## Diagnosis and Pathophysiology **Key Point:** This is a classic presentation of Guillain-Barré Syndrome (GBS) with ascending flaccid paralysis, areflexia, and albuminocytologic dissociation (elevated CSF protein with normal cell count). **High-Yield:** The preceding diarrheal illness (likely *Campylobacter jejuni*) is a well-recognized trigger for GBS in India and globally. The demyelinating pattern on NCS (prolonged distal latencies, conduction blocks) confirms the diagnosis. ## Immediate Management Principles **Clinical Pearl:** GBS is an autoimmune-mediated demyelinating neuropathy with potential for rapid respiratory compromise. The presence of mild facial weakness and tachycardia with ectopy suggests early bulbar and autonomic involvement — this patient requires ICU-level monitoring. **Mnemonic: IVIG vs Plasma Exchange (PE) — BOTH WORK EQUALLY:** - **I**ntravenous **I**mmunoglobulin — easier to administer, fewer complications, preferred in resource-limited settings - **P**lasma **E**xchange — equally effective, requires vascular access and anticoagulation ## Evidence-Based Treatment | Intervention | Onset | Duration | Contraindications | First-line in India | |---|---|---|---|---| | IVIG 2 g/kg | 24–48 hrs | 3–5 days | IgA deficiency, thrombosis risk | **Yes** | | Plasma exchange | 24–48 hrs | 5 days | Hemodynamic instability, sepsis | Alternative | | Corticosteroids | Slow | Variable | No proven benefit in GBS | **No** | | Supportive care alone | N/A | N/A | Inadequate for moderate–severe GBS | Adjunctive only | **Key Point:** Both IVIG and plasma exchange are Class I recommendations by the American Academy of Neurology. IVIG is preferred in this case because: 1. Easier vascular access in a rural setting 2. No need for anticoagulation 3. Lower risk of hemodynamic fluctuation (important given his cardiac ectopy) 4. Faster mobilization of therapy **Warning:** Corticosteroids alone are **ineffective** in GBS and may delay recovery; they are not recommended as monotherapy. ## Supportive Measures (Concurrent) 1. **Respiratory monitoring:** FVC, NIF every 6–8 hours; intubate if FVC < 15 mL/kg or NIF < 30 cm H₂O 2. **Autonomic support:** Continuous cardiac monitoring (risk of arrhythmia, labile BP) 3. **DVT prophylaxis:** Sequential compression devices ± anticoagulation 4. **Nutritional support:** Early enteral feeding if bulbar involvement 5. **Pain management:** Neuropathic pain is common; gabapentin or pregabalin **High-Yield:** This patient's tachycardia and ectopy warrant ICU admission for hemodynamic and respiratory surveillance even before immunotherapy. 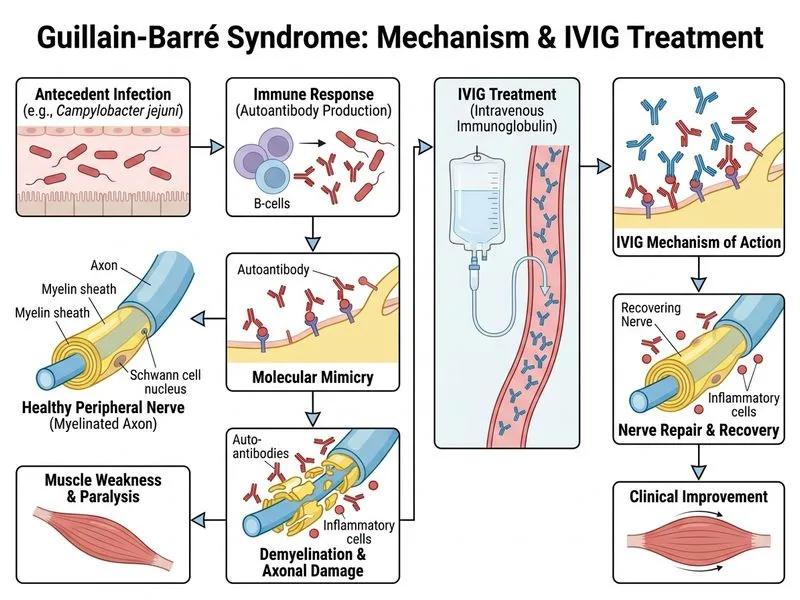
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.