## Clinical Diagnosis **Key Point:** This patient has **acute cholecystitis complicated by sepsis** (fever, hypotension, toxic appearance, elevated WBC, free intraperitoneal fluid suggesting possible perforation or peritonitis). ## Diagnostic Features of Complicated Acute Cholecystitis | Feature | Finding | Significance | |---------|---------|---------------| | **Wall thickness** | 6 mm (normal <3 mm) | Severe inflammation | | **Pericholecystic fluid** | Extensive | Peritoneal irritation | | **Free intraperitoneal fluid** | Present | Suggests perforation or spreading peritonitis | | **Haemodynamic status** | Hypotensive (100/62) | Septic shock | | **WBC** | 16,000/μL | Severe systemic response | | **Bilirubin** | Normal (1.2 mg/dL) | Rules out CBD obstruction | **High-Yield:** The presence of **hypotension, fever, and free intraperitoneal fluid** indicates **sepsis and possible perforation** — this is a surgical emergency requiring **immediate intervention**. ## Management Strategy **Clinical Pearl:** In a septic patient with complicated acute cholecystitis: 1. **Immediate resuscitation:** IV fluids, broad-spectrum antibiotics (piperacillin-tazobactam or carbapenems), vasopressors if needed 2. **Definitive source control:** Either - **Open cholecystectomy** (preferred if patient can tolerate general anaesthesia and the surgeon is experienced) — allows exploration for perforation, peritoneal lavage, and definitive removal - **Percutaneous cholecystostomy** (if patient is too unstable for surgery or has severe comorbidities) — allows drainage and stabilization; definitive cholecystectomy deferred to 6–8 weeks **Mnemonic: SEPTIC GALLBLADDER = DRAIN OR CUT** - **S**epsis / **E**xcessive inflammation - **P**erforation risk / **T**oxic appearance - **I**mmediate intervention needed - **C**holecystostomy (if unfit) or **C**holecystectomy (if fit) ## Why NOT Laparoscopic Cholecystectomy? **Warning:** Laparoscopy is **contraindicated in septic shock** and suspected perforation because: - Risk of tension pneumoperitoneum and cardiovascular collapse - Difficult to manage perforation and peritoneal lavage laparoscopically - Conversion to open surgery increases morbidity in unstable patients **Tip:** In sepsis, **open surgery or percutaneous drainage** is the safest approach. ## Why NOT ERCP? - Bilirubin is **normal** (1.2 mg/dL); no evidence of CBD obstruction - ERCP would delay source control in a septic patient - No indication for biliary decompression ## Why NOT Conservative Management? - **Septic shock** requires **immediate source control** (surgery or drainage) - Conservative management alone will lead to multi-organ failure and death - Free intraperitoneal fluid suggests perforation, which cannot be managed medically 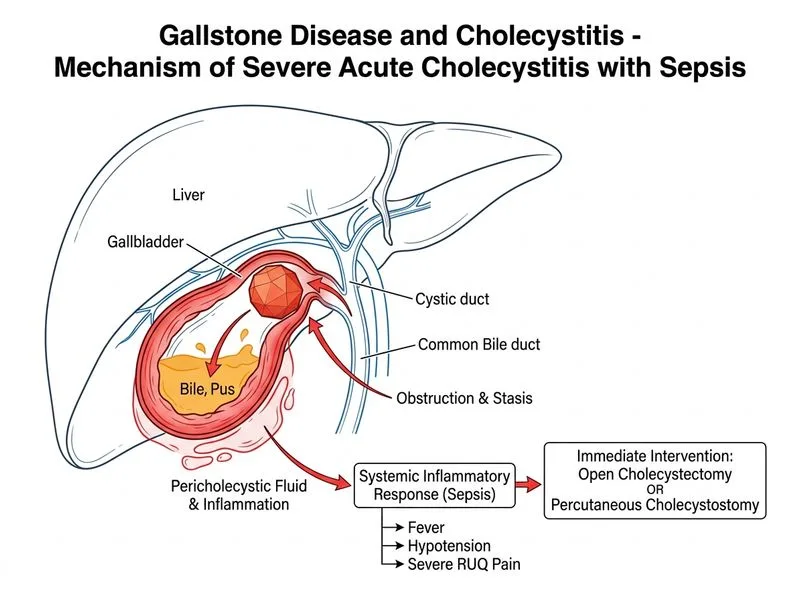
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.