## Investigation Before Rigid Bronchoscopy in Suspected Airway Foreign Body ### Clinical Scenario Analysis The child has: - **Chronic presentation (2 weeks)** with persistent cough, recurrent low-grade fever - **Radiological evidence**: left lower lobe collapse + left upper lobe hyperinflation - **Suspected location**: left main bronchus - **Stable child** — no acute respiratory distress The question asks for the most appropriate **next investigation** before rigid bronchoscopy — a diagnostic step to confirm localization and assess the nature and surrounding airway changes. ### Why Flexible Fibreoptic Bronchoscopy (FFB) is Correct **Key Point:** In a stable child with a chronic (>1 week) suspected airway foreign body, **flexible fibreoptic bronchoscopy (FFB)** is the most appropriate diagnostic investigation before proceeding to rigid bronchoscopy. It allows direct visualization, precise localization, and assessment of secondary airway changes without requiring general anaesthesia. **High-Yield Advantages of FFB in this context:** 1. **Direct visualization** of the foreign body and surrounding mucosa 2. **Precise localization** — confirms which bronchus/segment is involved 3. **Assessment of secondary changes** — edema, granulation tissue, mucopus (critical in chronic FB >1 week) 4. **Performed under topical anaesthesia ± light sedation** — avoids GA risk at this diagnostic stage 5. **Guides the rigid bronchoscopist** on approach, expected difficulty, and instrument selection **Clinical Pearl:** In chronic foreign body aspiration (>1 week), significant granulation tissue, mucosal edema, and secondary infection may develop around the FB. FFB allows pre-operative assessment of these changes, enabling better planning of the rigid bronchoscopy and reducing intraoperative complications. *(Dhingra's Diseases of Ear, Nose & Throat, 7th ed., Ch. 16)* ### Why the Other Options Are Less Appropriate | Option | Reason Not Preferred | |---|---| | **A — Immediate rigid bronchoscopy** | Requires GA; appropriate as definitive therapy, not as a pre-operative investigation in a stable child | | **C — Inspiratory/expiratory X-rays** | Already have CXR evidence; additional plain films add little when FB is already radiologically suspected | | **D — CT chest** | Increasingly used in modern practice for pre-operative planning in chronic/complex cases, but **not the standard next step** per ENT guidelines before rigid bronchoscopy in a stable child with clear radiological and clinical evidence | **Note on CT Chest (Option D):** While CECT chest is gaining acceptance in complex or atypical cases (radiolucent FB, uncertain localization, or failed prior retrieval), standard ENT texts (Dhingra, Scott-Brown) recommend FFB as the preferred diagnostic step before rigid bronchoscopy in stable pediatric patients with chronic FB aspiration. CT exposes the child to radiation and delays definitive management without adding the direct mucosal assessment that FFB provides. ### Diagnostic Sequence in Airway Foreign Body (Stable Child) ``` Clinical suspicion → Chest X-ray (inspiratory + expiratory) → If FB suspected and child stable → Flexible fibreoptic bronchoscopy → Localize FB, assess airway mucosa → Plan and perform Rigid bronchoscopy + FB removal → Post-removal CXR ``` **Mnemonic — FLEX before RIGID:** - **F**irst-line diagnostic tool in stable child - **L**ocalization of foreign body - **E**valuation of airway mucosa (edema, granulation, infection) - **X**-ray findings confirmed by direct visualization [cite: Dhingra's Diseases of Ear, Nose & Throat, 7th ed., Ch. 16; Scott-Brown's Otorhinolaryngology, 8th ed.] 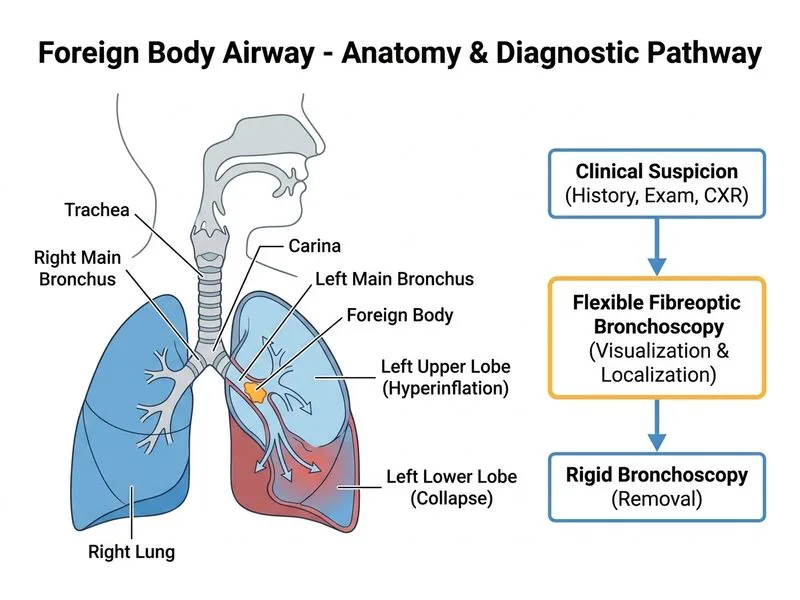
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.