## Embryological Basis of Truncus Arteriosus ### Normal Development During weeks 4–7 of embryonic development, the truncus arteriosus is divided into the aorta, pulmonary trunk, and proximal coronary arteries by the **truncoconal (aorticopulmonary) ridges**. These ridges are derived from neural crest cells and grow spirally to partition the common trunk into three separate vessels. ### Pathophysiology of Truncus Arteriosus Communis (TAC) **Key Point:** Truncus arteriosus results from **failure of the truncoconal ridges to divide the common arterial trunk** into separate aorta and pulmonary artery. This is a neural crest cell migration defect affecting the conotruncus region. ### Clinical Presentation - Cyanosis (mixing of systemic and pulmonary blood) - Poor feeding and failure to thrive - Pulmonary overcirculation (bounding pulses, wide pulse pressure) - Single S2 (single arterial valve) - Associated with 22q11 deletion (DiGeorge syndrome) in ~35% of cases ### Van Praagh Classification | Type | Pulmonary Artery Origin | | --- | --- | | A1 | Main PA arises from left posterolateral wall of trunk | | A2 | Right and left PAs arise separately from trunk | | A3 | Right PA from right lateral wall; left PA from aortic arch | | A4 | PAs arise from descending aorta | ### Management Algorithm ```mermaid flowchart TD A[Truncus Arteriosus Communis diagnosed]:::outcome --> B{Hemodynamically stable?}:::decision B -->|No/Cyanotic| C[Start PGE1 infusion]:::action B -->|Yes| D[Optimize preoperatively] C --> E[Maintain ductal patency] E --> F[Reduce right-to-left shunt] D --> G[Surgical repair: Rastelli procedure] G --> H[Separate PAs from trunk<br/>Reconstruct pulmonary circulation]:::action H --> I[Successful palliation]:::outcome ``` ### Immediate Management (Next Step) **High-Yield:** The immediate next step in a cyanotic neonate with TAC is to **initiate prostaglandin E1 (PGE1) infusion** at 0.05–0.1 µg/kg/min. **Rationale:** 1. PGE1 keeps the ductus arteriosus patent, allowing right-to-left shunting and systemic perfusion 2. Reduces the degree of mixing and improves systemic oxygen delivery 3. Buys time for preoperative stabilization and surgical planning 4. Definitive management is the **Rastelli procedure** (separation of PAs from trunk, reconstruction of pulmonary circulation, placement of conduit) **Clinical Pearl:** Do NOT give indomethacin or acetaminophen (which close the PDA) in TAC — the patent ductus is essential for survival in this condition. [cite:Robbins 10e Ch 12] 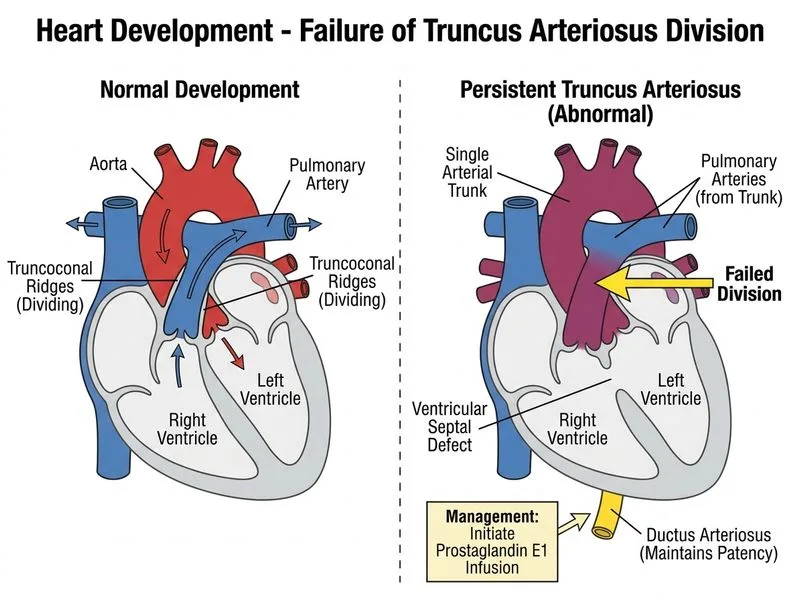
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.