## Clinical Assessment **Key Point:** This patient's GCS = E2 + V2 + M5 = **GCS 9** (not 7 as previously stated — V2 = incomprehensible sounds scores 2, M5 = localizes to pain scores 5, E2 = opens to pain scores 2; total = 9). This classifies him as having a **moderate traumatic brain injury** (GCS 9–12). The CT findings show a **thin acute subdural hematoma (3 mm) with minimal midline shift (2 mm) and no brainstem herniation signs**. > **Note on CSF rhinorrhea:** The presence of CSF rhinorrhea indicates a basilar skull fracture. While this is an important finding requiring follow-up (and prophylactic antibiotics are controversial), it does **not** change the acute SDH management algorithm — the decision to operate is still driven by hematoma thickness, midline shift, and clinical trajectory. ## Management Principles for Acute SDH | Feature | Thin SDH (<10 mm, <5 mm shift) | Thick SDH (≥10 mm or ≥5 mm shift) | |---------|--------------------------------|-----------------------------------| | **Indication for surgery** | Not automatically indicated | Surgical evacuation indicated | | **Monitoring** | Serial neuro exams, repeat imaging | Immediate neurosurgery | | **Osmotic therapy** | Reserved for deterioration/herniation signs | May be used as bridge to OR | **High-Yield (Greenberg / Bullock EBIC Guidelines):** The decision to operate on acute SDH is based on **thickness ≥ 10 mm OR midline shift ≥ 5 mm**, regardless of GCS. A thin SDH (3 mm) with minimal shift (2 mm) does **not** meet surgical criteria. Conservative ICU management with serial neurological exams and repeat CT is the standard of care. ## Why Option A is Correct 1. **GCS 9 (moderate TBI)** warrants ICU admission with continuous neuro monitoring 2. **Thin SDH (3 mm) + minimal shift (2 mm)** does not meet Bullock criteria for surgical evacuation (≥10 mm thickness or ≥5 mm shift) 3. **No herniation signs** — pupils equal and reactive, no Cushing's triad 4. **Serial CT at 24 hours** detects any hematoma expansion early; neurosurgery on standby ensures rapid response if deterioration occurs 5. **Mannitol (Option C)** is reserved for signs of raised ICP or impending herniation — not used prophylactically in a hemodynamically stable patient without herniation signs ## Why the Other Options Are Wrong - **Option B (Dexamethasone):** Corticosteroids are **contraindicated** in traumatic brain injury (CRASH trial demonstrated increased mortality). This is a hard rule in TBI management. - **Option C (Mannitol + urgent evacuation):** Mannitol is not indicated without signs of herniation or ICP crisis. Urgent evacuation is not indicated for a 3 mm SDH with 2 mm shift. The verifier's GCS calculation (9) is correct, but GCS alone does not mandate surgery — mass effect criteria must also be met. - **Option D (Bedside burr hole without CT):** Absolutely contraindicated. CT confirmation is mandatory before any surgical intervention; bedside burr holes without imaging guidance are dangerous and not standard of care. ## Clinical Pearl **Warning:** Do not confuse GCS severity with surgical indication. The **Bullock criteria** for acute SDH surgery are: thickness ≥ 10 mm OR midline shift ≥ 5 mm (regardless of GCS), OR GCS drop ≥ 2 points from injury to hospital arrival. This patient meets none of these criteria. **Mnemonic:** **MASS** — **M**idline shift ≥5 mm, **A**cute SDH thickness ≥10 mm, **S**urgical criteria met → operate; **S**igns of herniation → also operate. *References: Bullock MR et al., Neurosurgery 2006 (Guidelines for Surgical Management of TBI); CRASH Trial Collaborators, Lancet 2004; Greenberg MS, Handbook of Neurosurgery, 9th ed.* 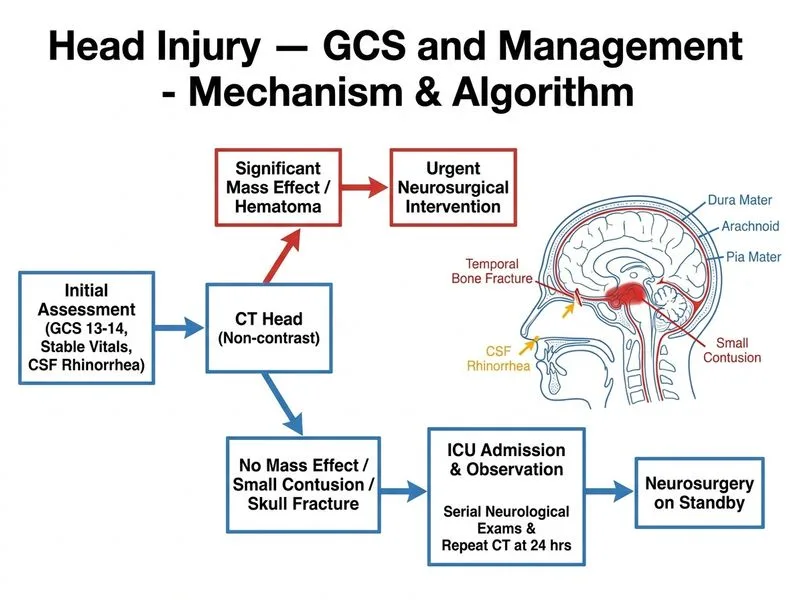
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.