## Distinguishing Acute Cholecystitis from Biliary Colic ### Key Pathophysiologic Difference **Key Point:** Biliary colic is transient obstruction of the cystic duct by a stone without inflammation; acute cholecystitis is cystic duct obstruction WITH secondary inflammation and tissue injury. ### Comparison Table | Feature | Biliary Colic | Acute Cholecystitis | | --- | --- | --- | | **Gallstones** | Present (required) | Present (90% of cases) | | **Fever** | Absent | Present (70–80% of cases) | | **WBC elevation** | Normal | Elevated (>10,000/μL) | | **CRP/inflammatory markers** | Normal | Elevated | | **Murphy's sign** | Negative | Positive | | **Pain duration** | 30 min – 2 hours | > 6 hours, often 12–72 hours | | **Gallbladder wall** | Normal | Thickened (>3 mm) | | **Pericholecystic fluid** | Absent | Present | ### Why Systemic Inflammation is the Discriminator **High-Yield:** Fever, elevated WBC, and elevated inflammatory markers (CRP, procalcitonin) indicate **tissue injury and bacterial invasion/translocation**, which occur only in acute cholecystitis. Biliary colic causes pain from visceral distension and smooth muscle spasm alone — no inflammation. **Clinical Pearl:** A patient with gallstones and RUQ pain but NO fever and normal WBC likely has biliary colic; the same patient WITH fever and leukocytosis has acute cholecystitis until proven otherwise. ### Why Other Options Are Not Discriminators 1. **Gallstones on imaging** — Present in both conditions; 80% of people with gallstones never develop symptoms. 2. **RUQ pain > 6 hours** — While acute cholecystitis typically lasts longer, biliary colic can occasionally persist 2–3 hours; overlap exists. 3. **Positive Murphy's sign** — Highly specific for cholecystitis but can be absent in 20–30% of cases; not a universal discriminator. [cite:Sabiston Textbook of Surgery 21e Ch 54] 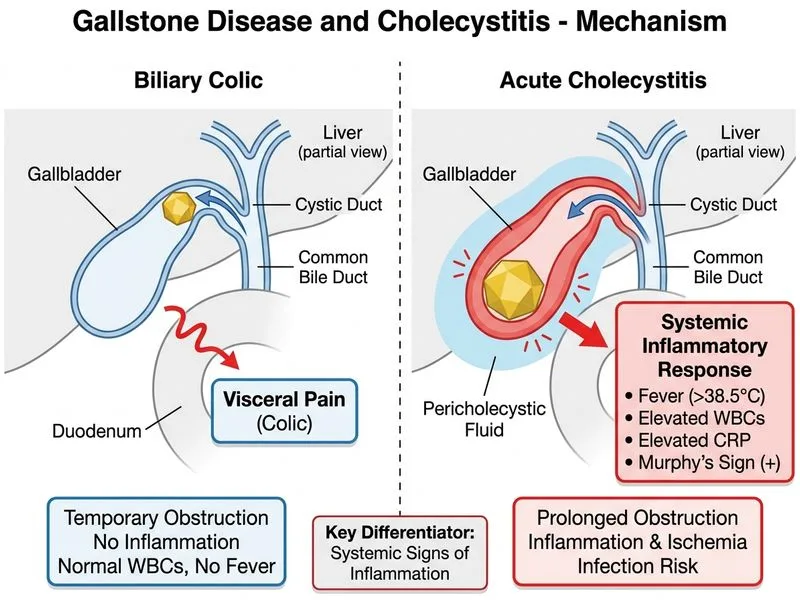
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.