## Distinguishing Gonorrhea from Chlamydia: Gram Stain Appearance ### Key Microbiological Difference **Key Point:** The presence of **intracellular gram-negative diplococci on Gram stain** is the single best distinguishing feature of *Neisseria gonorrhoeae* from *Chlamydia trachomatis*. Chlamydia is an obligate intracellular bacterium that is **not visible on Gram stain** — it cannot be detected by this method at all, making the Gram stain finding pathognomonic for gonorrhea in the right clinical context. ### Comparative Table: Gonorrhea vs. Chlamydia | Feature | *N. gonorrhoeae* | *C. trachomatis* | | --- | --- | --- | | **Gram stain appearance** | Gram-negative diplococci within PMNs (intracellular) | **Not visible on Gram stain** (obligate intracellular; too small) | | **Culture media** | Thayer-Martin, MTM (selective enriched agar) | Cannot be cultured on standard agar; requires cell culture or NAATs | | **Oxidase test** | Positive | Not applicable | | **First-line treatment** | Ceftriaxone IM | Azithromycin or doxycycline | | **Acute vs. chronic PID** | Acute urethritis/cervicitis | Chronic/recurrent PID; higher risk of tubal damage | ### Why Option C is the Best Distinguishing Feature **High-Yield:** The question asks what **best distinguishes** gonorrhea from Chlamydia in genital infection. The Gram stain showing intracellular gram-negative diplococci is **unique to gonorrhea** — Chlamydia produces no such finding. This is the most direct, clinically immediate discriminator used at the bedside. **Clinical Pearl:** A positive Gram stain (intracellular gram-negative diplococci in PMNs) has ~95% specificity for gonorrhea in symptomatic men. Chlamydia is invisible on Gram stain and requires NAAT for diagnosis. This is the classic teaching point in every STI chapter. ### Why the Other Options Are Incorrect - **Option A — Ability to grow on standard bacterial culture media:** This is a **factual error** as a distinguishing feature. *N. gonorrhoeae* is **fastidious** and does NOT grow on standard (e.g., blood agar alone without enrichment); it requires **selective enriched media** (Thayer-Martin). The distinction is that Chlamydia cannot be cultured on any agar at all, but framing gonorrhea as growing on "standard" media is misleading and not the best discriminator. - **Option B — Tetracycline as first-line treatment:** Tetracycline/doxycycline is used for Chlamydia, not gonorrhea (treated with ceftriaxone). This is a treatment difference, not a diagnostic distinguishing feature. - **Option D — Association with chronic PID:** Both organisms can cause PID. Chlamydia is more associated with chronic/recurrent PID, but this is a clinical outcome tendency, not a direct discriminating microbiological feature. [cite: Harrison's Principles of Internal Medicine, 21e, Ch 137; Jawetz Medical Microbiology, 28e] 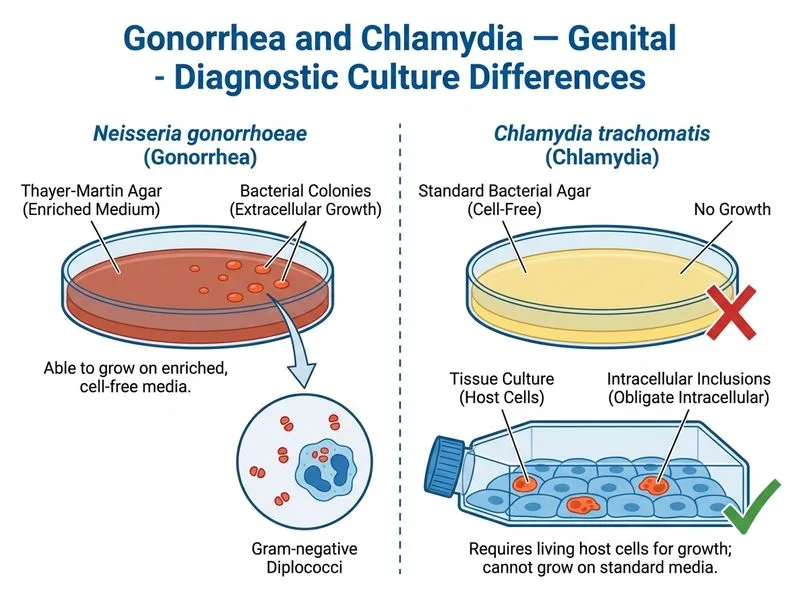
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.