## Clinical Scenario Analysis The described defect is **gastroschisis** — a full-thickness anterior abdominal wall defect of embryological origin, arising from failure of the lateral body folds to fuse during weeks 6–10 of gestation. The defect is typically to the right of the umbilicus and lacks peritoneal and skin coverage. ## Embryological Basis **Key Point:** Gastroschisis arises from **mesoderm** (specifically the somatopleure — the fusion of somatic mesoderm and ectoderm). The anterior abdominal wall is derived from: - **Ectoderm:** skin and fascia - **Mesoderm:** muscle layers and peritoneum Failure of lateral body fold fusion → defect in mesodermal and ectodermal layers → herniation of viscera. ## Management Algorithm ```mermaid flowchart TD A[Prenatal diagnosis of gastroschisis]:::outcome --> B{Associated anomalies?}:::decision B -->|Yes: cardiac, renal, CNS| C[Detailed fetal echo + karyotype]:::action B -->|No: isolated| D[Counsel parents on prognosis]:::action C --> E[Plan delivery at tertiary centre]:::action D --> E E --> F[Vaginal delivery preferred if uncomplicated]:::action F --> G[Neonatal surgical closure post-delivery]:::action ``` ## Rationale for Correct Answer **High-Yield:** Prenatal management of gastroschisis is **expectant and coordinated**, NOT emergent in utero intervention: 1. **Detailed fetal assessment** — rule out associated anomalies (present in ~10% of cases) 2. **Karyotyping** — gastroschisis has low chromosomal abnormality risk (~2–3%), but assessment is standard 3. **Parental counselling** — prognosis is generally good (>90% survival with primary closure) 4. **Delivery planning** — arrange delivery at a centre with: - Neonatal intensive care - Pediatric surgical expertise - Capacity for staged closure if needed **Clinical Pearl:** Gastroschisis does NOT require emergency cesarean delivery or in utero surgery. Vaginal delivery is safe and preferred. Neonatal closure (primary or staged with silo) is the standard of care. ## Why This Approach - Fetal surgery for gastroschisis is **not indicated** — the defect is not life-threatening in utero - Prognosis depends on **bowel integrity** (assess for atresia, perforation) and **associated anomalies** — hence the need for detailed imaging - Delivery timing and mode are optimized **postnatally** based on neonatal condition 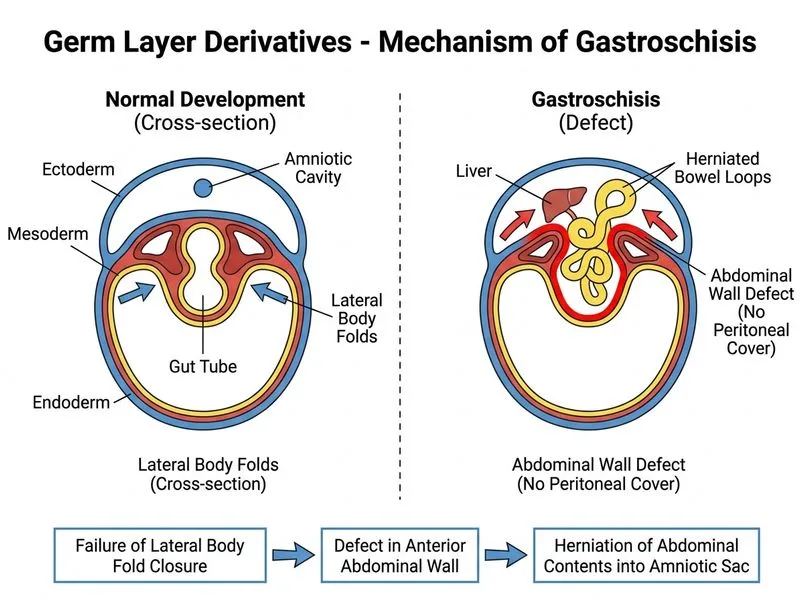
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.