## Dual Therapy for Presumed Gonococcal and Chlamydial Infection ### Clinical Presentation Analysis **Key Point:** Mucopurulent cervical discharge, cervical friability, and lower abdominal pain suggest cervicitis with possible pelvic inflammatory disease (PID). The absence of gram-negative diplococci on Gram stain does NOT exclude gonorrhea, as cervical Gram stain has low sensitivity (~50%) for *N. gonorrhoeae*. **High-Yield:** Gonorrhea and chlamydia frequently coexist (25–50% of cases). Treating only one pathogen leaves the patient at risk for treatment failure and complications. ### Why Gram Stain Negativity Does Not Exclude Gonorrhea | Feature | Urethral Smear | Cervical Smear | |---------|---|---| | Sensitivity for GC | ~95% | ~50% | | Specificity | ~99% | ~99% | | Reliability | High in males | Low in females | Cervical Gram stain is unreliable because: - Normal flora obscure gonococci - Specimen collection technique varies - Intracellular location makes visualization difficult ### Current Management Guideline **Clinical Pearl:** In women with suspected cervicitis or PID, empiric dual therapy is standard of care: 1. **Ceftriaxone 250 mg IM** (single dose) — covers gonorrhea, including resistant strains 2. **Azithromycin 1 g PO** (single dose) — covers chlamydia and atypical organisms This combination covers both pathogens and provides broader coverage for PID (which may involve anaerobes and gram-positive cocci). ### Why Not Monotherapy? - Azithromycin alone: Misses gonorrhea in ~10–15% of cases; also emerging resistance - Ceftriaxone alone: Misses chlamydia in ~30–40% of cases - Awaiting NAAT: Delays treatment in symptomatic PID; risks progression to tubo-ovarian abscess or infertility **Warning:** Do not withhold treatment pending culture or NAAT results in symptomatic women with signs of PID. Empiric dual therapy is the standard of care. 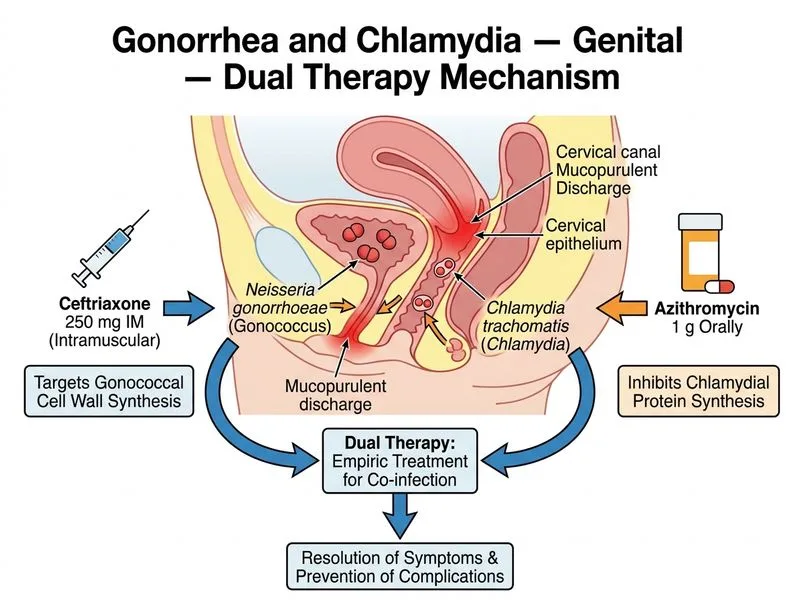
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.