## Embryological Pathogenesis of Tetralogy of Fallot (TOF) ### The Four Anatomical Components of TOF | Feature | Embryological Origin | Pathophysiology | |---------|----------------------|-----------------| | Ventricular Septal Defect (VSD) | Failure of conal septum to fuse with endocardial cushion septum | Allows right-to-left shunt | | Overriding Aorta | Anterior displacement of aorticopulmonary septum due to maldevelopment of conal region | Aorta straddles the VSD, receiving blood from both ventricles | | Right Ventricular Hypertrophy | Secondary to increased RV workload (RV must pump against pulmonary stenosis) | Develops postnatally | | Pulmonary Stenosis | Underdevelopment of the conus arteriosus and conal septum | Obstruction to RV outflow | ### The Neural Crest Cell Defect in TOF **Key Point:** TOF is a **conotruncal defect** caused by abnormal migration and proliferation of **neural crest cells** into the conus arteriosus and truncus arteriosus during weeks 4–6. ### Normal Conal Development 1. Neural crest cells migrate from the pharyngeal arches into the conus arteriosus. 2. These cells form the **conal septum** (also called the infundibular septum). 3. The conal septum grows **superiorly and anteriorly** to fuse with the **endocardial cushion septum** (which forms the membranous VSD). 4. This fusion divides the conus into two separate outflow tracts: the aortic outflow (from LV) and pulmonary outflow (from RV). 5. The conal septum also contributes to the wall of the pulmonary infundibulum. ### Pathogenesis in TOF When neural crest cell migration is **deficient or abnormal**: - The conal septum is **underdeveloped** (hypoplastic). - The conal septum **fails to fuse completely** with the endocardial cushion septum. - This results in: - **VSD**: The unfused portion of the conal septum leaves a defect in the ventricular septum. - **Overriding aorta**: The aorta, instead of arising solely from the left ventricle, is displaced anteriorly and straddles the VSD, receiving blood from both ventricles. - **Pulmonary stenosis**: The hypoplastic conal septum narrows the pulmonary infundibulum, causing obstruction to RV outflow. - **RV hypertrophy**: Develops secondary to increased RV pressure as it works against the stenotic pulmonary valve. **High-Yield:** TOF is the most common **cyanotic heart defect in children beyond the neonatal period**. The "four defects" are actually **three primary defects** (VSD, overriding aorta, pulmonary stenosis) with RV hypertrophy being a secondary consequence. ### Clinical Presentation in This Infant - **Cyanosis**: Deoxygenated blood from the right ventricle bypasses the stenotic pulmonary valve via the VSD and overriding aorta, entering the systemic circulation directly. - **Single loud S2**: The aortic valve closes normally, but the pulmonary valve closes late and softly due to pulmonary stenosis; thus, only the aortic component is heard. - **Systolic ejection murmur**: From the pulmonary stenosis (not the VSD, which is typically silent). ### Tet Spell (Hypercyanotic Spell) Infants with TOF may experience sudden episodes of severe cyanosis (Tet spells) caused by: - Increased right-to-left shunting through the VSD. - Triggered by crying, feeding, or defecation (increased systemic vascular resistance). - **Management**: Knee-chest position (increases systemic vascular resistance), oxygen, morphine, and beta-blockers. **Mnemonic:** **CONUS** = **C**onal septum defect → **O**verride → **N**ormal pulmonary valve but **U**nderdeveloped infundibulum → **S**eptal defect. (This is a memory aid for the embryological sequence, not a standard mnemonic.) **Clinical Pearl:** TOF is strongly associated with **22q11 deletion (DiGeorge syndrome)**, which affects neural crest cell development. Always screen for other features of DiGeorge (thymic hypoplasia, hypocalcemia, cleft palate, facial dysmorphism). 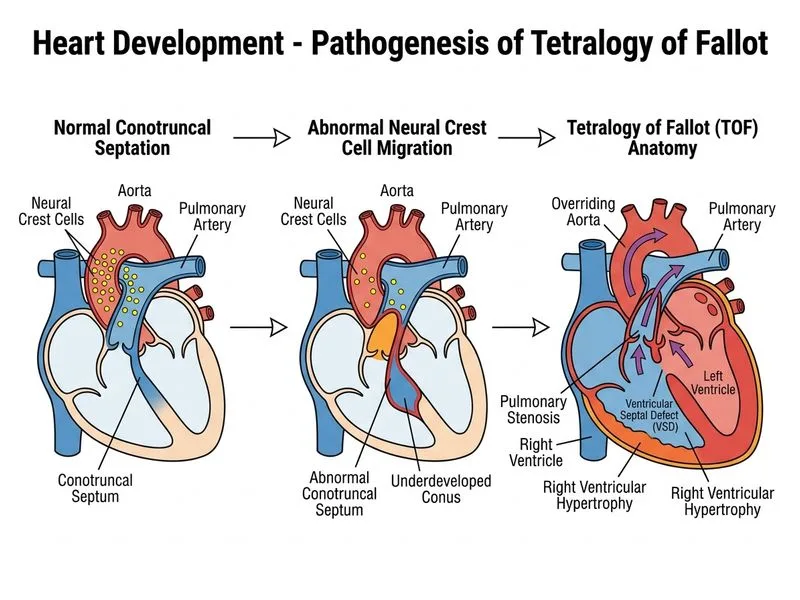
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.