## CSF Findings and Timing in GBS **Key Point:** Cerebrospinal fluid analysis in GBS shows **albuminocytologic dissociation** — markedly elevated protein (typically 100–500 mg/dL, sometimes >1000 mg/dL) with **normal or minimally elevated cell count** (<50 WBC/µL, usually <10). This finding is most prominent after the first week of illness. ### Timing of LP and CSF Evolution **High-Yield:** The classic CSF pattern in GBS develops over time: - **Days 1–3 (early illness):** CSF may be completely normal or show only mild protein elevation - **Days 4–7 (peak):** Albuminocytologic dissociation becomes evident - **Days 7–14 onwards:** Protein peaks and remains elevated; cell count stays normal **Clinical Pearl:** If LP is performed in the first 3 days and CSF is normal, do NOT exclude GBS. Repeat LP after 1 week may show the characteristic pattern. The diagnosis should not be delayed waiting for CSF confirmation when clinical features and NCS/EMG are suggestive. ### Albuminocytologic Dissociation Explained This unique CSF pattern reflects: - **Elevated protein:** Breakdown of blood–brain barrier and increased vascular permeability at nerve roots and spinal cord - **Normal cell count:** Minimal inflammatory cell infiltration (demyelination is the primary pathology, not primary inflammation) **Mnemonic:** **GBS-CSF = HIGH protein, LOW cells** — **H**igh albumin, **I**ncreased protein, **G**BS hallmark, **L**ow WBC, **O**ver 1 week, **W**hy: demyelination not inflammation. ### Differential CSF Patterns | Condition | Protein | WBC | Glucose | Distinguishing Feature | |---|---|---|---|---| | **GBS (classic)** | ↑↑ (100–500+) | Normal/↑ (<50) | Normal | Albuminocytologic dissociation | | **Bacterial meningitis** | ↑ (100–500) | ↑↑ (>100, PMN) | ↓ | Low glucose, PMN predominance | | **Viral meningitis** | ↑ (50–200) | ↑ (10–500, lymph) | Normal | Lymphocytic pleocytosis | | **TB meningitis** | ↑↑ (100–500) | ↑ (50–500, lymph) | ↓ | Low glucose, chronic course | | **Spinal cord compression** | ↑↑ | Normal/↑ (<50) | Normal | MRI shows mass; no ascending paralysis | **Warning:** A CSF with pleocytosis (>50 WBC/µL) should prompt reconsideration of the diagnosis — consider viral meningitis, Lyme disease, or other inflammatory neuropathies. [cite:Harrison 21e Ch 446; Robbins 10e Ch 28] 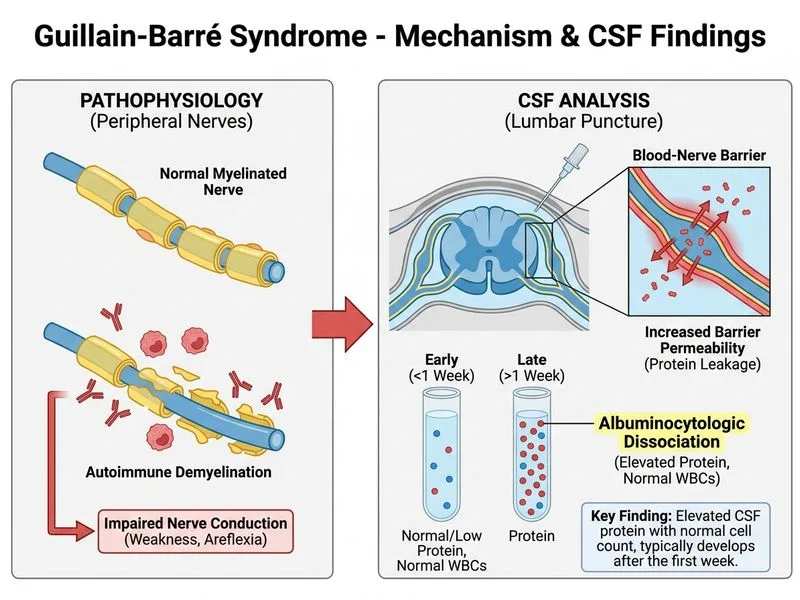
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.