## PaCO₂ Management in Severe Head Injury **Key Point:** Target PaCO₂ is 40–45 mmHg in severe head injury. Aggressive hyperventilation (PaCO₂ < 30 mmHg) is no longer recommended as a routine strategy and may worsen outcomes by reducing cerebral blood flow. ### Pathophysiology of CO₂ and Cerebral Perfusion 1. CO₂ is a potent cerebral vasodilator 2. Hyperventilation lowers PaCO₂ → cerebral vasoconstriction → reduced intracranial blood volume → decreased ICP 3. However, prolonged vasoconstriction reduces cerebral perfusion pressure and worsens ischemia 4. Current evidence supports normocapnia (40–45 mmHg) as the safe target **High-Yield:** Aggressive hyperventilation (PaCO₂ < 30 mmHg) is now reserved **only** for acute ICP crisis (herniation signs) as a **temporary bridge** to definitive intervention (surgery, osmotic therapy). It should not be used prophylactically. **Clinical Pearl:** Hypercapnia (PaCO₂ > 45 mmHg) increases ICP and is harmful; hypocapnia (< 30 mmHg) reduces cerebral perfusion. The "sweet spot" is normocapnia. **Mnemonic:** **40–45 is GREAT** — maintain normal CO₂ levels; save aggressive hyperventilation for **CRISIS** (herniation only). ### Evolution of Guidelines | Era | Recommendation | Rationale | | --- | --- | --- | | 1980s–1990s | Aggressive hyperventilation (PaCO₂ 25–30) | Rapid ICP reduction | | 2000s onwards | Normocapnia (40–45 mmHg) | Avoids secondary ischemia | | Current (ATLS/BTF) | 40–45 routine; < 30 only for acute herniation | Evidence-based neuroprotection | 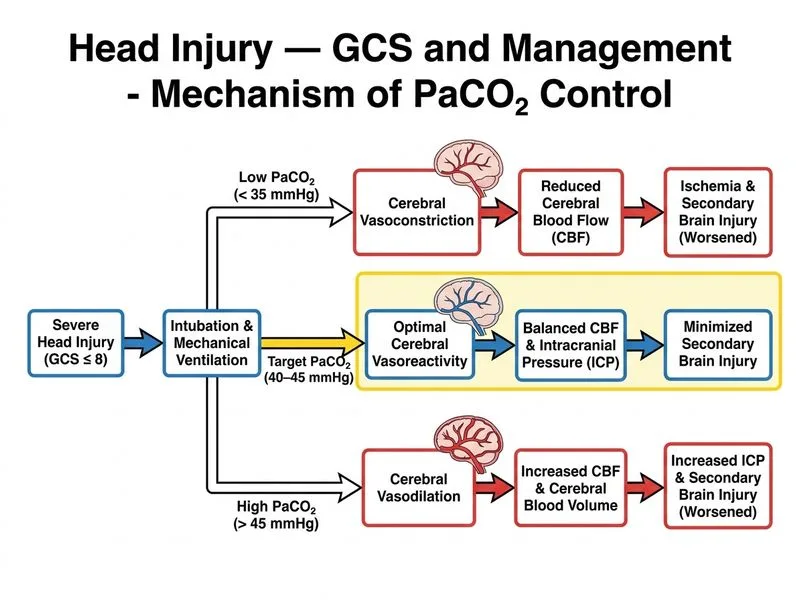
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.