappropriate. ## Management Algorithm ```mermaid flowchart TD A[Breast mass with uncertain imaging]:::outcome --> B{Diagnostic certainty?}:::decision B -->|Clear benign on imaging| C[Observation or excision per patient preference]:::action B -->|Equivocal or concerning features| D[Core needle biopsy]:::action D --> E{Histology result}:::decision E -->|Benign fibroadenoma| F[Local excision if symptomatic; observation if asymptomatic]:::action E -->|Benign phyllodes| G[Wide local excision 1-2 cm margins]:::action E -->|Borderline/malignant phyllodes| H[Wide local excision + imaging to exclude metastases]:::urgent E -->|Suspicious for malignancy| I[Excision + oncologic staging]:::urgent ``` ## Summary **Key Point:** In a young woman with a breast mass showing rapid growth and equivocal imaging features, **core needle biopsy is the standard next step** to obtain tissue diagnosis and differentiate fibroadenoma from phyllodes tumor. This guides surgical planning and ensures appropriate margins if malignancy is present. [cite:Robbins 10e Ch 24; Park 26e Ch 3] 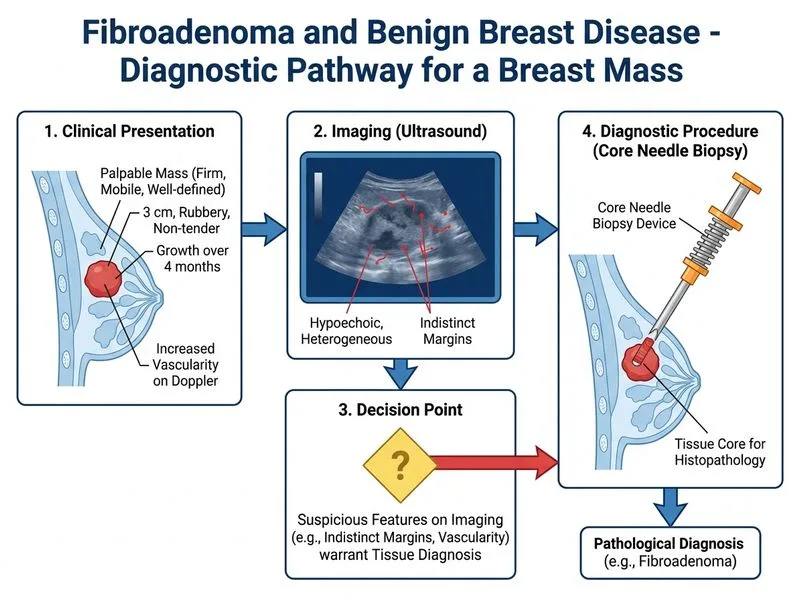
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.