## Diagnosis: Persistent Gestational Trophoblastic Neoplasia (PGTN) — Invasive Mole ### Clinical Scenario Analysis **Key Point:** Post-evacuation β-hCG that has not normalized by 6 weeks (18,000 mIU/mL from 280,000 at evacuation) with imaging evidence of a myometrial mass with increased vascularity = **invasive mole / PGTN** requiring staging and chemotherapy. ### FIGO Criteria for Diagnosing PGTN After Complete Mole - β-hCG plateau (±10%) over 4 consecutive weekly values over 3 weeks - β-hCG rise (>10%) over 3 consecutive weekly values over 2 weeks - β-hCG remains elevated at 6 months post-evacuation - Histological diagnosis of choriocarcinoma or invasive mole This patient meets criteria: persistent elevation with myometrial mass at 6 weeks. ### Why Pelvic MRI for Staging FIRST? Per FIGO 2000 guidelines and standard GTN management protocols (Seckl et al., Lancet Oncology; Berkowitz & Goldstein, NEJM): 1. **Staging is mandatory before chemotherapy** — the FIGO/WHO scoring system determines whether the patient receives single-agent or multi-agent chemotherapy. Incorrect risk stratification leads to under- or over-treatment. 2. **Pelvic MRI** is the gold standard for assessing depth of myometrial invasion, parametrial involvement, and local extent of disease — ultrasound alone is insufficient for complete staging. 3. **Staging workup** includes: pelvic MRI (or ultrasound), CXR (and CT chest if CXR positive), serum β-hCG, LFTs, RFTs, CBC. 4. Only after staging is the FIGO score calculated → Low risk (score ≤6): single-agent MTX or ActD; High risk (score ≥7): multi-agent EMA-CO. ### FIGO/WHO Scoring System (Abbreviated) | Factor | 0 | 1 | 2 | 4 | |--------|---|---|---|---| | Age | <40 | ≥40 | — | — | | Antecedent pregnancy | Mole | Abortion | Term | — | | Interval (months) | <4 | 4–6 | 7–12 | >12 | | Pre-treatment β-hCG | <1,000 | 1,000–10,000 | 10,000–100,000 | >100,000 | | Largest tumor (cm) | <3 | 3–4 | ≥5 | — | | Site of metastases | Lung | Spleen/kidney | GI | Brain/liver | | Number of metastases | 0 | 1–4 | 5–8 | >8 | | Prior chemotherapy | — | — | Single agent | ≥2 agents | **This patient's preliminary score:** Age <40 (0) + mole (0) + interval <4 months (0) + β-hCG 10,000–100,000 (2) + tumor <3 cm (0) + no metastases (0) = **Score ~2 → Low risk**, but this MUST be confirmed after full staging. ### Why NOT the Other Options - **Expectant management (B):** Contraindicated — PGTN with myometrial invasion will not resolve spontaneously; β-hCG will plateau or rise further. Expectancy is never appropriate once PGTN criteria are met. - **Repeat curettage + chemotherapy (C):** Repeat curettage is **NOT recommended** in PGTN with myometrial invasion — it carries risk of uterine perforation, haemorrhage, and dissemination. FIGO guidelines do not recommend routine repeat curettage for PGTN; chemotherapy alone is the standard. Curettage may be considered only in selected cases of non-invasive disease. - **Hysterectomy (D):** Not first-line. Reserved for women who have completed childbearing, have failed chemotherapy, or have life-threatening haemorrhage. Chemotherapy achieves >95% cure even with myometrial invasion. **Clinical Pearl (Harrison's Principles, 21st ed.):** In GTN, staging and risk stratification MUST precede chemotherapy selection. Pelvic MRI is the preferred imaging modality for local disease assessment. The sequence is: confirm PGTN → stage (MRI + CXR ± CT) → calculate FIGO score → initiate appropriate chemotherapy. **High-Yield:** Repeat curettage is NOT standard of care for invasive mole/PGTN — this is a common exam trap. Chemotherapy (after staging) is the definitive treatment. 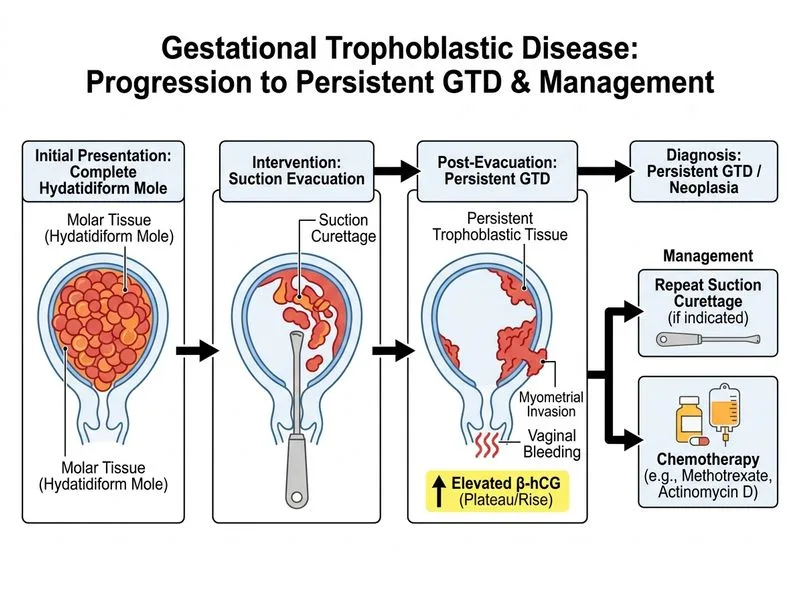
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.