## Clinical Context This patient has a **recurrent giant cell tumor** of the distal radius after initial intralesional curettage. Recurrence after first-line treatment significantly changes the management strategy. The lesion is locally aggressive (cortical erosion) and has failed conservative management. ## Recurrent GCT: Management Escalation **Key Point:** Recurrent GCT mandates **wide local excision** rather than repeat intralesional curettage because: 1. Recurrence indicates aggressive biology 2. Repeat intralesional curettage has a 50% re-recurrence rate 3. Wide excision reduces recurrence to <5% 4. Early aggressive management prevents further morbidity **High-Yield:** The distinction between **primary GCT** (intralesional curettage) and **recurrent GCT** (wide excision) is a high-yield NEET PG concept. This is a classic "best next step" scenario testing this escalation principle. ## Management Algorithm for GCT ```mermaid flowchart TD A[Giant Cell Tumor Diagnosed]:::outcome --> B{Primary or Recurrent?}:::decision B -->|Primary| C[Intralesional Curettage + Adjuvants]:::action C --> D{Healed?}:::decision D -->|Yes| E[Follow-up Imaging at 6, 12, 24 months]:::action D -->|No| F[Recurrence]:::outcome B -->|Recurrent| G[Wide Local Excision]:::action F --> G G --> H[Reconstruction: Fibular strut / Vascularized bone / Allograft]:::action H --> I[Adjuvant Denosumab if aggressive features]:::action ``` ## Reconstruction Options for Distal Radius | Method | Advantages | Disadvantages | |--------|-----------|---------------| | **Fibular strut graft** | Non-vascularized, simpler, adequate for distal radius | Slower incorporation, risk of non-union | | **Vascularized fibular graft** | Superior healing, lower non-union risk | Technically demanding, longer operative time | | **Allograft** | No donor site morbidity | Risk of disease transmission, slower incorporation | | **Reconstruction plate + cancellous graft** | Provides stability | Inadequate for large defects | **Clinical Pearl:** In the distal radius, a fibular strut graft is often sufficient for reconstruction after wide excision of recurrent GCT, especially if the lesion does not involve the entire bone width. Vascularized transfer is reserved for massive defects or multiple recurrences. ## Role of Denosumab in Recurrent GCT **Key Point:** Denosumab (RANKL inhibitor) is an **adjuvant** option, not primary therapy: - May be used **before** wide excision to reduce tumor vascularity and facilitate surgery - May be used **after** wide excision in aggressive or multiply recurrent cases - Does NOT replace surgical management - Typical dosing: 120 mg SC weekly × 4 weeks, then monthly **Warning:** Denosumab alone without surgery is inadequate for recurrent GCT. It is a neoadjuvant or adjuvant tool, not definitive treatment. 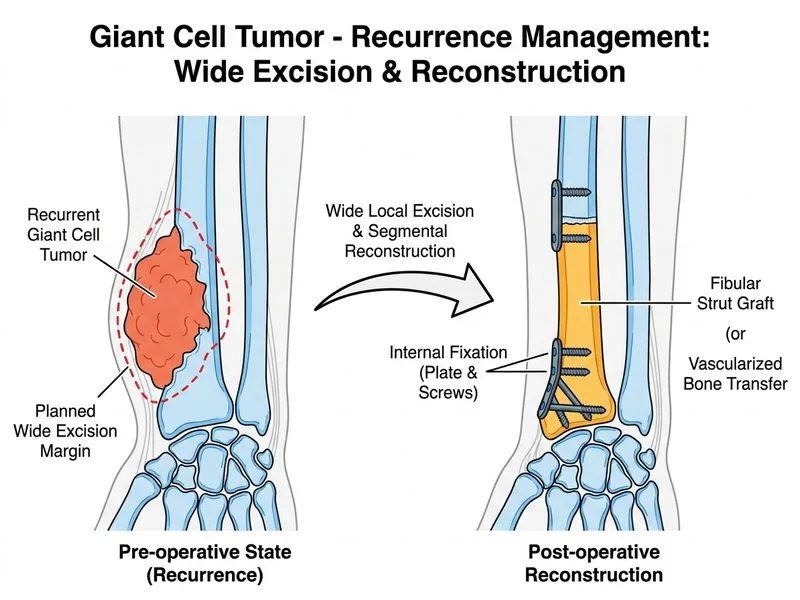
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.