## Transposition of the Great Arteries (TGA): Embryological Defect and Emergency Management ### Embryological Basis **Key Point:** TGA results from **abnormal rotation of the aorticopulmonary septum** during weeks 4–6 of development. The aorta arises from the right ventricle and the pulmonary artery from the left ventricle—the reverse of normal anatomy. ### Normal vs. TGA Anatomy | Feature | Normal | TGA | | --- | --- | --- | | Aorta origin | Left ventricle | Right ventricle | | Pulmonary artery origin | Right ventricle | Left ventricle | | Systemic circulation | Deoxygenated RV → Lungs → LV → Aorta | Deoxygenated RV → Aorta (systemic) | | Pulmonary circulation | Oxygenated Lungs → LV → Aorta | Oxygenated Lungs → LV → PA (recirculates) | | Survival | Normal | Requires mixing (PDA, ASD, VSD) | ### Pathophysiology in TGA with Intact VSD 1. **Two separate, non-communicating circulations** exist in parallel 2. Deoxygenated blood from systemic veins enters the right atrium → right ventricle → aorta → systemic circulation (severe hypoxemia) 3. Oxygenated blood from lungs enters the left atrium → left ventricle → pulmonary artery → back to lungs (wasted oxygenation) 4. Survival depends on **mixing** via: - Patent foramen ovale (PFO) - Patent ductus arteriosus (PDA) - Ventricular septal defect (VSD) ### Clinical Presentation - **Severe cyanosis** within hours to days of birth (SpO₂ often <70%) - Poor feeding, respiratory distress - Single loud S2 (anterior aorta) - "Egg-on-string" appearance on CXR (narrow mediastinum, decreased pulmonary vascularity) - Hyperoxia test: minimal response to 100% O₂ (distinguishes from other cyanotic heart disease) ### Emergency Management Algorithm ```mermaid flowchart TD A[TGA diagnosed<br/>Severe cyanosis]:::urgent --> B[Start PGE1 infusion]:::action B --> C[Keep ductus arteriosus patent]:::action C --> D{Adequate mixing?}:::decision D -->|No| E[Balloon Atrial Septostomy<br/>Rashkind procedure]:::action D -->|Yes| F[Stabilize, prepare for surgery] E --> G[Create ASD<br/>Improve LA-RA mixing]:::action G --> H[Improve systemic oxygenation] H --> I[Definitive: Arterial Switch<br/>Operation within 48-72 hrs]:::action I --> J[Restore normal anatomy]:::outcome ``` ### Immediate Next Step: Balloon Atrial Septostomy (Rashkind Procedure) **High-Yield:** In a cyanotic infant with TGA and inadequate mixing, the **immediate next step is Balloon Atrial Septostomy (BAS)** to enlarge the foramen ovale and allow right-to-left shunting at the atrial level. **Procedure Details:** 1. A balloon-tipped catheter is advanced through the femoral vein into the right atrium 2. The balloon is inflated in the left atrium and rapidly withdrawn, tearing the atrial septum 3. This creates a large ASD, allowing oxygenated blood from the left atrium to mix with deoxygenated blood in the right atrium 4. Improves systemic oxygenation from ~65% to ~75–80% (temporary measure) **Clinical Pearl:** BAS is performed **at the bedside** in the ICU or catheterization lab and provides immediate hemodynamic improvement while the infant is being prepared for definitive arterial switch operation (ASO). **Concurrent Medical Management:** - **Prostaglandin E1 (PGE1)** infusion to maintain PDA patency - Avoid high FiO₂ (paradoxically increases pulmonary blood flow, worsening systemic hypoxemia) - Maintain mild acidosis and hypothermia to reduce pulmonary vascular resistance ### Definitive Treatment **Arterial Switch Operation (ASO)** within 48–72 hours: - Transect the aorta and pulmonary artery - Reanastomose them to their correct ventricles - Relocate coronary arteries to the neoaorta - Success rate >90% in experienced centers [cite:Robbins 10e Ch 12; Harrison 21e Ch 282] 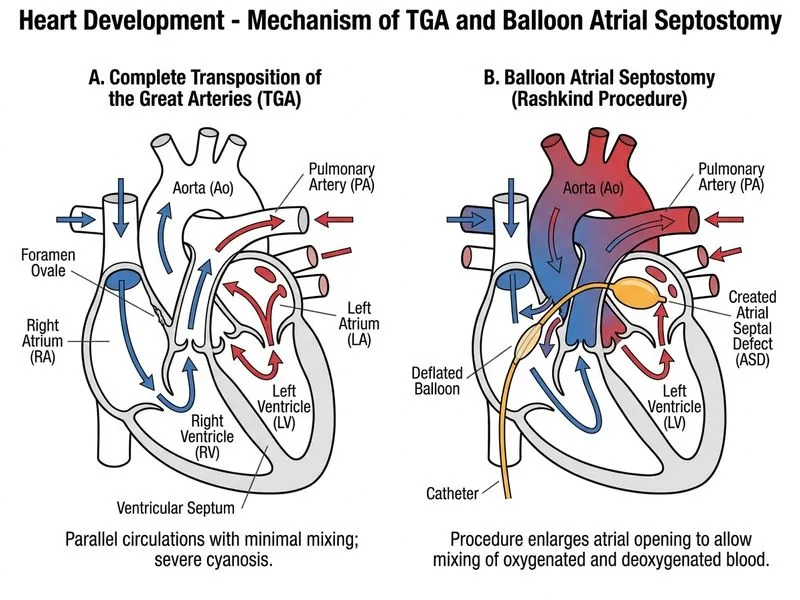
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.