## Management of Recurrent Giant Cell Tumor ### Clinical Context **Key Point:** This patient has **recurrent GCT** — a failed intralesional treatment. Recurrence occurs in 10–50% of cases depending on the initial adjuvant used; allograft alone has higher recurrence than cement or cryotherapy. ### Treatment Algorithm for Recurrent GCT ```mermaid flowchart TD A[Recurrent GCT confirmed]:::outcome --> B{Location & Aggressiveness?}:::decision B -->|Expendable bone| C[Wide excision]:::action B -->|Non-expendable, contained| D[Repeat curettage + aggressive adjuvant]:::decision B -->|Non-expendable, aggressive| E[Wide excision + reconstruction]:::action C --> F[Amputation if extensive]:::urgent D --> G[Phenol + cryotherapy]:::action E --> H[Fibular autograft or endoprosthesis]:::action G --> I[Monitor closely]:::outcome H --> J[Functional limb preservation]:::outcome ``` ### Why Wide Excision Is Now Indicated **High-Yield:** After failed intralesional treatment, **wide excision becomes the standard of care** because: 1. **Recurrence indicates aggressive biology** — the tumor has already demonstrated resistance to conservative management 2. **Risk of further recurrence is high** — repeat curettage has unacceptably high re-recurrence rates (up to 50–60%) 3. **Cortical thinning suggests structural compromise** — risk of pathologic fracture and joint instability 4. **Preservation of limb function** — wide excision with reconstruction (fibular autograft or endoprosthesis) maintains ambulation and function **Clinical Pearl:** The proximal tibia is a **non-expendable bone** (unlike fibula or distal radius). Therefore, amputation is avoided if reconstruction is feasible. ### Reconstruction Options After Wide Excision | Reconstruction Method | Indication | Advantage | Disadvantage | |----------------------|-----------|-----------|---------------| | **Fibular autograft** | Young patient, good bone stock | Biologic, incorporates, no rejection | Donor site morbidity, long incorporation | | **Endoprosthesis** | Elderly, poor health, rapid return to function | Immediate stability, no donor site | Loosening, revision needed, cost | | **Allograft + plate** | Moderate age, good vascularity | Biologic option, lower cost | Slower incorporation, infection risk | | **Distraction osteogenesis** | Metaphyseal defect, young patient | Biologic, regenerates bone | Prolonged treatment (3–6 months) | ### Why Repeat Curettage Is NOT Adequate **Warning:** Repeat intralesional curettage (option A) is **not recommended** for recurrent GCT because: - Re-recurrence rate is 50–60% (unacceptably high) - The tumor has already proven aggressive and resistant to conservative treatment - Each curettage weakens bone stock and increases fracture risk - Phenol + cryotherapy together are rarely used (phenol toxicity + cryonecrosis = excessive tissue damage) **Key Point:** The principle is: **"Once failed, treat with wide excision."** ### Denosumab: Emerging Role, Not First-Line Here **High-Yield:** Denosumab (anti-RANKL monoclonal antibody) is increasingly used for: - **Unresectable GCT** (sacral, pelvic tumors) - **Metastatic GCT** (rare, ~2% of cases) - **Neoadjuvant therapy** to reduce tumor vascularity and facilitate surgery However, denosumab is **NOT first-line for resectable recurrent GCT** in an extremity. The tumor is surgically accessible and wide excision offers definitive control. ### Amputation Is Last Resort **Urgent:** Amputation (option D) is reserved for: - Extensive soft-tissue involvement with neurovascular compromise - Failed reconstruction with severe functional impairment - Pathologic fracture with instability - Patient refusal of reconstruction In this case, wide excision with reconstruction is feasible and preferred. ### Follow-Up After Wide Excision **Clinical Pearl:** - Radiographs at 6 weeks, 3 months, 6 months, then annually - MRI at 6 months to assess graft incorporation - Clinical assessment for pain, swelling, functional status - Recurrence after wide excision is rare (<5%) [cite:Rockwood and Green's Fractures in Adults Ch 38; Orthopedic Surgery Principles and Practice 3e] 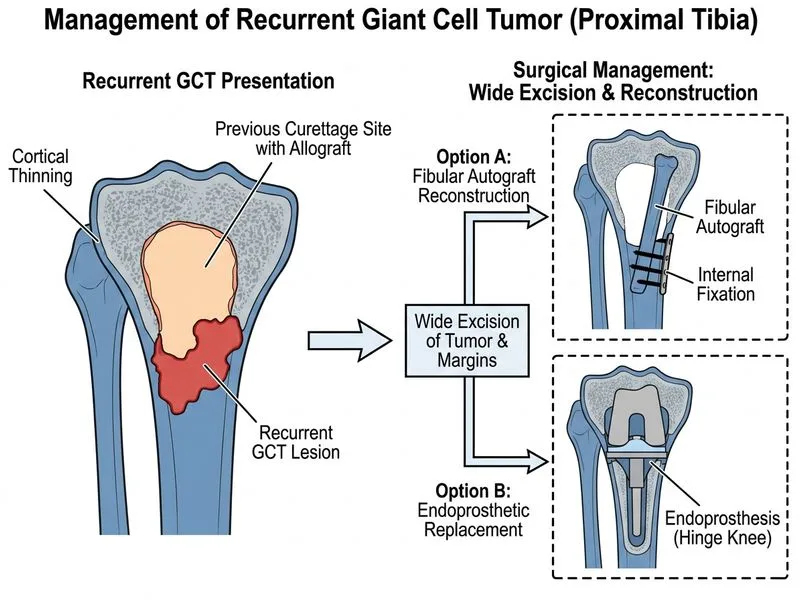
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.