## Management of Giant Cell Tumor of Bone ### Diagnosis Confirmation **Key Point:** The clinical presentation (epiphyseal/metaphyseal location at knee in young adult), imaging (eccentric lytic lesion extending to subarticular cortex), and cytology (multinucleated giant cells) are pathognomonic for giant cell tumor (GCT) of bone. ### Treatment Algorithm ```mermaid flowchart TD A[GCT of bone diagnosed]:::outcome --> B{Grade/Aggressiveness?}:::decision B -->|Low-grade, contained| C[Intralesional curettage + adjuvant]:::action B -->|High-grade or recurrent| D[Wide excision]:::action C --> E[Bone cement or allograft fill]:::action C --> F[Monitor for recurrence]:::outcome D --> G[Reconstruction if needed]:::action E --> H[Follow-up imaging at 3-6 months]:::outcome ``` ### Rationale for Intralesional Curettage **High-Yield:** Intralesional curettage with adjuvant (bone cement, allograft, or phenol) is the **gold standard first-line treatment** for most GCTs because: 1. **Preserves bone stock** — especially important in young patients and around the knee joint 2. **Maintains joint function** — avoids morbidity of wide excision and reconstruction 3. **Adequate local control** — recurrence rate is 10–15% with adjuvant, acceptable for a benign tumor 4. **Allows repeat surgery** — if recurrence occurs, wide excision can still be performed ### Adjuvant Options After Curettage | Adjuvant | Mechanism | Advantage | Disadvantage | |----------|-----------|-----------|---------------| | Bone cement (PMMA) | Thermal necrosis + mechanical fill | Radiopaque, easy to monitor | Exothermic reaction risk | | Allograft | Biologic fill, osteoconductive | Lower recurrence than cement alone | Slower incorporation | | Phenol | Chemical cauterization | Reduces recurrence | Toxicity if systemic absorption | | Cryotherapy | Liquid nitrogen freezing | Effective adjuvant | Risk of pathologic fracture | **Clinical Pearl:** The combination of curettage + adjuvant (especially allograft or cement) reduces recurrence from ~50% (curettage alone) to 10–15%. ### Why Wide Excision Is NOT First-Line Here **Warning:** Wide excision (option B) is reserved for: - Recurrent GCT after failed intralesional treatment - High-grade/aggressive lesions with cortical breakthrough - Pathologic fracture - Lesions in expendable bones (fibula, distal radius) For a primary, contained distal femoral GCT in a young woman, wide excision causes unnecessary loss of bone stock and joint dysfunction. ### Chemotherapy Is NOT Indicated **Key Point:** GCT is a **benign tumor** — chemotherapy (option C) has no role. Chemotherapy is used only for malignant bone tumors (osteosarcoma, Ewing sarcoma, chondrosarcoma). ### Follow-Up Protocol **High-Yield:** After curettage + adjuvant: - Plain radiographs at 3–6 weeks (assess fill, alignment) - MRI or CT at 3–6 months (detect early recurrence) - Clinical follow-up for minimum 2 years (peak recurrence window) - Recurrence presents as progressive pain, swelling, or radiolucency at the surgical site [cite:Rockwood and Green's Fractures in Adults Ch 38] 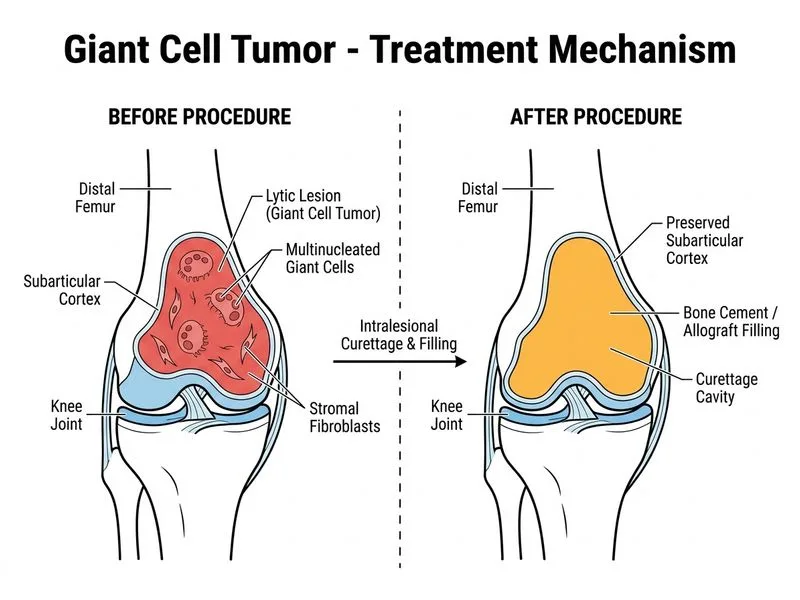
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.