## Acute vs. Chronic Subdural Hematoma: Key Discriminators ### Temporal Evolution and Imaging **Key Point:** The presence of an organizing membrane (neomembrane) and mixed-density fluid on CT is the hallmark of chronic subdural hematoma. This reflects the healing process over 2–3 weeks, during which the hematoma undergoes liquefaction and is surrounded by a fibrovascular membrane. Acute subdural hematoma shows homogeneous hyperdensity without membrane formation. ### Comparative Table | Feature | Acute SDH | Chronic SDH | |---------|-----------|-------------| | **Timing** | 0–3 days | >3 weeks (usually 2–4 weeks) | | **CT density** | Homogeneous hyperdense (bright) | Mixed density (hypodense + isodense) | | **Organizing membrane** | Absent | Present (neomembrane) | | **Fluid character** | Fresh blood | Liquefied, xanthochromic | | **Clinical onset** | Acute deterioration | Insidious (headache, confusion, gait disturbance) | | **Mechanism** | Usually severe trauma | Often trivial trauma (elderly, anticoagulated) | | **Associated brain injury** | Significant (contusion, DAI) | Minimal underlying brain injury | | **Mortality** | 30–60% | <5% if treated | ### Pathophysiology of Chronic SDH 1. **Week 1:** Hematoma is hyperdense (fresh blood); clot begins to organize at periphery. 2. **Week 2–3:** Neomembrane forms around the collection; internal fibrinolysis begins; fluid becomes mixed-density. 3. **Week 3+:** Membrane fully formed; fluid becomes hypodense (CSF-like); risk of rebleeding into the membrane. **High-Yield:** The **neomembrane is friable and highly vascularized** — it can rebleed spontaneously or with trivial trauma, causing recurrent subdural hematoma. This is why anticoagulation must be reversed or held carefully in chronic SDH. ### Clinical Pearl **Clinical Pearl:** Chronic subdural hematoma is common in elderly patients, chronic alcoholics, and those on anticoagulation. The initial trauma may be so trivial (a fall from standing) that the patient does not remember it. Presentation is insidious: progressive headache, cognitive decline, gait disturbance, and sometimes focal neurological deficits mimicking stroke or dementia. ### Why Other Options Are Not Discriminators - **Immediate loss of consciousness:** Acute SDH often causes immediate coma, but chronic SDH may present without any loss of consciousness — the patient may not even recall the initial injury. - **Midline shift:** Both acute and chronic SDH can cause midline shift depending on volume. This reflects severity, not chronicity. - **Emergency craniotomy:** Acute SDH requires emergency surgery; chronic SDH is usually managed conservatively unless symptomatic or enlarging, then burr holes (not full craniotomy) are preferred. 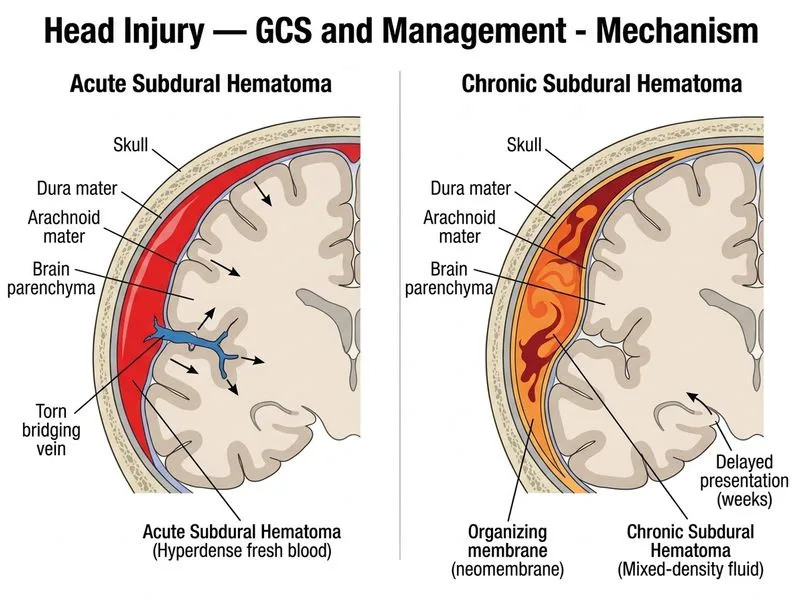
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.