## Clinical Scenario Analysis The described lesion is a **simple sacral dimple** — a common benign finding in newborns. The presence of a hair tuft is a minor risk factor but does not mandate intervention in the absence of imaging or clinical evidence of spinal dysraphism. ## Embryological Basis **Key Point:** Sacral dimples arise from incomplete fusion of the **ectoderm** during primary neurulation (weeks 3–4 of gestation). The neural tube is derived from **ectoderm** (specifically the neuroectoderm), and its incomplete closure or tethering of remnant tissue can result in: - **Tethered spinal cord** (mesodermal and ectodermal involvement) - **Dermal sinus tract** (ectodermal invagination) - **Simple dimple** (benign ectodermal depression) ## Risk Stratification | Feature | Risk of Spinal Dysraphism | |---------|---------------------------| | Dimple alone, no hair | ~1% | | Dimple + hair tuft | ~5–10% | | Dimple + skin changes (hemangioma, lipoma) | ~30–50% | | Dimple > 5 mm diameter, deep location | Higher risk | | Normal ultrasound imaging | Very low risk | **Mnemonic: SADDLE** — Signs Alerting to Dysraphism in Dimple Lesions: - **S**kin changes (hemangioma, lipoma, pigmentation) - **A**bnormal ultrasound findings - **D**eep dimple (>5 mm) - **D**ischarge or infection - **L**ower sacral location - **E**vidence of tethering on imaging ## Management Algorithm ```mermaid flowchart TD A[Sacral dimple identified]:::outcome --> B{Ultrasound findings normal?}:::decision B -->|Yes| C{High-risk features present?}:::decision B -->|No: tethering/sinus/syrinx| D[MRI + neurosurgery referral]:::action C -->|No| E[Clinical observation only]:::action C -->|Yes: skin changes, deep dimple| F[MRI for further assessment]:::action E --> G[Review at routine follow-up]:::action F --> H{Dysraphism confirmed?}:::decision H -->|Yes| I[Surgical intervention]:::action H -->|No| J[Discharge with reassurance]:::action ``` ## Rationale for Correct Answer **High-Yield:** In this case: - Ultrasound is **normal** (no tethering, syrinx, or sinus tract) - Dimple + hair tuft = **low-to-intermediate risk** but **not high-risk** - **Clinical observation** is the standard of care; MRI is reserved for: - Abnormal ultrasound findings - High-risk clinical features (skin changes, deep dimple, progressive neurological signs) - Parental anxiety with imaging abnormalities **Clinical Pearl:** A normal ultrasound in a newborn with a simple sacral dimple has a **negative predictive value >99%** for clinically significant spinal dysraphism. Prophylactic MRI and surgery are not indicated and increase cost and unnecessary anxiety. ## Why This Approach - **Expectant management** reduces unnecessary imaging and intervention - **Clinical vigilance** for progressive neurological signs (weakness, incontinence, asymmetric reflexes) is key - **Reassurance** to parents is important; most simple dimples are benign - **MRI is reserved** for imaging abnormalities or high-risk features 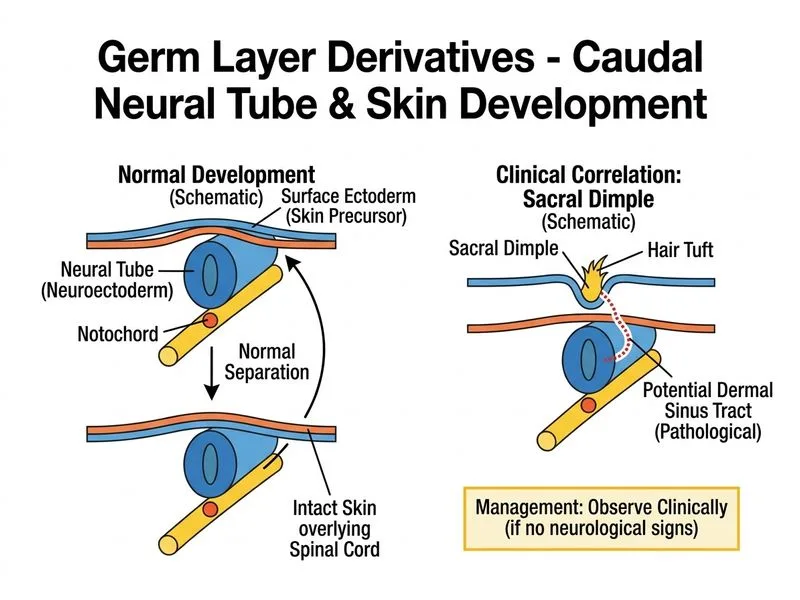
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.