## Acute Epidural Hematoma with Herniation — Airway Priority **Key Point:** A patient with GCS 7, a fixed dilated pupil (sign of uncal herniation), and respiratory depression is in **acute neurological emergency**. The FIRST priority is **airway protection** — not pharmacological management, not even neurosurgery — because without a secure airway, the patient will die from hypoxia before reaching the OR. **High-Yield:** In any head injury with GCS ≤ 8 or signs of herniation: 1. **Airway** (intubate immediately) 2. **Breathing** (ventilate, target normocapnia or mild hypocapnia) 3. **Circulation** (maintain MAP to perfuse brain) 4. **Neurosurgery** (definitive evacuation) ### Triage of Interventions in Herniation ```mermaid flowchart TD A[GCS ≤ 8 + Herniation signs]:::urgent --> B[Airway threatened?]:::decision B -->|Yes| C[Rapid Sequence Intubation]:::action B -->|No| D[Prepare for intubation]:::action C --> E[Secure airway + ventilate]:::action E --> F[Mannitol + hyperventilation<br/>as bridge to OR]:::action F --> G[Activate neurosurgery<br/>Immediate OR]:::action G --> H[Evacuation of hematoma]:::action H --> I[Neurological recovery]:::outcome ``` **Clinical Pearl:** The **fixed dilated pupil** (6 mm, non-reactive) on the LEFT indicates uncal herniation on that side — the ipsilateral uncus is herniating through the tentorial notch, compressing the oculomotor nerve (CN III). This is a **neurosurgical emergency**, but the patient cannot survive surgery without a patent airway. **Warning:** Do NOT attempt burr holes at the bedside in a non-intubated patient with GCS 7 and respiratory depression. The patient will aspirate and die. Burr holes are a **last resort** only if the patient is in a facility with no OR and no intubation capability — exceedingly rare in modern trauma centers. **Mnemonic: ABCs of Herniation** - **A**irway first (intubate if GCS ≤ 8) - **B**ridge therapy (mannitol, hyperventilation) - **C**all neurosurgery (simultaneous with A) - **S**urgery (evacuation in OR) ### Rapid Sequence Intubation Drugs in Head Injury | Drug | Dose | Advantage in Head Injury | Caution | |------|------|--------------------------|----------| | **Etomidate** | 0.2–0.3 mg/kg IV | Maintains cerebral perfusion pressure; minimal ICP rise | Avoid in sepsis; single dose only | | **Propofol** | 1–2 mg/kg IV | Decreases ICP | Hypotension risk; avoid in shock | | **Thiopental** | 3–5 mg/kg IV | Decreases ICP and cerebral metabolic rate | Hypotension; rarely used now | | **Rocuronium** | 1.2 mg/kg IV | Rapid onset; no histamine release | — | | **Succinylcholine** | 1–1.5 mg/kg IV | Rapid onset | May transiently raise ICP; use with caution | **Key Point:** Etomidate or propofol + rocuronium is the standard RSI combination in head injury. Succinylcholine is acceptable if rocuronium is unavailable, but the transient ICP rise is a minor concern compared to airway loss. [cite:ATLS 10th Edition, Chapter 4: Initial Assessment and Management; Neurocritical Care Society Guidelines on Traumatic Brain Injury] 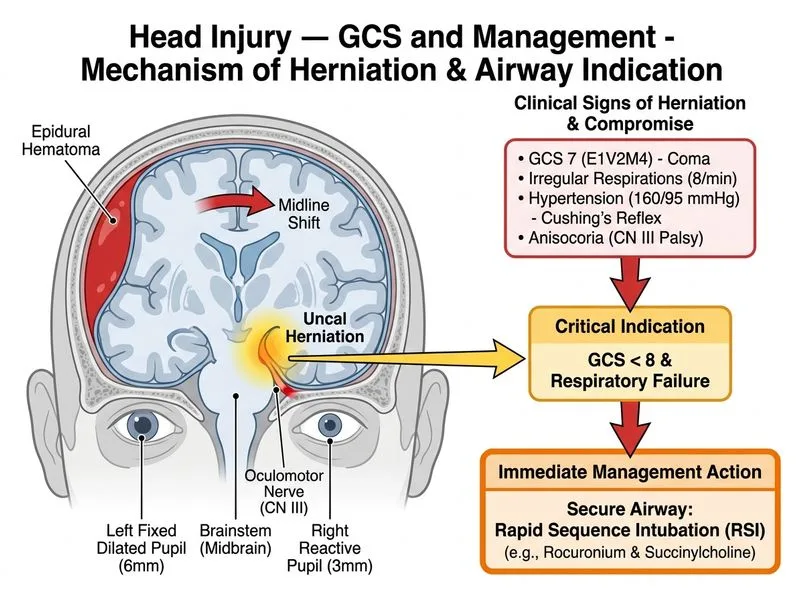
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.