## Clinical Context This patient has a small epidural hematoma (EDH) with preserved consciousness (GCS 15) and no mass effect. The key question is: does this patient need surgery or can she be managed conservatively? ## Key Point: **Epidural hematoma <30 mm without midline shift and GCS ≥13 can be managed conservatively with close neurological monitoring and serial imaging.** Surgery is reserved for hematomas >30 mm, midline shift, or GCS deterioration. ## Epidural vs Subdural Hematoma — Management Comparison | Feature | Epidural Hematoma | Acute Subdural Hematoma | | --- | --- | --- | | **Size threshold for surgery** | >30 mm OR midline shift | >10 mm OR GCS ≤12 | | **Consciousness at presentation** | Often preserved initially ("lucid interval") | Often altered (GCS ≤12) | | **Natural history** | Can stabilize or expand slowly | Tends to expand; higher mortality | | **Conservative management** | Possible if <30 mm, GCS ≥13, no shift | Rare; usually operative | | **Imaging follow-up** | Repeat CT at 24–48 hrs | Repeat CT if deterioration | ## Operative vs Conservative Management Algorithm ```mermaid flowchart TD A[EDH on CT]:::outcome --> B{Size >30 mm OR midline shift OR GCS <13?}:::decision B -->|Yes| C[Neurosurgical evacuation]:::action B -->|No| D[Conservative management]:::action D --> E[High-dependency/ICU admission]:::action E --> F[Hourly neuro checks × 24 hrs]:::action F --> G[Repeat CT at 24 hrs]:::action G --> H{Stable or shrinking?}:::decision H -->|Yes| I[Continue observation, discharge when stable]:::outcome H -->|No| J[Neurosurgical consultation for delayed evacuation]:::action C --> K[Postoperative ICU care]:::outcome ``` ## Rationale for Correct Answer **High-dependency unit admission with serial neurological examinations and repeat CT at 24 hours** is the standard of care because: 1. **Size criterion met**: 20 mm EDH is <30 mm (operative threshold). 2. **GCS preserved**: GCS 15 indicates no significant mass effect or herniation risk. 3. **No midline shift**: Imaging shows no mass effect. 4. **Conservative management is safe**: EDH in young patients with good GCS can be managed non-operatively if monitored closely. Approximately 50% of small EDH resolve without surgery. 5. **Serial monitoring essential**: Hourly neuro checks for 24 hours; repeat CT at 24 hours to confirm stability or detect expansion. 6. **Escalation pathway**: If patient deteriorates (GCS drop, new focal signs) or hematoma expands, proceed to surgery. ## High-Yield: **Small EDH (≤30 mm) + GCS ≥13 + no shift = observe with serial imaging.** Do NOT operate on every EDH; size and consciousness matter. Young patients tolerate small EDH well. ## Clinical Pearl: The "lucid interval" is classically associated with EDH — patient may be alert initially, then deteriorate as the hematoma expands. This patient is currently lucid; close monitoring will detect any deterioration early, allowing timely intervention. ## Warning: ~~Do not discharge home~~ — this patient requires admission for continuous monitoring. Epidural hematoma can expand rapidly, and outpatient follow-up is unsafe. 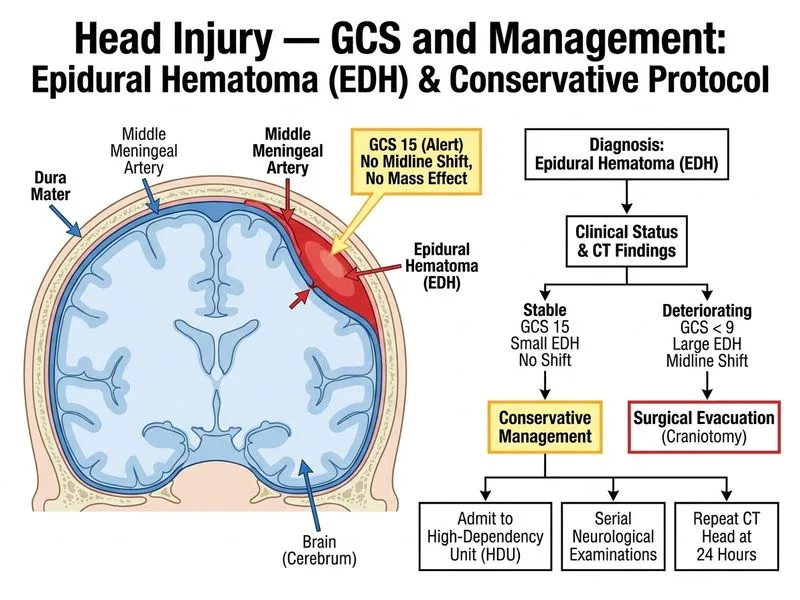
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.