## Clinical Context This is a vascular emergency superimposed on a fracture. The absent dorsalis pedis pulse, cold and pale limb, and comminuted displaced femur fracture indicate **acute limb ischaemia** — a true surgical emergency requiring immediate vascular surgery involvement. ## Why Immediate Vascular Surgery Consultation and Angiography is Correct **Key Point:** In a fracture with **hard signs of vascular injury** (absent pulse, cold/pale limb, ischaemia), the **immediate next step** is vascular surgery consultation alongside angiography to define the injury and plan operative repair. Time to revascularisation is the critical determinant of limb salvage. **Clinical Pearl (Rockwood & Green; Rutherford's Vascular Surgery):** Hard signs of vascular injury — pulselessness, pallor, paraesthesia, pain, paralysis (the "5 Ps") — mandate **immediate vascular surgery consultation**. While gentle fracture realignment may be attempted concurrently, it does NOT replace vascular assessment and should not delay the surgical team. In a comminuted femur fracture, the femoral or popliteal artery may be transected or thrombosed, not merely kinked — simple reduction will not restore flow in such cases. **High-Yield:** The management sequence for fracture + vascular injury with hard ischaemia signs: 1. **Immediate vascular surgery consultation** — concurrent with resuscitation 2. **Angiography (conventional or CT)** — to localise injury and plan repair 3. **Fracture stabilisation** (external fixator or traction) — done in coordination with vascular repair in the OR 4. **Revascularisation** — within 6 hours to prevent irreversible ischaemia ## Why Option A (Skeletal Traction) is Incorrect Applying skeletal traction and arranging operative fixation without first addressing the vascular emergency is inappropriate. Traction alone will not restore perfusion to an ischaemic limb with a transected or thrombosed vessel. The vascular injury must be identified and repaired urgently. ## Why Option C (CT Angiography First) is Incorrect Performing CT angiography *before any intervention* is inappropriate when the limb is already ischaemic with hard signs. In the presence of hard signs, the patient should go directly to the operating room; imaging should not delay revascularisation beyond what is clinically necessary. Angiography is performed as part of the vascular surgery workup, not as a standalone pre-intervention step that delays consultation. ## Why Option D (Closed Reduction First) is Incorrect Attempting closed reduction as the *first* step is inappropriate when hard signs of vascular injury are present. In a comminuted fracture, the vessel may be lacerated or thrombosed — reduction alone will not restore perfusion and wastes critical ischaemia time. The priority is to get the vascular surgery team involved immediately so operative revascularisation can proceed without delay. ## Rationale for Sequence | Step | Timing | Rationale | |------|--------|-----------| | Vascular surgery consult + angiography | Immediate | Define injury; plan operative repair | | Fracture stabilisation | In OR, concurrent with vascular repair | Provides stable platform for anastomosis | | Revascularisation | Within 6 hours | Prevents irreversible muscle/nerve ischaemia | | Post-op monitoring | ICU | Watch for reperfusion injury, compartment syndrome | **High-Yield:** For NEET PG / INI-CET: when a fracture stem describes **absent pulses + cold/pale limb**, the answer is **immediate vascular surgery consultation**, not closed reduction alone. Reduction may be part of the operative plan but does not precede vascular team involvement. 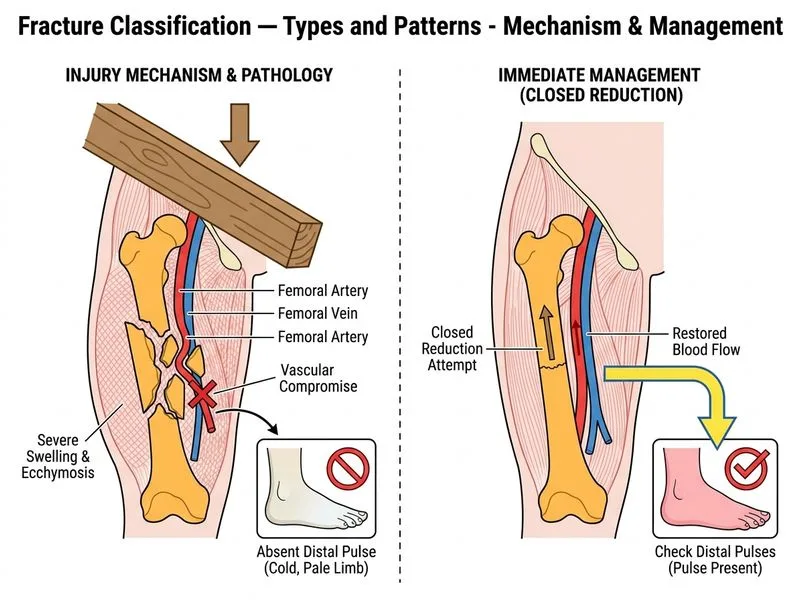
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.